Addressing the Challenges Facing SSA's Disability Programs
Social Security Bulletin, Vol. 66, No. 3, 2005/2006 (released August 2006)
An outline of the current initiatives—for example, the implementation of the Ticket to Work program and various demonstration projects designed to promote work resumption—undertaken to address the challenges facing SSA's disability programs. The article also contains a summary of the agency's efforts to enhance the efficiency of its administration of the disability programs, including the establishment of an eDib electronic disability folder and the creation of a workgroup to consider ideas for simplifying the SSI program.
Contributors to this article include Mark Green, Barry Eigen, John Lefko, and Scott Ebling. All contributors are with SSA's Office of Disability and Income Security Policy.
Contents of this publication are not copyrighted; any items may be reprinted, but citation of the Social Security Bulletin as the source is requested. The findings and conclusions presented in the Bulletin are those of the authors and do not necessarily represent the views of the Social Security Administration.
Introduction
Social Security is much more than a retirement program. For 50 years, the Social Security Disability Insurance (SSDI) program has protected workers and their families by providing cash benefits to individuals who are unable to work because of severe disabilities. SSDI also provides disability benefits to disabled widows and widowers of workers who are at least 50 years old and to children who have been disabled since before they were 22 years old; both of these benefits provide support to workers and their families, guaranteeing that there will be financial support when the workers are gone or no longer able to provide this support themselves. In addition, the Social Security Administration (SSA) administers a program called Supplemental Security Income (SSI), which pays benefits to both adults and children with severe disabilities who have limited means.
Both SSDI and SSI also provide access to programs that provide assistance with medical expenses to individuals with disabilities. Individuals entitled to SSDI benefits can become entitled to Medicare, and in most States individuals who are eligible for SSI are also eligible for Medicaid. In all, over 11 million Americans with disabilities receive a disability benefit from Social Security.
The definition of disability in the Social Security Act is strict, and the rules for determining disability are complicated. Applying for disability benefits can be a difficult experience for individuals with disabilities, not only because of the complexities of the program but also because of their disabilities. Claimants may be anxious as they wait for a decision in their case and worry about whether they have provided all the information needed to make a decision. While many individuals qualify within only a few months after they apply, others go through an appeals process which can continue for years before they qualify. Individuals who do not qualify often do not understand why they were denied and are not sure whether they should appeal their claims.1
The SSDI and SSI programs have grown in size and complexity since their inception. There has been some variability in the number of applications received over the years; however, since 2000 there has been a steady rise every year in the total number of applications.2 In Fiscal Year (FY) 2000, SSA received over 2.1 million claims for disability benefits. By FY 2005, SSA had received over 2.6 million claims for disability benefits, and the number of applications is expected to increase as baby boomers move into their more disability-prone years.
The factors involved in determining disability claims have also changed. In the early years of the SSDI and SSI disability programs, most individuals qualified because they had medical conditions that were included in the Listing of Impairments (the listings), a list of physical and mental medical conditions included in the regulations that are used to award the most obviously disabled individuals.3 Early in the program only a minority of individuals who qualified as disabled did so based on the more complex rules for establishing disability. These rules consider the functional effects of the individual's medical conditions on their ability to work together with their vocational factors of age, education, and work experience. Over the years, these proportions have been changing gradually but steadily so that the proportion of individuals who qualify under the listings is lower each year and the proportions who qualify based on their functional capacity and vocational factors are higher. There are many reasons for this change, but one is that medical science and treatment have improved dramatically over the years so that it is no longer appropriate to presume disability in some individuals who formerly would have been awarded under the listings. Another reason is that the percentage of claims involving mental impairments and combinations of physical and mental impairments has increased dramatically over the years. These claims are more complex and difficult to adjudicate.
The 2.6 million new applications for disability benefits that SSA processed in FY 2005 are only part of the total disability workload. Many appeals of disability claims are also processed; for example, in FY 2005, administrative law judges (ALJs) in SSA's hearing offices processed over 500,000 appeals of disability claims. In addition, the cases of people who receive disability benefits are also reviewed to ensure that they continue to qualify; in FY 2007, it is expected that 1.6 million of these continuing disability reviews will be processed.
In FY 2005, SSA made payments to approximately 6 million disabled workers and more than 5 million blind and disabled SSI beneficiaries. For a number of years, those Social Security beneficiaries that wanted to work sought assistance from State vocational rehabilitation (VR) agencies. However, few beneficiaries used the services and successfully returned to work. Additionally, certain policies and procedures also acted as disincentives and prevented people from attempting to work. While the enactment of legislation in 1999 that was intended to provide greater employment opportunities for individuals with disabilities provided some relief for disabled beneficiaries wanting to return to work, experience with the program demonstrated that additional efforts were needed to develop a comprehensive strategy of work incentives to increase the employment options for disabled individuals.
