History of SSA During the Johnson Administration 1963-1968
APPENDIX E- PRINCIPAL CHANGES IN MEDICARE MADE BY THE 1967 AMENDMENTS
Payment for Physicians' and Other Medical Services May Be Made on
Unpaid Bills
If no assignment is taken, medical insurance payments may now be
made directly to the patient on the basis of an itemized bill--even
though it has not been paid. There is no change in the assignment
method under which physicians and suppliers may have payment made
directly to them. This new provision applies to all bills received
or processed by carriers on or after January 2, 1968 (the date of
enactment) even though the services were rendered before that date.
Time Limit for Filing Medical Insurance Bills (Paid or Unpaid)
In order for payment to be made on a bill it must be submitted before
December 31 of the year following the year in which services are
received. For purposes of this rule, services received in the last
3 months of a calendar year are counted as received in the following
year; thus, bills for such services may be submitted until December
31 of the second year after the year in which services were actually
received.
A special extension permits bills for covered services received
in July, August, or September, 1966, to be submitted until March
31, 1968.
Elimination of Certain Physician Certifications
Physician certification of medical necessity for virtually all outpatient
hospital services and admissions to general hospitals has been eliminated.
The provision applies to admissions and to outpatient services furnished
on and after January 2, 1968. The first certification for inpatient
services in a general hospital will now be required as of the 14th
day of services. Initial certification is still required for admissions
to psychiatric and tuberculosis hospitals and to extended care facilities.
Additional Inpatient Hospital Benefit Days (Effective January
1, 1968)
Each hospital insurance beneficiary will have a "lifetime reserve"
of 60 additional days of inpatient hospital coverage. These additional
days can be used at the patient's option whenever the 90 days covered
in a "spell of illness" have been exhausted, and are subject
to $20 a day coinsurance. This benefit is not renewable; the number
of days in a beneficiary's "lifetime reserve" is permanently
reduced by the number of days used.
NOTE: If the beneficiary is an inpatient of a participating
hospital on January 1, 1968, and has previously exhausted his inpatient
hospital benefits, the lifetime reserve days can be drawn on immediately.
Full Reimbursement of Radiology and Pathology Services to Hospital
Inpatients (Effective April 1, 1968)
Payment of the full reasonable charges may be made under medical
insurance for radiology and pathology services furnished by physicians
to inpatients of participating hospitals. The $50 annual deductible
does not have to be met. Thus, because there will rarely be any
patient liability for these services, medicare reimbursement procedures
can be greatly facilitated and the patient can frequently be left
out of the process completely.
Under this provision, it will also be possible to pay for radiology
and pathology services to hospital inpatients in a manner that is
more consistent with the usual billing procedures of many hospitals
and the manner in which these services are reimbursed by most other
health insurance programs. Where the hospital customarily bills
for both the hospital's services and the services of the pathologists
and radiologists, the absence of the medical insurance deductible
and coinsurance will now make it unnecessary to break down the bill
on a patient-by-patient basis into the parts covered under the hospital
insurance and medical insurance programs, since this can be done
on an aggregate basis. Thus, where the total services are billed
through the hospital, the provision would provide opportunities
for the development of hospital billing procedures that will greatly
reduce paperwork and facilitate administration.
Inclusion of All Outpatient Hospital Benefits Under Medical Insurance
(Effective April 1, 1968)
This provision consolidates all covered outpatient hospital services
under the medical insurance program. Thus, there will be only a
single deductible and coinsurance applied to all covered outpatient
hospital services (the $50 annual medical insurance deductible and
20 percent coinsurance), and no need to separate diagnostic from
therapeutic services as in the past, for allocation of costs and
charges to different parts of the medicare program.
Also, effective April 1, 1968, hospitals may, in situations to be
described in forthcoming regulations, collect an outpatient charge
of $50 or less from the beneficiary. This provision will simplify
hospital collection processes in situations where the hospital cannot
readily determine whether the patient has met the deductible, and
he is able to pay the bill at the time services are rendered. Where
such collections are made, the beneficiary would ordinarily receive
the medical insurance reimbursement on the basis of a claim prepared
on his behalf by the hospital. Payments to the hospital will be
periodically adjusted to assure that total hospital reimbursement
for outpatient services does not exceed what the hospital would
have received if it had submitted all bills on a cost reimbursement
basis.
Payment for Additional Outpatient Physical Therapy Services (Effective
July 1,1968)
At present, physical therapy services are covered when furnished
under the direct supervision of a physician or to homebound patients
under a home health plan. Effective July 1, 1968, physical therapy
services will also be covered under the medical insurance program
when furnished by qualified providers of services or others under
arrangements with, and under the supervision of, such providers.
For purposes of this additional coverage, the term "providers
of services" includes approved clinics, rehabilitation agencies
and public health agencies. In order for payment to be made for
such services, a physician must certify that the patient requires
physical therapy services on an outpatient basis, and is under a
plan of treatment established and periodically reviewed by a physician
which prescribes the type, amount, and duration of the services.
The patient does not need to be confined to his home.
Payment under Medical Insurance for Certain Ancillary Services
Not Payable Under Hospital Insurance (Effective April 1, 1968)
Under this provision, payment can be made under medical insurance
for certain ancillary services furnished by a hospital or extended
care facility for which no payment can be made under hospital insurance.
This provision would apply, for example, where a patient has exhausted
his hospital insurance eligibility or where an extended care facility
patient has not met the prior hospitalization requirement. These
benefits are subject to the $50 deductible and 20 percent coinsurance.
Inclusion of Certain Podiatrists' Services and General Exclusion
of Specified Foot Care Services (Effective January 1, 1968)
Services of doctors of podiatry or surgical chiropody are covered
under the medical insurance program as physicians' services, but
only with respect to functions which they are authorized to perform
by the State where they practice. However, certain specified foot
care services will now be excluded whether performed by a podiatrist
or medical doctor. These exclusions include treatment of flat foot
conditions, the prescription of supportive devices for such conditions,
treatment of subluxations of the foot, and routine foot care (including
cutting or removal of corns, warts or callouses, trimming of nails
and other routine hygienic care).
Specific Exclusion of Eye Refractions
All procedures performed during any eye examination on and after
January 2, 1968, to determine the refractive state of the eyes (even
in connection with furnishing prosthetic lenses) are now excluded
from coverage. The exclusion applies whether the refractions are
performed by ophthalmologists, other physicians, or optometrists,
and even though the total examination is for the treatment or diagnosis
of eye disease or injury.
Payment for Purchase of Durable Medical Equipment (Effective
January 1, 1968)
In addition to payment for rental, payment can also be made for
purchase of durable medical equipment by or for an individual. Except
for inexpensive items, payment will be made periodically in the
same amount as if the equipment were rented, but only for the period
of time that the equipment is medically necessary or until the purchase
price has been met, whichever occurs first.
Payment fof Portable X-Ray Services (Effective January 1, 1968)
Payment will be made for diagnostic X-ray services furnished in
the patient's home or other place of residence. These services will
be covered under medical insurance if they are provided under the
general supervision of a physician and if they meet health and safety
regulations.
Blood Deductibles (Effective January l, 1968)
Under this provision, the definition of "blood" is broadened
to include packed red blood cells as well as whole blood. A 3-pint
blood deductible will now also apply to the medical insurance program
for blood furnished during a calendar year in connection with services
covered by that program. This deductible is separate from the 3-pint
blood deductible for each "spell of illness" in the hospital
insurance program, and neither can be used to meet the other.
Payment for Services Furnished to Inpatients of Non-Participating
Hospitals
Under this provision, partial payment may be made for inpatient
emergency or non-emergency services furnished by certain non-participating
hospitals between July 1, 1966, and January 1, 1968, and for emergency
inpatient services furnished by certain non-participating hospitals
in respect to admissions on or after January 1, 1968. A facility
is considered a hospital under this provision if it is licensed
as a hospital, has a full-time nursing service and is primarily
engaged in furnishing medical care under the supervision of a doctor
of medicine or osteopathy. Hospital insurance will pay 60 percent
of the room and board charges and 80 percent of other charges for
covered services after the usual deductibles are met. These benefits
are limited to 20 days if the hospital does not qualify to take
part in medicare, but if the hospital begins to participate in medicare
before January 1, 1969, and applies its utilization review plan
to the services rendered, the full duration of hospital insurance
benefits can apply.
Incentive Reimbursement Experimentation
The Secretary of Health, Education., and Welfare is authorized to
experiment with alternative methods of reimbursement to organizations
and physicians under the medicare, medicaid and child health programs.
The experiments would test various incentives for increasing the
efficiency and economy of health services without adversely affecting
the quality of care. Experiments may involve only those physicians,
institutions, and organizations that agree to participate and may
not be initiated until the Secretary obtains the advice and recommendations
of specialists competent to evaluate the possibility of securing
productive results.