As the disability programs have grown in both size and complexity, SSA has been challenged to provide the high quality of service that disabled claimants and the public expect and deserve. Over the last five years, SSA has implemented a number of initiatives intended to fundamentally improve the administration of the disability program by improving the accuracy, consistency, and fairness of the disability determination process; to make the right decision as early in the process as possible; and to assist disabled individuals who want to work to do so. To accomplish these objectives, SSA has made important institutional improvements to better support the disability programs and has strengthened the disability determination process through structural and qualitative changes. This paper will describe some of the important recent improvements that SSA has made including implementing a new electronic disability system; establishing a new administrative review process for deciding disability claims; updating disability policies and strengthening the ability to address policy issues; and implementing a comprehensive work opportunity initiative.
Electronic Disability (eDib)
Processing cases in paper folders requires considerable work and expense that is not only inefficient but no longer necessary with modern technology. A substantial part of the time needed to adjudicate a disability case is actually spent locating lost folders, mailing folders between offices and requesting and waiting for medical evidence to be sent. Other actions required by paper folders are also unnecessary and redundant, such as re-entering a claimant's name and Social Security number by hand every time a new form must be completed. There is also a risk of lost or damaged folders and lost evidence whenever paper folders and mail must be moved from place to place. Clearly, it is no longer appropriate or efficient to continue to process this enormous caseload in this way, and it is critical that SSA move toward using technology in order to improve the timeliness and accuracy of disability case processing.
Therefore, since 2001 SSA has speeded its efforts to change from a paper process to an entirely electronic disability process, called eDib. The eDib process is the foundation for many of the other major improvements that SSA is making, including the new Disability Service Improvement (DSI) rules described below. As a result of eDib, the traditional paper disability folder is replaced by an electronic folder that stores the documentation for the disability claim. It contains documentation to support all stages of the disability claims process, from the application through all appeals, and in the near future will include continuing disability reviews.
The eDib process starts with the application for disability. Individuals are now able to file a claim for disability benefits either by using the Internet or by contact with a Social Security office. SSA has taken over 500,000 disability claims over the Internet since the process first began in August 2002. Forms that were once printed and signed by hand are created and stored electronically. All of SSA's 1,338 field offices are now using the Electronic Disability Collect System, taking 20,000 claims per day. This process enables a field office to immediately transfer a disability claim to a Disability Determination Service (DDS), thus avoiding delays. When a claim is transferred from the Social Security field office to the appropriate DDS, the data that was collected during the field office interview is automatically shared with the DDS. It is no longer necessary to reenter data at the DDS or at other levels of adjudication and with each action an adjudicator takes because the data is automatically propagated into the claim.
Medical and other evidence that is received in electronic form goes directly into the electronic folder. Evidence that is received in paper form is scanned and added to the electronic folder. A free, easy-to-use website called Electronic Records Express has been developed for medical providers who can create and securely submit their information electronically by scanning their paper records or creating an extract of their electronic records. Medical providers who perform consultative examinations can also use the service, which also provides an option for teledictation and the facility for the provider to sign the report electronically.4
The contents of the electronic folder can be accessed by SSA field office staff, quality assessment reviewers, and State and Federal adjudicators from anywhere in the country. It also enables more than one employee or component to work on a claim at the same time, thus expediting the processing of the claim. It provides greater flexibility, protects against lost or damaged folders, and also protects the confidentiality of claimant information.5 This process also improves the ability to track and manage workloads and enhances the ability to electronically conduct business with the public by providing online options for filing for disability benefits and submitting medical and other evidence.
Implementation of the electronic disability folder began in January 2004. As of January 31, 2006, all of the State DDSs had begun using electronic disability folders, and more than half were working new claims in a completely electronic environment. To ensure that each State is able to process disability cases in a fully electronic environment SSA began a certification process in January 2005, called the Independence Day Assessment (IDA). Once a State has been IDA certified, electronic folders processed by that State become the official record of the Agency's actions on the disability case. Currently, 45 States and territories have been certified, and all remaining States and territories will be certified by the end of calendar year 2006. SSA's hearing offices began a similar certification process in September 2005 which will continue through early 2007 as additional hearing offices begin to process appeals in a completely electronic environment. By the end of 2006, each of the DDSs and the hearing offices are expected to be using electronic folders on a regular basis. Claims are being adjudicated more effectively and efficiently because of this streamlined process, and this flexibility affords SSA a new opportunity to make changes to improve the administrative efficiency of the disability program.
Disability Service Improvement (DSI)
On March 31, 2006, the Commissioner published final rules to implement a new disability determination process called Disability Service Improvement (DSI).6 The new process is designed to improve the accuracy, consistency, and timeliness of disability decision-making throughout the administrative review process. DSI is expected to significantly reduce average disability determination processing time, increase decisional consistency and accuracy, and ensure that the right decision is made as early in the disability determination process as possible. The DSI process will help to ensure that individuals who are clearly disabled receive determinations within 20 calendar days of the date the DDSs receive their applications for benefits. The final rules also facilitate greater accountability for the quality of disability determinations at every step of the process.
The new rules are the result of collaborative discussions that began when the Commissioner of SSA first presented her ideas to the House Ways and Means Subcommittee on Social Security in 2003. The Commissioner personally met with hundreds of professional organizations, advocates, members of Congress and congressional staff, as well as Social Security and State employee groups.
The DSI process includes many innovations and specific changes from the current disability determination process. Some of the major changes that are described in the new rules include the following:
- The regulations establish a "quick disability determination" (QDD) process for individuals who are clearly disabled. Under the QDD process, a predictive model will identify claims that involve a high potential that the claimant is disabled and that evidence of the claimant's allegations can be easily and quickly obtained. These claims will be automatically referred from the SSA field office to QDD units in the DDSs whose function will be to process QDD claims within the 20-day time limit.
- The regulations also establish a Medical and Vocational Expert System (MVES) consisting of a Medical and Vocational Expert Unit and a national network of medical, psychological and vocational experts who meet qualification standards required by the Commissioner. These experts will be able to provide the best possible and most appropriate medical and vocational expertise for adjudicators at each level of the disability decision-making process.
- The regulations eliminate the reconsideration step of the administrative review process and establish instead a Federal Reviewing Official to whom individuals who are dissatisfied with their initial determinations can appeal. Under the new procedures, the decision will be made by a Federal employee who will be an attorney and a specialist in disability adjudication.
- The regulations eliminate the claimant initiated appeal of an ALJ's disability decision to the Appeals Council. Individuals who do not agree with a final ALJ decision may now appeal directly to Federal district court. However, a new Decision Review Board will be established to identify and review the most problematic and error prone ALJ decisions, both favorable and unfavorable, and will be able to focus on promptly identifying decision-making errors that, when corrected, will improve decision-making at all levels of the disability determination process.
Other changes in the DSI rules are also intended to strengthen the quality of the decisions at all levels and make technical changes related to the submission of evidence.
The new regulations are effective for individuals who reside in the states in the Boston region (New Hampshire, Maine, Vermont, Connecticut, Massachusetts, and Rhode Island) for initial SSDI and SSI disability claims filed beginning August 1, 2006. As SSA gains experience with these changes, the DSI process will be gradually implemented in other regions.
Improvements in Policymaking–Listing of Impairments
There are two ways that an individual can be found disabled under SSA's rules:
- By having a physical or mental condition(s) that is in the Listing of Impairments (the listings) or that is medically equal in severity to a listed condition, or
- By showing an inability to work based on a consideration of the functional effects of the individual's medical condition(s) and considering the individual's vocational factors of age, education, and work experience.7
The Listing of Impairments (the listings) is a set of medical evaluation criteria in the Social Security regulations that describes physical and mental conditions that are so severe that it is presumed that individuals whose medical conditions meet or equal their criteria are disabled regardless of their age, education, or work experience. The listings are arranged by body system (for example, musculoskeletal, cardiovascular, and mental disorders) and include both diagnostic and severity criteria.
Since the beginning of the disability program, SSA has used listings to more quickly identify individuals who are clearly disabled. However, no comprehensive update of the listings has taken place for many years. While some body systems were updated in the early 1990's, others date back to the 1980's and some even earlier. As a result, many of the listings do not reflect recent advances in medicine. In addition, experience in using the listings in adjudication suggests changes that should be made to ensure that the listings both appropriately identify individuals with disabilities and that they are able to be understood and applied uniformly by all adjudicators.
Therefore, all of the body systems in the listings are being updated. Since 2004, SSA has published final rules revising the body systems for cancer,8 kidney disease,9 cardiovascular diseases,10 skin disorders,11 and impairments that affect multiple body systems (such as Down syndrome).12 Final rules have also been published that update the regulations that explain how to use the listings.13 In addition, SSA has published Notices of Proposed Rulemaking (NPRMs) asking for public comment on proposed revisions to the vision14 and digestive disorders15 listings and an NPRM that will allow adjudicators to rely on evidence from optometrists in making disability determinations for all eye disorders.16 SSA plans to finish updating all of the listings within the next two to three years.
Since 2003, SSA has also made a significant change in how proposed changes to the listings are developed. Through "advance" notices of proposed rulemaking and public outreach meetings, SSA is actively soliciting the comments and expertise of the public, medical professionals, and advocates for people with disabilities before deciding what revisions to propose in the listings. These methods have provided policymakers not only additional expert input that might not otherwise have been available, but also insights into how the rules are understood and applied and how they could be improved from the perspective of the people who are affected by them. This process has greatly improved the quality of the proposed changes and will result in better final rules.
Addressing Complex Policy Issues–Disability Program Policy Council (DPPC)
Administering the SSDI and SSI disability programs has presented many challenges. Resolution of conflicts in the disability decision-making process has oftentimes been stalled due to dispersion and lack of coordination among the various program policy and legal components throughout SSA. Experience has shown there is a critical need for policy consistency among all adjudicatory levels as well as the need to clarify existing regulations and procedures, promulgate Social Security rulings into regulations, and eliminate existing regulations that add little or no value. Recognizing the necessity for a more integrated approach in addressing policy issues, the Commissioner has established a new Disability Program Policy Council (DPPC). The Council, chaired by the Deputy Commissioner for Disability & Income Security Programs, is a forum for addressing disability policy issues aimed at improving SSA's disability programs by allowing disability decision makers to raise complex or controversial policy issues for discussion in a collaborative fashion and make policy recommendations for consideration by the Commissioner.
Implementing A Comprehensive Work Opportunity Initiative
Expanding employment opportunities for disabled beneficiaries has been a priority for SSA. For a number of years SSA has supported demonstrations and projects intended to address the broad needs of beneficiaries with disabilities. These projects can lead to ways to better serve individuals with disabilities including potentially changing program rules to allow for better coordination among other federal and state programs. SSA also receives funding for projects through specific congressional mandates. These projects support specific program changes or outreach activities targeted to populations in particular need.
In recent years, SSA has implemented a variety of work incentives, including the Ticket to Work and Self Sufficiency Program (the Ticket Program), intended to provide disabled beneficiaries greater flexibility and expanded choice in obtaining the rehabilitation, employment and other support services that they need to go to work and attain their employment goals. In February 2001, SSA received additional support from President Bush by the creation of the New Freedom Initiative, a comprehensive government-wide program whose primary goal is to promote the full participation of individuals with disabilities in all areas of society, including the expansion of educational and employment opportunities for disabled beneficiaries. Among the major components of the New Freedom Initiative are two that are most relevant to SSA's goal of improving work opportunities for individuals with disabilities:
- Integrating Americans with disabilities into the workforce, and
- The swift implementation of the Ticket Program, a law passed in December 1999 that gave people with disabilities the ability to choose their own support services and maintain health benefits when they return to work.
SSA's Comprehensive Work Opportunity Initiative seeks to address the multiple barriers faced by disabled beneficiaries who wish to return to work and covers two major areas: immediate projects and demonstration projects.
Text description for chart titled
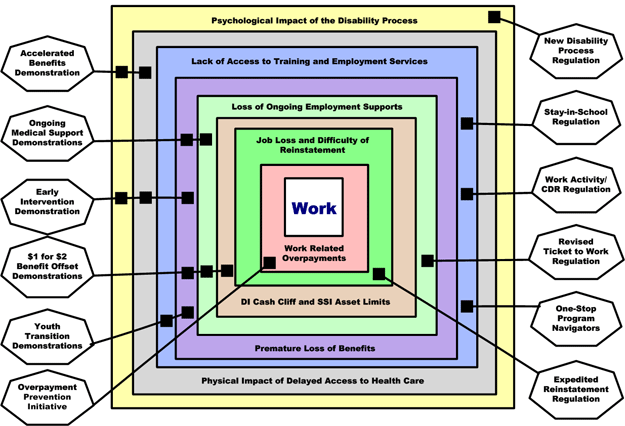
The Comprehensive Work Opportunity Initiative: Overcoming Multiple Barriers to Employment
This diagram is captioned "A variety of strategies are needed in order to overcome the multiple barriers to employment—regulatory changes and possible statutory changes, which can be assessed through a variety of demonstration projects."
The chart shows eight concentric squares, each representing an obstacle to employment; and twelve labeled balloons, each representing a component of the Comprehensive Work Opportunity Initiative, linked to the obstacle or obstacles it addresses.
Each obstacle is listed below, with the relevant components noted.
Obstacle 1: Psychological impact of the disability process.
Relevant components:
- Accelerated benefits demonstration,
- Early intervention demonstration,
- New disability process regulation.
Obstacle 2: Physical impact of delayed access to health care.
Relevant components:
- Accelerated benefits demonstration,
- Early intervention demonstration.
Obstacle 3: Lack of access to training and employment services.
Relevant components:
- One-stop program navigators,
- Stay-in-school regulation,
- Work activity/CDR regulation,
- Youth transition demonstrations.
Obstacle 4: Premature loss of benefits.
Relevant components:
- $1 for $2 benefit offset demonstrations,
- Early intervention demonstration,
- Ongoing medical support demonstrations,
- Youth transition demonstrations.
Obstacle 5: Loss of ongoing employment supports.
Relevant components:
- $1 for $2 benefit offset demonstrations,
- Ongoing medical support demonstrations,
- Revised Ticket to Work regulation.
Obstacle 6: DI cash cliff and SSI limits.
Relevant components:
- $1 for $2 benefit offset demonstrations.
Obstacle 7: Job loss and difficulty of reinstatement.
Relevant components:
- Expedited reinstatement regulation.
Obstacle 8: Work related overpayments.
Relevant components:
- Overpayment prevention initiative.
The immediate projects include regulatory and other activities that have already started or can begin in the short term. Demonstration projects are longer term activities that test various interventions that address barriers to working or returning to work. Upon completion, the most effective methods are implemented or SSA seeks the authority to implement them, if necessary. As a part of the Commissioner's DSI plan, SSA intends to conduct several demonstration projects aimed at helping people who want to work do so. These projects advance the President's New Freedom Initiative and provide work incentives and opportunities earlier in the disability determination process. Along with the Ticket Program, they are an important part of a comprehensive SSA initiative dedicated to helping people with disabilities who want to work do so to their fullest capabilities. Significant elements of the Comprehensive Work Opportunity Initiative include the following:
Ticket to Work and Work Incentives Improvement Act (Ticket Program)
The Ticket to Work and Work Incentives Improvement Act, P.L. 106-170, became law on December 17, 1999. The Act pointed out that individuals with disabilities have greater opportunities than ever for employment. This has come about through the passage of the Americans with Disabilities Act in 1990, advancements in public understanding of disability, and innovations in medical treatment, rehabilitation and assistive technology. Yet, at the time the law was passed, less than one-half of one percent of SSDI and SSI beneficiaries left the disability rolls and returned to work. The financial disincentives to work and earn income along with the lack of adequate employment training and placement services were, and continue to be, significant barriers to employment. The Ticket Program is an important component in a coordinated series of initiatives that are designed to help overcome significant barriers to employment.
The goal of the Ticket Program is to increase beneficiary choice in obtaining rehabilitation and vocational services. Most disability beneficiaries are provided a ticket that they can use to obtain services from either an employment network (EN) that has contracted with SSA to provide services under the program at no cost to the beneficiary, or from a Vocational Rehabilitation (VR) Agency. The program is voluntary; beneficiaries who decide that the program is not right for them do not have to participate, and their benefits are not affected by that decision.
The Ticket Program was phased in nationally over a three-year period. During this time, SSA mailed tickets to more than 8 million disability beneficiaries. Currently, tickets are mailed to approximately 75,000 new Ticket-eligible beneficiaries each month. As of June 16, 2006, more than 9,700 beneficiaries have chosen to use their ticket to work with an EN, and 127,638 beneficiaries are working with their VR agencies.
Providers participating in the Ticket Program as ENs can choose from two outcome-based payment methods. In one, ENs receive payment from SSA for each month the beneficiaries with whom they are working do not receive a cash benefit from SSA because of work. SSA will make up to 60 of these outcome payments for each beneficiary. Outcome payments are not related to a beneficiary's benefit amount, but are a standard amount that is a percentage of the average benefit paid to all disability beneficiaries in the previous year. Under the second payment method, ENs can receive payments for months before the beneficiary loses cash benefits if the beneficiary achieves specific milestones of earnings. Once these beneficiaries do not receive a cash benefit because of earnings, these ENs are then eligible for up to 60 outcome payments at a reduced rate. ENs must select one of the payment methods, under which SSA will make payments for all ticket holders who have agreed to work with them.
Beneficiaries also can choose to receive services from their VR Agency. The VR agencies have an additional payment option. They can elect to receive payment as an EN under one of the payment options described above. Or, they can elect to receive payment under the traditional cost reimbursement system that was in place before the Ticket program. VR agencies can make this payment method decision on a case-by-case basis.
In 2005, the Commissioner issued an NPRM proposing amendments to the current Ticket Program in order to improve the overall effectiveness of the program.17 Based upon experience in implementing the Ticket Program and comments that the current policy, which precludes further use of a ticket if VR reimbursement has been paid, is too restrictive and does not allow beneficiaries to take advantage of the full potential of the Ticket program, the NPRM provides that a beneficiary's ticket need not be assigned to a State VR agency in order for the VR agency to be paid under the cost reimbursement payment system. Beneficiaries will also be afforded protection from the initiation of a continuing disability review while receiving services from a State VR agency, providing that all the related provisions regarding timely progress are met. Payments could also be made to an EN under a Ticket to Work payment system and to a State VR agency under the cost reimbursement payment system with respect to the same beneficiary. In order to ensure that State VR agencies do not potentially receive payments under both payment systems for the same beneficiary, the NPRM provides that a beneficiary may not assign a ticket to a State VR agency if the State VR agency provided the beneficiary with services and received payment under the cost reimbursement system with respect to the services provided to the beneficiary. Having considered recommendations from the Ticket to Work and Work Incentives Advisory Panel and the Government Accountability Office, revisions to the Ticket eligibility rules were also included in the NPRM to allow beneficiaries whose conditions may medically improve to participate in the program without first requiring a continuing disability review to be conducted.18 Additional changes intended to create a greater financial incentive for EN participation were also included in the NPRM. Final regulations are expected to be published in 2006.
Benefits Planning, Assistance and Outreach (BPAO)
Another important employment support provided by the Ticket to Work Act is the Benefits Planning, Assistance and Outreach Program (BPAO). SSA awarded and maintains 114 cooperative agreements with community-based organizations in all states to provide all SSA disability beneficiaries (including transition-to-work aged youth) access to benefits planning and other assistance services. The goal of the BPAO program is to help SSA's disabled beneficiaries make better, informed choices about work and its potential effect on benefits. The projects provide each client with an individual analysis of the impact work and increased earnings might have not just on SSA benefits, but on other important benefits as well, such as Food Stamps, Medicaid and supported housing. This information is intended to allay fears about returning to work. In addition to benefits planning, the benefits specialists conduct outreach to beneficiaries and their families who potentially are eligible to participate in the many Federal and state work incentives programs. They also work with those Federal, state and private agencies and nonprofit organizations that serve beneficiaries with disabilities.
Effective September 30, 2006, the name of the BPAO program will change to the Work Incentives Planning and Assistance (WIPA) Program, reflecting an emphasis on work incentives. Benefits Specialists under the WIPA Program will be referred to as Community Work Incentives Coordinators (CWICs).
Expedited Reinstatement (EXR)
One of the greatest fears disabled beneficiaries have about returning to work is that they will lose their cash benefits and be unable to re-establish their eligibility if they have to stop work. Addressing that fear is the goal of another important provision of the Ticket to Work Act, called Expedited Reinstatement (EXR). EXR, which was effective January 1, 2001, provides former disability beneficiaries the opportunity to request to have their benefits started again without having to complete a new application if they:
- stopped receiving their disability benefits because of work;
- are no longer able to perform that work at what is described as the substantial gainful activity (SGA) level;
- have an impairment that is the same or related to the impairment that was the basis for them receiving benefits earlier; and
- make the request within 5 years from the month their benefits were terminated.
SSA must make a determination that the individual is again eligible for disability benefits. There are two important elements of this determination that ease the transition from work to cash benefits. First, it is made using the standards SSA uses to determine if a beneficiary's disability has ceased, which require that SSA establish that the individual's impairment has improved. And, while SSA is making this determination, these individuals are eligible for up to 6 months of provisional benefits, which include cash and Medicare/Medicaid coverage. Further, if SSA approves the request for EXR, eligible spouses and children of title II beneficiaries, and eligible spouses of title XVI beneficiaries, also are eligible to have their benefits reinstated.19
Demonstration Projects
Another important component of the Ticket to Work Act is that it restored SSA's title II demonstration project authority which had expired in 1996. The law gave SSA the general authority to conduct demonstration projects designed to test the impact of various changes to the law on the ability of disabled beneficiaries to work and earn more. The law also specifically directed SSA to conduct a demonstration project that tests the effect of reducing title II benefits by $1 for every $2 of earnings above a specific level. In addition, the law included a significant expansion of the scope of SSA's demonstration authority to include applicants who have impairments that might reasonably be expected to be disabling. SSA has used its demonstration authority to plan and conduct a wide range of projects under a Comprehensive Work Opportunity Initiative to better serve its disability beneficiaries. Some of the most significant demonstration projects include the following:
Benefit Offset Demonstration. As noted above, the Ticket to Work and Work Incentives Improvement Act directed SSA to conduct a demonstration project that tests the effect of reducing title II benefits by $1 for every $2 of earnings above a specific level. As the law noted, despite recent changes that have provided historic employment opportunities for the disabled, less than one-half of one percent of title II disability beneficiaries leave the benefit rolls because of work. Many beneficiaries have stated that the eligibility rules of the SSA disability program include a number of strong disincentives to work and increased earnings. Perhaps the most important of these disincentives is what is known as the "cash cliff." Under current law, title II beneficiaries are allowed a nine-month trial work period during which they can test their ability to work without losing any benefits. After this trial work period and a three-month grace period, however, beneficiaries who work at the SGA level in any month (in 2006, $860 per month) lose their entire benefit for that month. Beneficiaries also are entitled to a 36-month period after their trial work period during which they can receive benefits for months during which they do not engage in SGA. If beneficiaries work at the SGA level after that 36-month period, which is called the Extended Period of Eligibility (EPE), they lose their entitlement to cash benefits and face the eventual loss of Medicare benefits as well. (Current law provides for at least 7¾ years of Medicare coverage beyond the trial work period for beneficiaries who return to work and remain disabled.)
In September 2004, SSA awarded a contract to develop the design for a national demonstration project that will test the effects of various interventions, in combination with a benefit offset, on employment outcomes. The goal of the demonstration project is to test changes that will enable more beneficiaries to return to work and maximize their employment, earnings and economic independence. The benefit offset policy would allow beneficiaries who are participating in the demonstration to face a more gradual reduction in their benefits if they earn above the SGA amount than is currently allowed. They will be able to take advantage of the other employment supports offered, without the certainty of losing all of their cash benefits with earnings even minimally above the SGA level. Participants also will maintain their eligibility for Medicare and the other employment supports that are available to all title II disability beneficiaries.
In addition, SSA has modified this project to include a test of an early intervention strategy by focusing on disability applicants. This aspect of the project will test strategies that are designed to help disability applicants return to work rather than continue through SSA's disability application process. Applicants who participate in this component of the demonstration also will receive a wide range of employment supports, closer to the onset of their disability, in an effort to maintain their connection to the workforce and prevent dependence on public cash benefits. It is anticipated that participants will be able to enroll in early 2007.
In the interim, in August 2005, SSA initiated a pilot benefit offset project in Connecticut, Utah, Vermont and Wisconsin. In this simplified design, SSA is testing the effect of combining an offset in title II disability benefits of $1 for every $2 in earnings above the SGA amount with benefits counseling. Project participants also can take advantage of an expanded 72-month EPE. States are recruiting beneficiaries from various sources, such as the client lists from their VR agency and the local BPAO program. SSA will use the results from this pilot project to inform the national demonstration project.
Youth Transition Demonstration. In September 2003, SSA awarded cooperative agreements in six states—California, Colorado, Iowa, Maryland, Mississippi and New York—to develop service delivery systems to help youth ages 14–25 who receive either SSI or title II disability benefits, or are at risk of becoming beneficiaries. The goal of this project is to study the impact of waivers to SSI program rules and enhanced coordination of services for youth on their ability to start work or to increase earnings and achieve self-sufficiency. These projects work collaboratively with many partners, including educational institutions, VR, labor and other organizations, to build sustainable improvements in the delivery of transition services and supports for youth. These improvements demonstrate how communities can integrate services and resources to support the successful transition of youth with disabilities from high school to post-secondary education or employment with a goal of maximizing economic self-sufficiency.
Accelerated Benefits. Under current law, most title II disability beneficiaries must wait 24 months after they become eligible for cash benefits before Medicare is available to them. Accordingly, many newly entitled beneficiaries have no health insurance and therefore limited access to health care during a period of time when access to care might help improve their medical condition and increase their ability to work. Certain title II disability beneficiaries are entitled to benefits with the expectation that their impairments will improve to the point that they can return to work and leave the benefit rolls. Yet, despite that designation, the rate of return to work for these beneficiaries is relatively low. This might be the result of medical conditions that deteriorate because of the lack of treatment while these beneficiaries await their entitlement to Medicare.
The Accelerated Benefits project will provide immediate health benefits and employment supports to newly entitled title II disability beneficiaries who have impairments that are expected to improve or could possibly improve with access to appropriate health care. Project participants will be recruited at the point they are notified that they have been allowed benefits. This project is designed to determine whether the provision of health care for certain newly entitled beneficiaries will have the long term payoffs of improving their medical conditions and increasing the likelihood that they will return to work. SSA awarded the contract to implement and evaluate this project in January 2006, and enrollment is expected by the end of 2006.
Mental Health Treatment Study. The proportion of disability beneficiaries with mental disorders has grown to over one-quarter of the individuals receiving title II benefits. While most forms of mental illness are treatable, many beneficiaries with these impairments do not receive the treatment and employment support services that could help them increase their ability to work. The Mental Health Treatment Study will provide comprehensive outpatient mental health treatment to beneficiaries in 21 sites across the country who have a primary impairment of either schizophrenia or affective disorder. The study will address the impact of providing treatment, both pharmaceutical and psychotherapeutic, and/or employment supports that are not covered by other insurance, on employment outcomes. Enrollment is expected to begin in the summer of 2006.
Ongoing Medical Benefits–HIV/Auto-Immune Deficiency Demonstration. The Ongoing Medical Benefits–HIV/Auto Immune Deficiency Demonstration will provide support services and health benefits to current title II disability beneficiaries with a diagnosis of human immunodeficiency virus/acquired immune deficiency syndrome (HIV/AIDS), immune disorder and/or auto-immune disorder. Research has shown that many people within this population would like to return to work but are unable to perform their previous jobs, or are unsure about how to return to work after a period of unemployment because of their condition. Many also struggle to pay for costly medical treatment and services.
The purpose of this California-based demonstration is to provide immediate access to healthcare services and resources required for a successful return to work. The health benefits will be designed to provide beneficiaries with HIV or other immune related disorders with health coverage to ensure they receive adequate medical treatment for their impairments. Project participants also will receive employment service coordination from the California Department of Rehabilitation. Each beneficiary enrolled will be assessed to determine the types of services and/or interventions needed for a sustained and successful return to work. An Expert Medical Unit, composed of medical specialists in the HIV/auto-immune field, will be established to provide expert guidance on issues relevant to this population. Enrollment of participants is expected to begin in April 2007.
Interim Medical Benefits Demonstration. The Interim Medical Benefits Demonstration will provide health insurance coverage to certain applicants throughout the disability determination process. Eligible applicants will be those without such insurance whose medical condition is likely to improve with medical treatment or where consistent, treating source evidence will be necessary to enable SSA to make a benefit eligibility determination. Project participants will be individuals who reside in one of the states in the Boston region (New Hampshire, Maine, Vermont, Connecticut, Massachusetts and Rhode Island) where the Commissioner's new DSI adjudication process will be in effect.
State Partnership Initiative (SPI)
In 1998, under its ongoing title XVI demonstration project authority, SSA began the State Partnership Initiative (SPI) in 12 states around the country (California, Illinois, Iowa, Minnesota, New Hampshire, New Mexico, New York, North Carolina, Ohio, Oklahoma, Vermont and Wisconsin). The Rehabilitation Services Administration provided funds for similar projects in six more states. These projects were designed to help the states develop innovative statewide programs that provided employment supports to individuals with disabilities, to increase their job opportunities and their earnings. Four of the states implemented waivers to test alternative SSI rules for counting earnings and resources. The SPI projects ended in September 2004. In the four States that conducted waiver projects, SSI Waiver Demonstration participants, especially those who were not employed at intake, fared better than the general SPI participant group, but in absolute terms their employment and benefit outcomes were not large enough to have a significant impact on their economic self-sufficiency.
Disability Program Navigator (DPN)
SSA and the Employment and Training Administration in the Department of Labor (DOL) collaborated on this project that currently funds approximately 200 new positions, called Disability Program Navigators (DPNs), in 17 States. These individuals are located in DOL's One-Stop Career Centers, a key component of the reforms implemented under the Workforce Investment Act. One-Stop Career Centers are designed to deliver a full range of employment services to individuals who are seeking new jobs or careers. The DPN position is designed to add important enhancements to these services, by working to develop linkages with employers to help people with disabilities find jobs, and by serving as a resource regarding SSA's work incentives and employment supports as well as a resource to the workforce investment community.
DPNs also facilitate the transition of youth with disabilities to help them find employment and achieve economic self-sufficiency. This project is being conducted in the following States: Arizona, California, Colorado, Delaware, Florida, Illinois, Iowa, Maryland, Massachusetts, Mississippi, New Mexico, New York, Oklahoma, Oregon, South Carolina, Vermont, and Wisconsin.
Area Work Incentives Coordinator (AWIC)
In response to concerns expressed by disability beneficiaries and advocates that it was sometimes difficult to obtain accurate, consistent information from the SSA field offices regarding employment supports and work incentives, SSA undertook a major effort to increase this knowledge and awareness among its staff. The most important element of this effort was announced in 2003, when SSA created the Area Work Incentives Coordinator (AWIC) position. The 58 AWICs provide assistance to personnel in field offices on employment support and outreach issues by coordinating and conducting local public outreach on work incentives; providing, coordinating, and overseeing training for SSA personnel on employment support programs; and monitoring the disability work-related issues in their respective areas. The AWICs coordinate with the 1,335 Work Incentives Liaisons in local offices, the Public Affairs Specialists, the Plan for Achieving Self-Support Cadre members, and other personnel in order to provide improved services and information on SSA's employment support programs to assist beneficiaries with disabilities who want to start or continue working.
Conclusion
The initiatives described above illustrate that the past five years have been one of the most active periods of change and improvement in the Social Security disability programs in the 50 years since the first disability insurance benefits were paid. They are bringing the SSDI and SSI programs and policies into the 21st century both technologically and medically, providing what are hoped will be realistic, practical solutions to the problems that SSA faces in quickly, accurately, and appropriately making millions of disability decisions each year. For the first time in over 50 years, new administrative review procedures described in the Commissioner's DSI plan were developed and are being implemented in order to improve the accuracy, consistency and fairness of the disability decision-making process with the goal to make the right decision as early in the process as possible. And the various elements of the Comprehensive Work Opportunity Initiative will help SSA meet the important goal of the President's New Freedom Initiative to promote full participation of individuals with disabilities in all areas of society. While there is still a long way to go before all of these goals are fully realized, the Commissioner has set a course that will serve the disability programs well for many years to come.
Notes
1. The Social Security Act and SSA's implementing regulations prescribe rules for deciding if an individual is "disabled." SSA's criteria for deciding if someone is disabled are not necessarily the same as the criteria applied in other Government and private disability programs.
2. In January 2001, the Social Security Advisory Board referenced several possible factors for the increase in applications including unemployment rates, efforts by State and local governments to shift welfare caseloads and spending to the Federal government, court decisions, changes in regulations, and adjudicative climate. Disability Decision Making: Data and Materials.
3. The Listing of Impairments describes, for each major body system, impairments that are considered severe enough to prevent a person from doing any gainful activity (or in the case of children under age 18 applying for SSI, cause marked and severe functional limitations). Most of the listed impairments are permanent or expected to result in death, or a specific statement of duration is made. For all others, the evidence must show that the impairment has lasted or is expected to last for a continuous period of at least 12 months. The criteria in the Listing of Impairments are applicable to evaluation of claims for disability benefits or payments under both the SSDI and SSI programs. For a complete description of these criteria, see Appendix 1 to Subpart P of Part 404 contained in Title 20 of the Code of Federal Regulations.
4. "Consultative examinations" is the term that is used to describe the independent medical examinations that SSA purchases.
5. The practical benefit of processing cases electronically was demonstrated in 2005. In the aftermath of Hurricane Katrina, there was significant damage to the paper disability folders located in the New Orleans office of the Louisiana Disability Determination Services. However, 1,500 of the 5,000 cases had already been stored electronically through eDib. These records were immediately transferred to other offices to be processed.
6. 71 FR 16424 (March 31, 2006).
7. There are different rules for children who apply for disability benefits under SSI. They must show that their conditions meet or medically equal the criteria of a listing or that their impairments "functionally equal" the listings.
8. 69 FR 67038 (November 15, 2004).
9. 70 FR 38582 (July 5, 2005).
10. 71 FR 2312 (January 13, 2006).
11. 69 FR 32260 (June 9, 2004).
12. 70 FR 51252 (August 30, 2005).
13. 71 FR 10419 (March 1, 2006).
14. 70 FR 48342 (August 17, 2005).
15. 69 FR 64702 (November 8, 2004).
16. 71 FR 10456 (March 1, 2006).
17. 70 FR 57222 (September 30, 2005).
18. Individuals whose conditions may medically improve are designated as "Medical Improvement Expected" or MIE.
19. The Social Security Administration administers two programs that provide benefits based on disability: the Social Security Disability Insurance program (title II of the Social Security Act (the Act)) and the Supplemental Security Income (SSI) program (title XVI of the Act). Title II provides for payment of disability benefits to individuals who are "insured" under the Act by virtue of their contributions to the Social Security trust fund through the Social Security tax on their earnings, as well as to certain disabled dependents of insured individuals. Title XVI provides for SSI payments to individuals (including children under age 18) who are disabled and have limited income and resources. The Act and SSA's implementing regulations prescribe rules for deciding if an individual is "disabled."