Advisory Council Study of Health Insurance for the Disabled
An advisory council, to be appointed in 1968, will study the question
of providing health insurance protection for the disabled under
Title XVIII. The council will make its recommendations to the Secretary
not later than January 1, 1969.
Changes in Reduction of Benefit Days for Psychiatric end Tuberculosis
Treatment (Effective January 1, 1968)
Any inpatient days in a psychiatric or tuberculosis hospital in
the 90-day period before his hospital insurance coverage began have
previously counted against a beneficiary's days of coverage during
his first "spell of illness." This provision has been
modified as follows:
1. The reduction will not apply to tuberculosis hospitals.
2. The provision no longer prevents payment for inpatient services
in a general hospital unless the services are primarily for the
diagnosis or treatment of mental illness and the spell of illness
began in a psychiatric hospital.
3. The applicable period prior to hospital insurance eligibility
has been extended from 90 to 150 days to reflect the new lifetime
reserve of 60 additional inpatient hospital days.
Health Insurance Benefits Advisory Council
The 1967 amendments expand the responsibilities of the Health Insurance
Benefits Advisory Council to include reviewing the utilization of
services under medicare and making recommendations for program changes.
Study of Drug Proposals
The Secretary will study a proposal to establish quality and cost
standards for drugs for which payment is made under the Social Security
Act, and a proposal to cover drugs under the medical insurance program.
He is required to report his findings and recommendations to the
President and the Congress by January 1, 1969.
Coverage of Services of Additional Health Practitioners
The Secretary will study the need for extension of coverage under
the medical insurance program to the services of additional types
of licensed practitioners performing health services in independent
practice. He will make recommendations to the Congress prior to
January 1, 1969.
Hospital Insurance Eligibility
Individuals reaching age 65 prior to 1968 were eligible for hospital
insurance benefits, under a "transitional insured status"
provision, even though they did not have any social security work
credits. Under the new law, people who reach 65 in 1968 and are
not entitled to monthly social security or railroad retirement benefits
will need 3 calendar quarters--about 3/4 of a year--of social security
work credits, in order to be eligible for hospital insurance.
For people who reach 65 after 1968, the amount of work credits needed
increases by 3 quarters each year--6 quarters will be needed by
those who reach 65 in 1969, 9 by those who reach 65 in 1970, and
so on. Eventually the amount of work required for hospital insurance
protection will be the same as that required for monthly cash benefits.
However, a person who qualifies for monthly benefits as the dependent
or survivor of an insured worker will not need any work credits.
Medical Insurance Enrollment
Changes were also made in the provisions for medical insurance enrollment.
A person who is not enrolled for medical insurance may enroll during
the first 3 months of any year, provided this period begins within
3 years after he had his first opportunity to enroll. People already
65 or older who do not have medical insurance may enroll through
April 1, 1968; if they do not enroll by that date, they will have
to wait until 1969 for another opportunity to do so.
A person who is enrolled for medical insurance may give notice
of his intention to drop the insurance at any time. The notice is
effective at the end of the next calendar quarter (except for notices
received on or before April 1, 1968, which are effective on that
date). He may re-enroll during the first 3 months of any year, but
only if he does so within 3 years after his coverage is terminated.
Financing Hospital Insurance
The favorable actuarial balance of 0.74 percent of payroll that
the social security program has is sufficient to finance a substantial
part of the cost of the cash benefit provisions in the new law.
The remaining cost of the cash benefit increases and the income
required to assure an adequate financing base for the hospital insurance
program will, be secured through: (1) an increase in the contribution
and benefit base from $6,600 to $7,800 (effective January 1, 1968),
and (2) revised contribution rate schedules for the cash benefits
and hospital insurance parts of the program. There will be no increase
in the total contribution rate for 1968. The ultimate contribution
rate for cash benefits will be increased from 4.85 percent to 5.0
percent beginning in 1973 and the ultimate rate for hospital insurance
will be increased from 0.80 percent to 0.90 percent beginning in
1987.
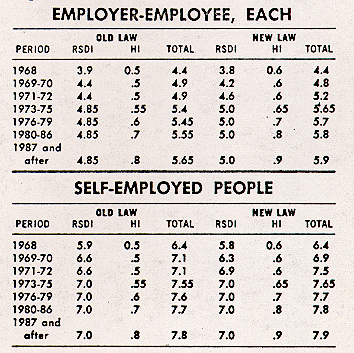
The tables below compare the contribution rates under the old and the new law. For each they show the percentage for retirement, survivors, and disability insurance and the percentage for hospital insurance: