Work-Related Overpayments to Social Security Disability Insurance Beneficiaries: Prevalence and Descriptive Statistics
Social Security Bulletin, Vol. 79 No. 2, 2019 (released May 2019)
We estimate the prevalence, duration, and dollar amount of work-related overpayments accrued to Disability Insurance (DI) beneficiaries based on administrative data from the Social Security Administration (SSA) for January 2010 through December 2012. We find that 1.9 percent of DI beneficiaries in our sample were overpaid because of work in 1 or more months during that period. Although overpayments were rare among DI beneficiaries overall, among those with earnings sufficient to put them at risk of a work-related overpayment, 71 percent were overpaid. Work-related overpayments lasted for a median of 9 months and accrued a median amount of $9,282. Overpayments were statistically associated with low levels of education and relatively low monthly benefit amounts. Findings for certain beneficiary and program-related characteristics suggest that modifying SSA outreach and communication efforts might help beneficiaries comply with DI earnings-reporting requirements and avoid overpayments.
Denise Hoffman is a senior researcher, Benjamin Fischer is a principal program analyst, and Andrew McGuirk is a lead data analytics developer at Mathematica Policy Research. John Jones is an economist with the Office of Research, Demonstration, and Employment Support, Office of Retirement and Disability Policy, Social Security Administration. When this article was written, Miriam Loewenberg was a senior systems analyst at Mathematica.
Acknowledgments: The authors thank Mark Trapani and Paul O'Leary of SSA, Paul Davies (formerly of SSA), and staff of the SSA Office of the Chief Actuary for their insightful comments on the manuscript. We also acknowledge contributions from David Stapleton, Aparna Keshaviah, Serge Lukashanets, and David Wittenburg at Mathematica on the research methods and manuscript. A previous version of this article was published as Disability Research Consortium Working Paper No. 2018-04 (https://www.mathematica-mpr.com/our-publications-and-findings/publications/work-related-overpayments-of-social-security-disability-insurance-beneficiaries-prevalence).
Note: The research reported herein was performed pursuant to a grant (1-DRC12000001-06-06) from the Social Security Administration funded as part of the Disability Research Consortium. Contents of this publication are not copyrighted; any items may be reprinted, but citation of the Social Security Bulletin as the source is requested.
Contents of this publication are not copyrighted; any items may be reprinted, but citation of the Social Security Bulletin as the source is requested. The findings and conclusions presented in the Bulletin are those of the authors and do not necessarily represent the views of the Social Security Administration.
Introduction
| BOND | Benefit Offset National Demonstration |
| CDR | continuing disability review |
| DAF | Disability Analysis File |
| DBAD | Disabled Beneficiaries and Dependents |
| DI | Disability Insurance |
| EPE | extended period of eligibility |
| GAO | Government Accountability Office |
| IRP | initial reinstatement period |
| MBR | Master Beneficiary Record |
| OIG | Office of the Inspector General |
| SGA | substantial gainful activity |
| SSA | Social Security Administration |
| STW | suspension or termination because of work |
| TWP | trial work period |
For decades, Social Security Administration (SSA) efforts to increase employment among Social Security Disability Insurance (DI) beneficiaries have been a focus of considerable interest among both policymakers and researchers. However, beneficiary work activity sometimes results in benefit overpayments, and research on the extent of those overpayments—and the characteristics of affected beneficiaries—has been relatively limited. A work-related overpayment occurs when SSA issues a monthly DI benefit to which an individual is not entitled because the agency either is not aware that the beneficiary has earnings exceeding the benefit-eligibility threshold for that month, or it has not yet concluded an investigation of reported earnings with benefit suspension or termination. Such overpayments can occur for several reasons, including the beneficiary's failure to report work activity timely, as required by DI rules; resource-related constraints on agency responses to reports of beneficiary work activity; and the complexity of the rules governing beneficiary work activity (Government Accountability Office [GAO] 2011, 2013, 2015). Although work activity is not the cause of all DI overpayments, this article focuses on work-related overpayments and we use the term “overpayments” in that specific context, unless noted otherwise.
DI overpayments account for a substantial sum of money and create administrative and fiscal management challenges for SSA. Work-related overpayment amounts ranged from $831 million in fiscal year 2010 to $980 million in fiscal year 2012. Over the same period, DI overpayments (including those not related to work) represented between 0.69 percent and 1.27 percent of total DI benefits paid. SSA failed to meet its benefit payment accuracy targets in all 3 years (SSA 2013a).
When SSA detects overpayments, beneficiaries are obligated to reimburse overpaid funds unless they succeed in appealing the overpayment finding or in requesting that the overpayment be waived. Overpayments can be quite large, especially when measured against the generally modest financial resources of DI beneficiaries. SSA policy is to attempt to recover the full overpayment amount immediately, but in practice, most repayments are effected through partial withholding of the monthly DI benefit once benefit payments have resumed (GAO 2016). Because the withholding is limited, full repayment can take many years. Overpayment recovery may continue after the disabled-worker benefit converts to a retirement benefit when the beneficiary reaches full retirement age. It may also result in benefit reductions for auxiliary beneficiaries (the worker's spouse and/or other dependents) and, should the beneficiary die, may be collected from surviving dependents. SSA estimates that the administrative cost of recovering overpayments for all reasons (including those not related to work) is 7 cents for every $1 recovered (SSA 2016, 132). In some cases, the overpayment is never recovered. Of the overpayment debt for all reasons identified in 2004, 53 percent was recovered, 26 percent was still outstanding, and 21 percent was waived or canceled as of February 2014 (SSA 2015, Table 4).
Anecdotal evidence suggests that overpayments and their aftermaths can be traumatic experiences for beneficiaries and may function as disincentives to work. For example, in qualitative interviews conducted as part of an assessment of SSA's Benefit Offset National Demonstration (BOND), field staff and beneficiaries reported concerns about the consequences of overpayments (Gubits and others 2013; Hoffman and others 2017). Similarly, qualitative interviews conducted with 91 beneficiaries who had recently worked at levels sufficient to trigger overpayments revealed that such overpayments were common and a source of great frustration (O'Day and others 2016). Similar findings emerged from semistructured interviews with 84 overpaid DI beneficiaries, as did reports that more than half of the interviewed beneficiaries immediately terminated employment upon learning of their overpayment (Kregel 2017). However, it is unclear if these findings are representative of the reactions of all overpaid beneficiaries.
One can easily find estimates of aggregate work-related overpayment amounts, as well as accounts of the reported frustrations of DI beneficiaries; but information on the prevalence of overpayments and the typical size of individual overpayments is scarce. In GAO (2013), the authors estimated that 0.4 percent of primary DI beneficiaries encountered a work-related overpayment over a 15-month period. However, those authors relied on sources other than Social Security administrative records, and they acknowledge that their statistics likely understate the prevalence of overpayments. An audit report by the SSA Office of the Inspector General (OIG) studied a sample of 985 DI beneficiaries in current-pay or temporary-suspension status as of October 2003. By February 2014, 3.2 percent of the sample had received a work-related overpayment at some point, with an average amount of $14,397 per overpaid beneficiary (SSA 2015). Calculations based on estimates in that report suggest that among the beneficiaries who worked at sufficient levels to be at risk of a work-related overpayment, 63 percent were overpaid. Another OIG audit report conducted case reviews of 275 beneficiaries with substantial earnings from 2007 through 2011 and revealed work-related overpayments that lasted an estimated 9 months and totaled $8,114 on average. Further, an estimated 60 of 65 beneficiaries at risk of a work-related overpayment (92 percent) were overpaid (SSA 2014). These are the best available statistics on work-related overpayments, but they were generated from relatively small samples of beneficiaries.
We have found no research that describes the characteristics of beneficiaries who encounter work-related overpayments. In general, one might expect that the likelihood of work-related overpayment is associated with beneficiary characteristics such as low levels of mental functioning or minimal contact with the SSA disability programs because those beneficiaries may have limited understanding of or exposure to DI rules on reporting work activity. Conversely, one might expect beneficiaries with high levels of education to be less likely to receive overpayments if they are better able to understand and fulfill the reporting requirements. However, these expectations are not borne out in all cases, as we describe below.
This article provides detailed statistics on the prevalence of work-related DI overpayments, the average size and duration of overpayments, and the characteristics of beneficiaries who were overpaid. We use an algorithm developed for the BOND evaluation to provide information on overpayments. We apply the algorithm to Social Security administrative data to detect overpayments. Administrative data allow us to scale our analysis more easily than we could do with the case-review data employed by other studies. In this analysis, we use a 10 percent random sample of DI beneficiaries who received or were potentially eligible for DI benefits in January 2010. We chose that starting date because SSA increased its efforts to identify overpayments at that time.
Although overpayments are rare among DI beneficiaries overall—reflecting that only a small portion of them work at sufficient levels to be at risk of a work-related overpayment—we find that overpayments are probable among at-risk beneficiaries (of whom 71 percent were overpaid). The median duration of work-related overpayments was 9 months and the median amount they accrued was $9,282. Overpayments were most prevalent among traditionally disadvantaged or vulnerable populations, including beneficiaries who are black or Hispanic, those with low monthly DI benefit amounts, those for whom medical improvement is not expected, and those with less than a high school education, holding other characteristics equal.
Background: SSA Policy Regarding Work Activity
SSA defines disability, in part, as the inability to engage in substantial gainful activity (SGA). Each year, SSA adjusts the earnings level that defines SGA based on changes in the national average wage. SGA is expressed as a monthly earnings threshold; in 2019, it is $1,220 for nonblind individuals and $2,040 for blind individuals.1 Because a condition of eligibility for DI benefits is an inability to engage in SGA, a beneficiary's earnings may affect continued eligibility. The eligibility of a beneficiary with earnings is affected in different ways in each of four stages, described below and summarized in Chart 1.
How work affects benefit eligibility for DI beneficiaries
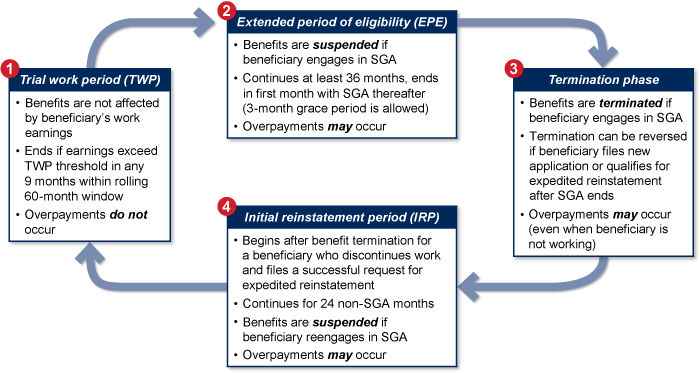
Text equivalent for Chart 1.
How work affects benefit eligibility for DI beneficiaries
- Trial work period (TWP)
- Benefits are not affected by beneficiary's work earnings
- Ends if earnings exceed TWP threshold in any 9 months within rolling 60-month window
- Overpayments do not occur
- Extended period of eligibility (EPE)
- Benefits are suspended if beneficiary engages in SGA
- Continues at least 36 months, ends in first month with SGA thereafter (3-month grace period is allowed)
- Overpayments may occur
- Termination phase
- Benefits are terminated if beneficiary engages in SGA
- Termination can be reversed if beneficiary files new application or qualifies for expedited reinstatement after SGA ends
- Overpayments may occur (even when beneficiary is not working)
- Initial reinstatement period (IRP)
- Begins after benefit termination for a beneficiary who discontinues work and files a successful request for expedited reinstatement
- Continues for 24 non-SGA months
- Benefits are suspended if beneficiary reengages in SGA
- Overpayments may occur
- The trial work period (TWP) enables a DI beneficiary to test her or his ability to work. During the TWP, work activity has no effect on receipt of DI benefits. The TWP consists of the first 9 months within a rolling 60-month window in which earnings have exceeded an annually adjusted monthly threshold ($880 in 2019).
- The extended period of eligibility (EPE) immediately follows the TWP and lasts at least 36 consecutive months. During the EPE, beneficiaries are ineligible for DI benefits in any month in which they engage in SGA, except for a grace period comprising the first month of SGA and the following two months. Benefits not paid under these circumstances are said to be “suspended for work,” and benefits resume if SGA ends. Work-related overpayments can occur in the EPE when a beneficiary engages in SGA, thereby meeting the conditions for which benefits should be suspended according to program rules, but SSA has not yet revised the beneficiary's records to change his or her eligibility status. Thus, overpayments accrue during all months in which the beneficiary engages in SGA and should have benefits suspended, but instead receives a benefit payment.
- The termination phase may follow the EPE. Beginning with the 37th month after the TWP, DI benefits will terminate if the beneficiary engages in SGA; otherwise, the EPE continues. Benefit eligibility terminates in the first month of SGA (or the first such month after the beneficiary uses any grace-period months that may remain). Overpayments can accrue from the month benefit eligibility terminates through the month in which SSA takes corrective administrative action to discontinue the benefit payments. For example, consider a beneficiary who has used all 3 grace-period months in his or her EPE and engages in SGA in the 37th month after the TWP. That beneficiary's eligibility terminates in that month, but SSA may not be aware of that change of status, and the agency may continue to issue monthly benefits. If SSA does not terminate benefit payments until the 57th month after the TWP, all benefits paid during that 20-month period will be counted as overpayments, even if the beneficiary was not working in months 38 through 57 (because eligibility terminated in month 37).
- The initial reinstatement period (IRP) may follow a period of benefit termination for individuals who do not sustain SGA. After benefit termination, a beneficiary may request expedited reinstatement of benefits beginning with the first month in which she or he is no longer engaging in SGA. This request triggers a medical continuing disability review (CDR). During this review, the beneficiary enters the IRP and SSA pays provisional benefits for up to 6 months. If SSA determines that the beneficiary is medically disabled, the IRP continues for at least 24 months from the month of the expedited reinstatement request. As with the EPE, benefit eligibility may be suspended in any month in which the individual engages in SGA, and overpayments can occur. The IRP lasts until the beneficiary receives 24 monthly benefit payments, not counting monthly payments that are suspended for SGA or certain other reasons. After the IRP, the beneficiary is entitled to another TWP and the cycle can begin again.
This description of SSA's work rules does not fully capture their regulatory complexity and the administrative challenge of enforcing them. GAO (2015) posits that the complexity of the SSA work rules contributes to overpayments. Indeed, in qualitative interviews, beneficiaries reported that SSA's earnings-reporting rules were confusing and that they did not have sufficient information (O'Day and others 2016).
To summarize, beneficiaries who work and who complete the TWP and grace-period months are at risk of a work-related overpayment.2 Overpayments may occur during the EPE, the termination phase, or the IRP. During those periods, if beneficiaries engage in SGA, SSA should either suspend benefits (if during the first 36 months of the EPE or in the IRP) or terminate them (after the first 36 EPE months), bringing about a benefit-payment status referred to as suspension or termination because of work (STW). However, for reasons we will detail, SSA does not always timely suspend or terminate benefits, and the lapse results in an overpayment.
Only beneficiaries who meet the criteria for STW status can have a work-related overpayment. As described in more detail below, our analysis identifies beneficiaries at risk of an overpayment as those meeting two criteria: (1) they meet the conditions to have their benefits suspended or terminated for work, and (2) SSA, either concurrently or subsequently (through the date we extracted the analysis data), designated them as in STW status. As researchers, we can only identify beneficiaries who meet the first criterion if SSA has also done so by designating them as in STW status. Hence, it is possible that there are other beneficiaries who were at risk of and potentially accruing overpayments, but were not yet known to SSA or to us as researchers. For brevity, we refer to all beneficiaries who meet both criteria as those who were “in STW status.”
SSA depends on beneficiaries' timely reporting of changes in work activity to avoid overpayments. However, based on data in SSA (2011b), we calculate that in 2010, between 66 percent and 75 percent of beneficiaries with earnings did not comply with earnings-reporting requirements. Similarly, OIG case reviews for 2012 suggest that 65 percent of work-related overpayment dollars were attributed to beneficiary failure to report earnings (SSA 2018). However, a majority (58 percent) of employed beneficiaries who responded to the National Beneficiary Survey indicated that they reported earnings to SSA within 3 months of starting a job (Wright and others 2012). Together, these statistics suggest that some beneficiaries attempt to report earnings but do not follow the correct reporting procedures or that some SSA staff do not correctly process earnings reported by beneficiaries.
When it does not receive a timely earnings report from a beneficiary, SSA must wait to receive earnings information from an administrative data source. During the period we analyze, SSA detected unreported earnings solely from Internal Revenue Service (IRS) data that became available with a lag of as long as 24 months after the earnings occurred (SSA 2011b). The delay reflects the nature of earnings reporting to the IRS. Employers are generally required to submit annual earnings information to the IRS on Form W-2 by January 31st of the year following the calendar year in which the earnings accrued. In turn, employees and the self-employed report their earnings to the IRS when they file their income tax returns, for which the standard deadline is mid-April after the calendar year in which the earnings accrued—although workers may request a 6-month extension to mid-October. After these lags, which vary depending on the earner's situation, SSA receives the IRS data. Agency staff match the IRS records to the SSA account to discern any discrepancies with earnings information reported to SSA by a beneficiary or third party, or lack thereof (Olsen and Hudson 2009). Overpayments may occur and accrue during these periods for any beneficiary with work earnings who has exhausted his or her TWP and grace-period months.
When SSA is apprised of overpayments, whether from beneficiary self-reported earnings or IRS records, agency staff must confirm alleged work incentives, verify wages, and gather other evidence from employers or other knowledgeable third parties before issuing a finding. This process is called a work CDR (in contrast with the medical CDR mentioned earlier). Because of agency backlogs, a work CDR can take several months to complete, adding to potential overpayment accruals. GAO (2011) documented an average delay of about 7 months for SSA to initiate a work CDR across a sample of 60 cases with overpayments. The delays and subsequent overpayments occurred both for beneficiaries who reported their earnings to SSA and those who did not.
Data and Methods
In this section, we describe the data sources and sample selection criteria we use in this analysis. We then describe our approach to identifying work-related overpayments and calculating the associated dollar amounts. Finally, we describe our approach to using this information to produce descriptive statistics on overpayments, adjusting for censoring and truncation.
Data
This analysis uses administrative data from SSA to develop descriptive statistics on the prevalence, size, and duration of work-related overpayments as well as the characteristics of beneficiaries who are overpaid as a result of work. We use data from Disabled Beneficiaries and Dependents (DBAD) files, which are monthly extracts of the Master Beneficiary Record (MBR), the primary repository of data used in administering the DI program. When SSA is apprised of beneficiary work activity, agency staff update the MBR to reflect the revised status. Each MBR update supersedes all previous iterations, and historical records are not retained. The DBAD files, however, capture historical information by preserving monthly snapshots of the MBR. A monthly DBAD snapshot includes the most recent MBR update—which may apply to multiple months—as well as up to 34 previous MBR updates. Note that, for some beneficiaries, the DBAD covers the history of all MBR updates and hence includes the entirety of those beneficiaries' tenures on DI.
For this analysis, we used four different DBAD files to provide data on a 3-year observation period (January 2010–December 2012). We selected the study sample from the January 2010, December 2012, and December 2014 DBAD files. The January 2010 file provided the majority of the statistics we present on beneficiary characteristics. To conduct the analysis of overpayment prevalence, amount, and duration, we used the March 2016 DBAD file, the most recent available at the time we began the analysis. The March 2016 file covered the entire tenures (from January 2010) for all but five beneficiaries, whom we dropped from the analysis.
Because the DBAD files do not contain comprehensive beneficiary information, we used the Disability Analysis File (DAF) for supplemental information. The DAF is SSA's largest longitudinal database of DI beneficiaries. It combines data from a variety of administrative data sources, including the MBR. The DAF is recreated every year with updated data. This analysis used the 2014 version of the DAF.
Analysis Sample
We selected a 10 percent random sample of beneficiaries with records in the January 2010 DBAD file who met certain criteria chosen to represent all eligible or potentially eligible beneficiaries not in terminated-benefit status as of that date. The first criterion was benefit payment status as of January 2010. We included beneficiaries in current-payment status, with payments deferred because of workers' compensation, and with benefits temporarily suspended for one of 10 reasons.3 Beneficiaries in current-payment status in January 2010 accounted for nearly all (98 percent) of the sample.
The second criterion was entitlement to DI disabled-worker benefits on the basis of one's own earnings history (primary beneficiary status). We excluded auxiliary beneficiaries (those who are entitled on the basis of a spouse's, parent's, or decedent's earnings record), as well as beneficiaries who are dually entitled on the basis of both their own and spousal or parental earnings. Overpayment rates for auxiliary and dually entitled beneficiaries may differ from those of the disabled-worker beneficiaries in our sample. We excluded auxiliary beneficiaries because it is difficult to distinguish between overpayments accrued as a result of the primary beneficiary's earnings and those stemming from earnings of the auxiliary or dually entitled beneficiary in the DBAD files. We selected records in which the beneficiary is entitled to benefits only on his or her own earnings record in the January 2010 and December 2012 DBAD files.
Third, we included only beneficiaries who were younger than 62 in the last month of the study period (December 2012) and were not assigned to one of two benefit-offset demonstrations. We implemented the age criterion to exclude from the sample any DI beneficiaries who might have converted to Social Security retirement benefits during the study period. We excluded beneficiaries identified in the December 2014 DBAD file as assigned to either the BOND or the four-state Benefit Offset Pilot Demonstration (BOPD) because the effect of earnings on benefits for BOND and BOPD treatment-group beneficiaries differs from that of current-law beneficiaries and the size and duration of their overpayments will similarly differ. Finally, we excluded 30 beneficiaries whose records were missing in the March 2016 DBAD file.
Our final analysis sample includes 490,193 observations representing all disabled-worker beneficiaries not assigned to BOPD or BOND who were aged 59 or younger and in current-payment or designated suspended-benefit status in January 2010.4 As this is a 10 percent sample, we would expect there to be nearly 5 million such beneficiaries in the DI program at that time. In 2010, there were 5.8 million disabled-worker DI beneficiaries who were younger than 60 (SSA 2011b). Because we exclude dually entitled and auxiliary beneficiaries, beneficiaries assigned to BOPD and BOND, and beneficiaries in certain payment statuses, our sample size appears to be in line with the published SSA estimates of the relevant DI population.
Identifying Overpayments
For this analysis, we focus on overpayments occurring when beneficiaries engage in SGA during the EPE or meet the criteria for work-related benefit termination after the EPE (see Chart 1). We do not examine overpayments that occur during the IRP because the events that trigger them (and the extent of beneficiaries' awareness of their accrual) likely differ from those of overpayments that occur in the EPE or termination phase. Furthermore, only a very small proportion of our sample (0.1 percent) engaged in SGA during the IRP in 2010 and were thus at risk of work-related overpayments. We also do not examine work-related Supplemental Security Income (SSI) overpayments, which could occur for individuals concurrently receiving DI and SSI benefits.
We identify overpayments with a method developed for the BOND evaluation. Because the DBAD files enable us to compare historical and updated beneficiary records for our 2010–2012 study period, we can use this method to identify beneficiaries at risk of overpayment because of their work activity, determine whether a given beneficiary was overpaid, and calculate the overpayment amount. We summarize the method and the efforts to validate our approach below; more detailed information is available in Hoffman and others (2017).
First, we use the March 2016 DBAD to identify beneficiaries who SSA had designated as in STW status (and hence were known to be at risk of overpayment) during 2010–2012.5 Recall that beneficiaries who do not meet the STW criteria are not at risk of overpayment because they are either not engaging in SGA or are using TWP or grace-period months. The March 2016 DBAD, the most recent monthly DBAD file available at the time we conducted this analysis, provides updated SSA information with which to identify STW status.
To identify work-related overpayments, we isolate the historical data on benefits paid in 2010, 2011, and 2012 for beneficiaries whose benefit status had been updated to STW as of the March 2016 DBAD. Specifically, we identify beneficiaries as overpaid when the updated data for a given month retroactively indicate that the beneficiary was in STW status but the historical data, reflecting SSA's awareness at the time, indicate that the beneficiary was in current-payment status. The dollar amount of the overpayment thus identified equals the amount of the benefit due in that month because a beneficiary in STW status is due no benefit.
We validated this approach as part of the BOND evaluation. An SSA official reviewed 10 randomly selected cases for which our algorithm indicated no overpayment and 20 cases in which we identified overpayments. For the 10 instances in which our algorithm identified no overpayment, the SSA review agreed in 9 cases and identified only a $2 overpayment in the other case. This small discrepancy falls within the agency's $30 administrative tolerance and would not warrant recording the overpayment on the beneficiary's record or notifying the beneficiary. In all 20 cases for which the algorithm identified overpayments, the SSA case reviews agreed. Our algorithm's estimate was within 5 percent of the SSA calculation of the overpayment amount for 16 of 20 cases and within 10 percent for 3 of the other 4 cases. In the final case, our algorithm predicted an overpayment of $1,386 versus the SSA calculated overpayment of $1,865. The difference resulted from a retroactive SSA recomputation of the beneficiary's monthly benefit amount that the algorithm did not capture. In aggregate, the predictions from our algorithm for all 20 cases were within 0.3 percent of the corresponding SSA estimate.
Analytical Approach
We begin our analysis by estimating the prevalence, duration, and dollar amount of work-related overpayments. We first estimate overpayments that accrued during 2010. The results provide context on beneficiary-level experiences that correspond with statistics on aggregate overpayments, which are often reported as annual measures, for example in SSA (2013a). Next, we extend the horizon to a 3-year span and produce the same statistics for overpayments that accrued in any month from January 2010 through December 2012. We use the Consumer Price Index for All Urban Consumers to adjust 2011 and 2012 dollars to 2010 values. We expect that the prevalence, duration, and amount of overpayments will all be greater over the longer horizon.
For the 3-year window in which we identify overpayments, overpayment months need not be consecutive. These 3-year statistics are lower-bound estimates of the prevalence, duration, and amount of overpayments beneficiaries may encounter during their DI tenure. For example, some beneficiaries may have accrued overpayments before 2010 or may begin to accrue overpayments in a later year which will not be reflected in the prevalence reported in this article. As described below, we adjust estimated overpayment durations and amounts to account for censoring and truncation.
We analyze overpayments in 2010 because in that year, SSA initiated changes to better identify overpayments. In January 2010, SSA convened a national workgroup that evaluated work CDR processes (SSA 2011a). SSA implemented many of the group's recommendations, including allocating more resources to complete work CDRs and prioritizing the work CDRs with the highest likelihood of overpayments (SSA 2014). Hence, we might expect pre-2009 overpayment statistics to differ from those for 2010 and later.
We do not extend the analysis period beyond 2012 because the necessary lag in SSA identification of overpayments cuts into the potential follow-up period. The more time has elapsed between the study period and the follow-up period, the more comprehensive the statistics on overpayments. The March 2016 DBAD allows for an identification lag of at least 3 years and 3 months (the period from our last month observed, December 2012, to March 2016). Extending the study period by 1 year would decrease the identification period by a year, to a minimum of 2 years and 3 months. In the previous application of this overpayment methodology, Hoffman and others (2017) showed that reducing the lag period from 2 years and 10 months to 1 year and 4 months (that is, removing 18 months of data) decreased the measured prevalence of overpayments by 7 percent, and reducing the lag period from 3 years and 10 months to 2 years and 4 months (similarly, removing 18 months of data) decreased the measured prevalence of overpayments by 4 percent. Accordingly, we are more confident in the estimates produced by using a longer identification period.
We estimate the distribution of the total number of months overpaid based on observed overpayments occurring from January 2010 through December 2012. As noted earlier, these estimates represent the minimum number of overpayment months beneficiaries encounter during their DI tenure. We refine these estimates using survival analysis techniques, which are needed when only partial information is known for some beneficiaries (because we cannot observe overpayments occurring before or after our study period). We use survival techniques to adjust our estimates of months overpaid and total overpayments for two factors: (1) left-truncation, reflecting the potential bias for beneficiaries whose overpayments began before January 2010, because those with longer pre-2010 overpayment periods are more likely to be observed with an overpayment in the 2010–2012 window; and (2) right-censoring, to include the partial information known for beneficiaries whose overpayment extended into 2013 (that is, we know that their months overpaid may exceed a certain value, but not by how much). We flag overpayments observed in January 2010 that are in a spell of consecutive STW months as truncated. We flag observed overpayments in December 2012 as censored; we do not observe overpayment or STW months in or after 2013. Survival analysis is used in estimating the duration and amount of overpayments only and does not change the prevalence of overpayment or the composition of overpaid beneficiaries. Appendix A presents details on our survival analysis methods.
We produce descriptive statistics for beneficiaries with at least one work-related overpayment and, separately, for beneficiaries in STW status who were not overpaid in 2010–2012, and compare their characteristics. We use information in the January 2010 DBAD on beneficiary age, sex, primary impairment, use of a representative payee, duration of current entitlement, first month in STW status during the current entitlement, monthly benefit amount, and geographic region. We use the 2014 DAF for supplementary information on several measures that are not provided or are not as detailed in the January 2010 DBAD, including race, education, concurrent receipt of SSI payments, level of DI claim adjudication, and medical improvement expectation.6 DAF records are available for 490,127 of the 490,193 total observations, resulting in a 99.99 percent match rate. In both data sources, all characteristics reflect the most recent information known as of January 2010.
Finally, we conduct a multivariate analysis to estimate the relationship between beneficiary characteristics and the likelihood of overpayment. We use a logistic regression model in which the independent variable is a binary indicator of a work-related overpayment in 2010, 2011, or 2012. The analysis sample is all beneficiaries in STW status during the study period. We control for a variety of beneficiary characteristics including age group, sex, race, primary impairment, duration of current entitlement to DI, first instance of STW status in current entitlement, use of a representative payee, monthly benefit amount, level of claim adjudication, medical improvement expectation, concurrent receipt of SSI payments, and geographic region. We present marginal effects—estimates of the average effect of changing from the variable's reference category to the indicated category—for ease of interpretation.
Results
In this section, we present descriptive statistics on overpayment prevalence, duration, and dollar amounts. We then examine the demographic and programmatic characteristics of beneficiaries who receive overpayments, including multivariate analysis of the associations between overpayment and certain characteristics.
Statistics on Overpayments
In 2010, 1.2 percent of DI beneficiaries in our sample accrued a work-related overpayment (Table 1).7 However, only 1.8 percent of beneficiaries in our sample were in STW status and hence at risk for a work-related overpayment in 2010 (not shown). Of those engaged in SGA after the end of their grace periods in 2010, 65.2 percent were overpaid.8
| Measure | 2010 | 2010–2012 |
|---|---|---|
| Prevalence (%) among— | ||
| All DI beneficiaries | 1.2 | 1.9 |
| DI beneficiaries in STW status | 65.2 | 71.0 |
| Duration | ||
| Months of overpayment among beneficiaries with any overpayments | 6.5 | 9.4 |
| Overpayment months as a percentage of STW months | 58.7 | 56.7 |
| Overpayment amount ($) among— | ||
| All beneficiaries (mean) | 82 | 192 |
| Beneficiaries with an overpayment | ||
| Mean | 6,976 | 9,941 |
| Median | 5,897 | 7,219 |
| SOURCE: Authors' calculations based on March 2016 DBAD. | ||
| NOTES: A work-related overpayment is a benefit payment occurring in a month for which administrative records later establish that the beneficiary met the conditions for STW status but was not yet designated as such by SSA.
Sample size = 490,193.
|
||
Among beneficiaries who received a work-related overpayment in any month in 2010, the average beneficiary was overpaid in 6.5 months (which were not necessarily consecutive). That average time span represents 58.7 percent of months in 2010 during which beneficiaries were in STW status and thus were at risk of a work-related overpayment as described above.
Reflecting the low prevalence of overpayments among all beneficiaries, the mean work-related overpayment amount for the entire sample was $82. However, the mean amount among those with any overpayments was nearly $7,000. The median overpayment among affected beneficiaries was less than $6,000, and the gap between the mean and median amounts indicates that some beneficiaries received substantial overpayments. Indeed, the 95th percentile overpayment amount in 2010 was $16,914 (not shown).
When we analyze the 3-year window of observations, we find that the prevalence, duration, and amount of overpayments are all higher than those observed in the 1-year frame. The prevalence of work-related overpayments accrued among all beneficiaries during calendar years 2010, 2011, and 2012 was 1.9 percent, exceeding the 2010 rate of 1.2 percent. The prevalence among beneficiaries in STW status during 2010–2012 (71 percent) likewise exceeded the prevalence in 2010 (65 percent). Of course, for any fixed group of beneficiaries, the prevalence over a 3-year period will always at least match the prevalence over a single year within that period.
Beneficiaries who received an overpayment at any point in 2010–2012 were overpaid in 9.4 months on average. Despite a tripling of the study period from 1 year to 3 years, the average duration of overpayment in 2010–2012 is only about 50 percent longer than that for 2010, primarily because right-censoring of spells is less common in the 3-year window than in the 1-year window. By contrast, the percentage of STW months with overpayments was 59 percent in 2010 alone but only 57 percent in 2010–2012. Because this is a cohort analysis, that difference may indicate the effect of an increasing share of individuals in terminated-benefit status over time. Overpayments presumably become less likely the longer benefits have been terminated.
The average overpayment amount among all beneficiaries was $192 and among beneficiaries with any overpayments it was $9,941 for the period 2010–2012. The latter amount is 43 percent greater than the single-year accrual ($6,976). Because the total overpayment amount is the product of the duration of the overpayment period and the monthly benefit amount, which is relatively constant from year to year, we would expect the difference between 1-year and 3-year overpayment amounts to be roughly proportional to the change in the average duration of overpayment. Indeed, the 3-year average duration of overpayment exceeded the 1-year duration for those overpaid by 45 percent.
The differences between the 1-year and the 3-year observations of the prevalence, duration, and size of overpayments highlight the potential effects of truncation and censoring on our statistics. Thirty-four percent of beneficiaries with any overpayments during 2010–2012 were overpaid in January 2010 and an additional 17 percent were overpaid in December 2012. We infer that some beneficiaries in the former group had overpayment spells that began before 2010, given that 86 percent of beneficiaries overpaid in January 2011 and 83 percent of those overpaid in January 2012 were also overpaid in the preceding month. Thus, a significant portion of beneficiaries who were overpaid in January 2010—presumably, more than 80 percent of them—likely were also overpaid before the start of our analysis period. Similarly, we expect that some of those who were overpaid in December 2012 continued to be overpaid beyond 2012.
We adjust the 3-year estimates to account for left-truncation and right-censoring and estimate the total duration of overpayments that occurred in 2010, 2011, or 2012. As described in Appendix A, these adjustments are based, in part, on a proxy for the pre-2010 overpayment months. This proxy is derived from the experiences of approximately 6,000 overpaid beneficiaries in our sample who were first in STW status in 2010, 2011, or 2012. During those 3 years, the ratio of overpayment months to STW months was 65 percent for those beneficiaries. We multiply this estimate by the number of consecutive pre-2010 STW months for each beneficiary with a first STW month before 2010 (1.7 months); the average of this product is 1.1 months.9 We use the proxy for number of pre-2010 overpayment variables as the “entry time variable” in our truncation adjustment. We account for right-censoring by flagging overpayments in December 2012 as censored observations.
The adjusted estimates of the total duration of overpayments accounting for censoring and truncation differ slightly from the unadjusted estimates (Table 2). Among overpaid beneficiaries, we observe a median of 7 months with overpayments in 2010–2012. The adjusted estimate indicates that, if we observed the entirety of the affected beneficiaries' overpayment spells, some of those spells would continue, resulting in a median overpayment duration of 9 months. Estimated overpayment spell durations at the 25th, 75th, and 95th percentiles also increase when accounting for truncation and censoring, from 3 to 4 months, from 14 to 16 months, and from 24 to 30 months, respectively.
| Percentile | Overpayment months | Aggregate overpayment amounts ($) | ||
|---|---|---|---|---|
| Unadjusted | Adjusted | Unadjusted | Adjusted | |
| 5th | 1 | 1 | 928 | 928 |
| 25th | 3 | 4 | 3,166 | 4,221 |
| 50th (median) | 7 | 9 | 7,219 | 9,282 |
| 75th | 14 | 16 | 13,826 | 15,801 |
| 95th | 24 | 30 | 28,441 | 35,551 |
| SOURCE: Authors' calculations based on March 2016 DBAD. | ||||
| NOTES: Unadjusted figures reflect observed months. Adjusted figures account for left-truncated and right-censored records.
Sample is restricted to beneficiaries with any overpayments during 2010–2012.
Sample size = 9,444.
|
||||
Table 2 also shows adjusted and unadjusted overpayment amounts among beneficiaries who received them. The estimated overpayment amounts that account for truncation and censoring are between about $1,000 and $2,000 higher than the unadjusted estimates at each quartile. The median observed overpayment amount is $7,219 and the median amount accounting for truncation and censoring is $9,282. The estimated overpayment amount at the 5th percentile is $928 before and after adjustment, while at the 95th percentile the observed overpayment amount is $28,441 and the adjusted amount is $35,551.
Characteristics of Overpaid Beneficiaries
The results of a bivariate analysis show that beneficiaries in STW status who were overpaid in at least 1 month during 2010–2012 were statistically different from those in STW status and not overpaid, and these outcomes emerged for nearly every characteristic we analyzed (Table 3). Beneficiaries with overpayments differed from those in STW status but not overpaid in their distributions by sex, age, race, and education, as well as by primary impairment. Beneficiaries in STW status with and without overpayments also differed by programmatic factors including SSI receipt, use of a representative payee, monthly DI benefit amount, time elapsed since first STW month, level of benefit adjudication, medical improvement outlook, and SSA region.
| Characteristic | Overpaid | Not overpaid | Difference (percentage points) | p-value of difference | Percentage in subgroup who were overpaid |
|---|---|---|---|---|---|
| Sex | |||||
| Men | 49.7 | 53.5 | -3.8 | < 0.0001 | 69.5 |
| Women | 50.3 | 46.5 | 3.8 | < 0.0001 | 72.6 |
| Age | |||||
| 39 or younger | 38.4 | 33.5 | 4.9 | < 0.0001 | 73.8 |
| 40–49 | 35.8 | 33.6 | 2.2 | < 0.0001 | 72.3 |
| 50–54 | 15.6 | 18.3 | -2.7 | < 0.0001 | 67.7 |
| 55 or older | 10.2 | 14.6 | -4.4 | < 0.0001 | 63.1 |
| Race/ethnicity | |||||
| Asian | 1.8 | 2.6 | -0.8 | < 0.0001 | 62.7 |
| Black (non-Hispanic) | 31.7 | 14.4 | 17.3 | < 0.0001 | 84.4 |
| Hispanic (any race) | 8.8 | 6.7 | 2.1 | < 0.0001 | 76.4 |
| White (non-Hispanic) | 54.6 | 72.7 | -18.1 | < 0.0001 | 64.8 |
| North American Indian/other | 1.7 | 1.8 | -0.1 | < 0.0001 | 69.0 |
| Unknown/missing | 1.4 | 1.8 | -0.4 | < 0.0001 | 65.9 |
| Educational attainment | |||||
| Less than high school | 10.4 | 7.0 | 3.4 | < 0.0001 | 78.5 |
| High school diploma or equivalent | 27.7 | 27.4 | 0.3 | < 0.0001 | 71.2 |
| Some postsecondary school | 15.3 | 17.2 | -1.9 | < 0.0001 | 68.6 |
| College or above | 8.9 | 16.0 | -7.1 | < 0.0001 | 57.7 |
| Missing | 37.7 | 32.4 | 5.3 | < 0.0001 | 74.1 |
| Primary impairment | |||||
| Neoplasms | 5.2 | 11.6 | -6.4 | < 0.0001 | 52.5 |
| Mental disorders | 30.6 | 27.9 | 2.7 | < 0.0001 | 72.8 |
| Intellectual disability | 10.1 | 6.5 | 3.6 | < 0.0001 | 79.2 |
| Injuries | 5 1 | 7.6 | -2.5 | < 0.0001 | 62.2 |
| Back or other musculoskeletal disorders | 18.2 | 17.2 | 1.0 | < 0.0001 | 72.2 |
| Nervous system disorders | 5.0 | 6.2 | -1.2 | < 0.0001 | 66.5 |
| Circulatory system disorders | 4.3 | 4.1 | 0.2 | < 0.0001 | 71.9 |
| Respiratory system disorders | 1.4 | 1.4 | 0.0 | < 0.0001 | 71.8 |
| Severe visual impairments | 1.8 | 1.4 | 0.4 | < 0.0001 | 75.7 |
| Digestive system disorders | 1.6 | 2.7 | -1.1 | < 0.0001 | 58.7 |
| Other impairments | 16.8 | 13.5 | 3.3 | < 0.0001 | 75.3 |
| Benefit type | |||||
| DI only | 88.1 | 91.0 | -2.9 | < 0.0001 | 70.4 |
| Concurrent DI and SSI | 11.9 | 9.0 | 2.9 | < 0.0001 | 76.4 |
| Months as DI beneficiary | |||||
| 36 or fewer | 24.7 | 23.6 | 1.1 | < 0.0001 | 71.9 |
| 37–84 | 36.7 | 40.9 | -4.2 | < 0.0001 | 68.8 |
| 85 or more | 38.6 | 35.5 | 3.1 | < 0.0001 | 72.7 |
| Use of representative payee | |||||
| Yes | 9.4 | 7.3 | 2.1 | 0.0002 | 75.8 |
| No | 90.7 | 92.7 | -2.0 | 0.0002 | 70.6 |
| Monthly DI benefit amount ($) | |||||
| Less than 1,000 | 57.5 | 36.0 | 21.5 | < 0.0001 | 79.6 |
| 1,000–2,000 | 40.1 | 55.9 | -15.8 | < 0.0001 | 63.8 |
| More than 2,000 | 2.4 | 8.2 | -5.8 | < 0.0001 | 41.3 |
| First STW month | |||||
| Before 2010 | 49.0 | 67.9 | -18.9 | < 0.0001 | 63.9 |
| In 2010 | 19.1 | 11.0 | 8.1 | < 0.0001 | 81.1 |
| In 2011 | 16.4 | 11.4 | 5.0 | < 0.0001 | 77.9 |
| In 2012 | 15.5 | 9.8 | 5.7 | < 0.0001 | 79.5 |
| Level of adjudication | |||||
| Initial decision | 81.1 | 83.5 | -2.4 | 0.0171 | 70.5 |
| Reconsideration a | 15.3 | 13.5 | 1.8 | 0.0171 | 73.6 |
| Administrative law judge | 0.4 | 0.3 | 0.1 | 0.0171 | 75.9 |
| Other/unknown | 3.2 | 2.7 | 0.5 | 0.0171 | 74.0 |
| Medical improvement outlook | |||||
| Expected | 6.9 | 11.2 | -4.3 | < 0.0001 | 60.2 |
| Possible | 54.9 | 54.6 | 0.3 | < 0.0001 | 71.2 |
| Not expected | 23.2 | 20.9 | 2.3 | < 0.0001 | 73.1 |
| No information/missing | 15.1 | 13.3 | 1.8 | < 0.0001 | 73.6 |
| SSA region | |||||
| Atlanta | 18.2 | 12.8 | 5.4 | < 0.0001 | 77.8 |
| Boston | 6.3 | 8.7 | -2.4 | < 0.0001 | 64.0 |
| Chicago | 14.5 | 14.3 | 0.2 | < 0.0001 | 71.3 |
| Dallas | 15.5 | 12.7 | 2.8 | < 0.0001 | 75.0 |
| Denver | 2.9 | 3.5 | -0.6 | < 0.0001 | 67.1 |
| Kansas City | 4.6 | 5.1 | -0.5 | < 0.0001 | 68.7 |
| New York | 9.6 | 12.0 | -2.4 | < 0.0001 | 66.1 |
| Philadelphia | 11.5 | 12.0 | -0.5 | < 0.0001 | 70.1 |
| San Francisco | 13.6 | 14.6 | -1.0 | < 0.0001 | 69.5 |
| Seattle | 3.4 | 4.4 | -1.0 | < 0.0001 | 65.6 |
| Sample size | 9,444 | 3,853 | 5,591 | . . . | 71.0 |
| SOURCE: Authors' calculations based on January 2010 DBAD, March 2016 DBAD, and 2014 DAF. | |||||
| NOTES: Rounded components of percentage distributions do not necessarily sum to 100.0.
. . . = not applicable.
|
|||||
| a. Includes reconsideration hearing. | |||||
Table 3 also shows how the prevalence of overpayment differs across subgroups. Overpayment rates were highest for beneficiaries who were black, had less than a high school education, had a primary impairment of intellectual disability, or had monthly benefits of less than $1,000. More than 78 percent of beneficiaries in each of those subgroups were overpaid, compared with 71 percent of the entire sample. By contrast, less than 58 percent of beneficiaries in STW status who had a college degree, a primary impairment of neoplasm, or monthly DI benefits of more than $2,000 had overpayments.
The prevalence of overpayment was greater among beneficiaries whose first STW month occurred in 2010, 2011, or 2012 (about 80 percent for each group) than for those whose first STW month was before 2010 (64 percent). Some beneficiaries who were first at risk of overpayment before 2010 presumably accrued overpayments before 2010. SSA would have suspended benefit payments when overpayments were detected—perhaps making that subgroup less likely to have overpayments during 2010–2012 than were beneficiaries newly exposed to overpayment risk.
We expect covariation across beneficiary characteristics (such as education and monthly DI benefit amount) as well as covariation between beneficiary characteristics and variables related to program participation such as the first STW month. Bivariate analysis does not account for these relationships and, accordingly, we conducted a multivariate analysis to isolate the association between each particular characteristic and the likelihood of an overpayment, holding all other characteristics constant.
In the multivariate analysis, several of the demographic characteristics are statistically significant predictors of overpayment among beneficiaries in STW status during 2010–2012 (Table 4). Among those at risk, black and Hispanic beneficiaries were more likely to be overpaid than their white counterparts, by 17 percentage points and 7 percentage points, respectively. In addition, beneficiaries aged 54 or younger were more likely to be overpaid than were those aged 55 or older, holding other characteristics constant. Age may predict overpayments in part because work CDRs are processed by distinct SSA entities depending on beneficiary age. The centralized Office of Disability Operations in Baltimore, Maryland processes work CDRs for beneficiaries who are younger than 54 and regional processing centers conduct work CDRs for those aged 54 or older (GAO 2011). If the work CDR processing times differ between those entities, we would expect to see overpayment rates differ around the age cutoff.10
| Characteristic | Marginal effect | p-value |
|---|---|---|
| Sex | ||
| Men | 0.0 | 0.98 |
| Women (reference) | . . . | . . . |
| Age | ||
| 39 or younger | 5.6 | 0.00 |
| 40–49 | 6.1 | 0.00 |
| 50–54 | 3.7 | 0.01 |
| 55 or older (reference) | . . . | . . . |
| Race/ethnicity | ||
| Asian | -0.5 | 0.85 |
| Black (non-Hispanic) | 16.9 | 0.00 |
| Hispanic (any race) | 6.7 | 0.00 |
| White (non-Hispanic) (reference) | . . . | . . . |
| North American Indian/other | 2.1 | 0.45 |
| Unknown/missing | 1.3 | 0.64 |
| Educational attainment | ||
| Less than high school | 3.6 | 0.02 |
| High school diploma or equivalent (reference) | . . . | . . . |
| Some postsecondary school | -1.9 | 0.10 |
| College or above | -5.7 | 0.00 |
| Missing | 2.4 | 0.03 |
| Primary impairment | ||
| Neoplasms | -10.8 | 0.00 |
| Mental disorders (reference) | . . . | . . . |
| Intellectual disability | -1.0 | 0.60 |
| Injuries | -7.0 | 0.00 |
| Back or other musculoskeletal disorders | -1.5 | 0.20 |
| Nervous system disorders | -5.1 | 0.00 |
| Circulatory system disorders | -0.5 | 0.80 |
| Respiratory system disorders | -1.4 | 0.66 |
| Severe visual impairments | 2.3 | 0.46 |
| Digestive system disorders | -9.5 | 0.00 |
| Other impairments | 0.5 | 0.71 |
| Benefit type | ||
| DI only (reference) | . . . | . . . |
| Concurrent DI and SSI | -8.5 | 0.00 |
| Months as DI beneficiary | ||
| 36 or fewer | -0.9 | 0.48 |
| 37–84 | -0.8 | 0.39 |
| 85 or more (reference) | . . . | . . . |
| Use of representative payee | ||
| Yes | -1.2 | 0.43 |
| No (reference) | . . . | . . . |
| Monthly DI benefit amount ($) | ||
| Less than 1,000 (reference) | . . . | . . . |
| 1,000–2,000 | -11.5 | 0.00 |
| More than 2,000 | -23.0 | 0.00 |
| First STW month | ||
| Before 2010 (reference) | . . . | . . . |
| In 2010 | 18.1 | 0.00 |
| In 2011 | 14.0 | 0.00 |
| In 2012 | 14.9 | 0.00 |
| Level of adjudication | ||
| Initial decision (reference) | . . . | . . . |
| Reconsideration a | 1.0 | 0.42 |
| Administrative law judge or other/unknown | 1.7 | 0.45 |
| Medical improvement outlook | ||
| Expected | -6.3 | 0.00 |
| Possible | -2.6 | 0.01 |
| Not expected (reference) | . . . | . . . |
| No information/missing | -1.2 | 0.43 |
| SSA region | ||
| Atlanta (reference) | . . . | . . . |
| Boston | -8.3 | 0.00 |
| Chicago | -5.1 | 0.00 |
| Dallas | -3.1 | 0.03 |
| Denver | -5.3 | 0.02 |
| Kansas City | -4.8 | 0.01 |
| New York | -9.9 | 0.00 |
| Philadelphia | -6.6 | 0.00 |
| San Francisco | -4.1 | 0.00 |
| Seattle | -6.9 | 0.00 |
| SOURCE: Authors' calculations based on January 2010 DBAD, March 2016 DBAD, and 2014 DAF. | ||
| NOTES: Data on race, education, concurrent DI and SSI receipt, level of adjudication, and medical improvement status are from DAF records for 9,442 beneficiaries with overpayments and 3,848 beneficiaries in STW status who are not overpaid. We retain non-DAF observations that do not match DAF records and code the corresponding DAF variables as "missing."
. . . = not applicable.
|
||
| a. Includes reconsideration hearing. | ||
Several health-related factors were also statistically significant predictors of overpayment among those in STW status. Beneficiaries with a primary impairment of neoplasms, injuries, nervous system disorders, and digestive system disorders were less likely to be overpaid than were those in the baseline category of mental disorders (which does not encompass intellectual disability)—all other characteristics being equal. Although we hypothesized that characteristics associated with lower levels of mental functioning would be associated with an increased likelihood of overpayment, intellectual disability has no statistically significant difference from the baseline category of mental disorders in the probability of overpayment. Finally, beneficiaries in STW status for whom medical improvement is expected or possible were also less likely to be overpaid than were those for whom medical improvement was categorized as not expected.
The strong and significant associations between overpayments and both education and DI benefit amount may signal disparities in compliance with SSA rules among beneficiaries in STW status within those categories. Relative to those with a high school–level education, beneficiaries with less than a high school education were 4 percentage points more likely and those with at least a college degree were 6 percentage points less likely to be overpaid. Beneficiaries with a DI benefit amount of more than $2,000 per month were 23 percentage points less likely to be overpaid than were otherwise similar beneficiaries receiving DI benefits of less than $1,000 per month. These findings suggest that beneficiaries with higher levels of education and the skills and training associated with higher-paying occupations (which determine the DI benefit amount) may be more apt to comply with the SSA requirements for reporting earnings. These beneficiaries may be more likely to understand and adhere to SSA's reporting requirements for earnings, or to seek and receive appropriate guidance from SSA field offices, or to have less trepidation about reporting work activity because of a comparatively stable financial situation, among other possible explanations.
Several characteristics may be related to exposure to SSA earnings-reporting requirements, which are presumably predictive of lower likelihood of overpayment. For example, beneficiaries who were in STW status and were concurrently receiving DI and SSI benefits in January 2010 were significantly less likely than those receiving only DI benefits to be overpaid, holding other characteristics constant. (We observed the reverse relationship in the bivariate results presented in Table 3, which highlights the importance of controlling for beneficiary characteristics.) Unlike DI-only beneficiaries, recipients of concurrent benefits must also meet SSI's more stringent monthly earnings-reporting requirements. In addition, with all else being equal, beneficiaries whose STW status began during the analysis period were significantly more likely to be overpaid than were those whose first STW month occurred before 2010. The likely reason is that SSA has had a longer time to become aware of beneficiary earnings, complete a work CDR, and, if warranted, declare STW status and suspend benefits, thereby ending a spell of overpayments.
Finally, certain SSA regions were strong predictors of overpayment. Beneficiaries in the Boston and New York regions were respectively 8 percentage points and 10 percentage points less likely to be overpaid than their counterparts in the Atlanta region. There may be differences in awareness of reporting requirements for earnings or in the rate of SSA processing of work CDRs across geographic regions. Indeed, SSA took action to reduce the duration and size of overpayments in the New York region in 2010. This effort (described in the discussion section) may have reduced the prevalence of overpayments during the study period. That is, if overpayment spells are shorter, there is a lower likelihood that a given overpayment spell occurred within the 2010–2012 window.
Discussion
This analysis is the first to reliably quantify the prevalence of work-related disability benefit overpayments, the per-beneficiary duration and amount of such overpayments, and the estimated likelihood of receiving overpayments by selected beneficiary characteristics. Such statistics have been elusive because the SSA system that tracks overpayments is an operational tool structured to monitor the outstanding balance of overpayments rather than a research tool designed to generate beneficiary-level statistics. Previous analyses have produced approximate measures of overpayments using case reviews with relatively small samples, or created lower-bound estimates using earnings data without information on the use of DI work incentives such as the TWP. In this analysis, we use a 10 percent sample of DI beneficiaries meeting logical inclusion criteria, resulting in a sample size of nearly 500,000 beneficiaries. Our analysis is based on an administrative data algorithm that identifies work-related overpayments in a given month.
We analyze the 3-year period from January 2010 to December 2012. It is important to note that the U.S. economy was beginning to recover from the Great Recession throughout that period. The prevalence and size of overpayments may be affected by economic conditions, including the proportion of beneficiaries who work (and hence are at risk of an overpayment), and also by the resources with which SSA can process work CDRs and adjust benefits timely.
The algorithm we use may not capture all work-related overpayments. For example, because our algorithm is based on benefits due (the amount to which a beneficiary is entitled in a month based on work activity in that month), it will not capture any adjustments such as withholdings to repay previous overpayments or lump-sum transfers to reconcile underpayments. These circumstances could lead to errors in either direction in our estimates of overpayment amounts. Although beneficiary-level estimates may exhibit small differences from the official SSA overpayment calculations, we expect the aggregate statistics to be unbiased estimates. Indeed, SSA case reviews of 20 current-law beneficiaries' records with overpayments found that the algorithm estimated an overpayment amount within 0.3 percent of the SSA calculation (Hoffman and others 2017).
Our results indicate that, during 2010–2012, 1.9 percent of all beneficiaries meeting our selection criteria were overpaid. This estimate is within the range of estimates produced by previous attempts to quantify the prevalence of overpayments over varying study periods, which range from 0.4 percent of beneficiaries in a 15-month period (GAO 2013) to 3.2 percent over a 10-year period (SSA 2015). Among beneficiaries who were in STW status during 2010–2012, we estimate that 71 percent were overpaid. The prevalence of overpayments among those whose first exposure to overpayment risk occurred within the study period is higher—approximately 80 percent. Previous OIG studies estimated that between 63 percent and 92 percent of beneficiaries who engaged in SGA were overpaid (SSA 2014, 2015). As we have noted, the estimates presented here are based on a different and presumably more reliable methodology. Our results definitively establish that, in the analysis period, overpayments were the norm for beneficiaries who engaged in SGA after the TWP and grace period.
When we adjusted our estimates to account for the entirety of the overpayment spells we observed, the median overpayment accruals were 9 months and $9,282. Between the 25th and 75th percentiles, adjusted estimates of accrued overpayments ranged from 4 months and $4,221 to 16 months and $15,801. These estimates are in line with an average 9-month duration and $8,114 overpayment amount identified in an OIG review of 275 cases involving beneficiaries with substantial earnings from 2007 to 2011 (SSA 2014). The overpayment amounts we estimate are lower than the $14,397 average amount identified during a 10-year OIG study that began in 2003, but that estimate was based on a small sample of 32 overpaid beneficiaries (SSA 2015). Additional sources of variation may include differences in methodology or sample composition, changes in the size of overpayments over time, or some combination of factors.
Our findings conform to the presumptive expectations that beneficiaries with little contact with the SSA disability programs are relatively more likely to receive work-related overpayments than are beneficiaries with more familiarity with SSA programs. Notably, beneficiaries who concurrently receive DI and SSI benefits are less likely to be overpaid than their DI-only counterparts, holding other characteristics constant. This suggests that awareness of SSI's strict earnings-reporting requirements in addition to the DI program rules helps recipients of concurrent benefits to avoid overpayment situations. This is particularly notable because recipients of concurrent benefits are more likely to have lower levels of education and lower DI benefit amounts, which are significantly associated with a higher likelihood of overpayment. Hence, the requirements and monitoring in the SSI program may be effective for populations that are otherwise less likely to be in compliance.
We do not have earnings data for overpaid beneficiaries, making it difficult to assess the potential burden of repayment relative to their incomes. For expositional purposes, assume that a beneficiary was overpaid $9,282 over the course of 9 months and earned $1,500 (50 percent above the 2010 SGA amount) in each of those months. The beneficiary received $22,782 in earnings plus benefits over those 9 months, only to learn later that more than 40 percent of that income was owed back to SSA. The burden would be greater still for a beneficiary with earnings just above the SGA level; overpayments would in that case amount to more than half of total income for the period. SSA may allow repayment in installments to disperse the burden over an extended period, but such plans are not always granted. Previous studies have reported beneficiary frustration and other negative reactions to overpayment notifications (Gubits and others 2013; O'Day and others 2016; Hoffman and others 2017).
Although the average estimated overpayment amount among all beneficiaries in our sample is modest—$82 in 2010—it implies an aggregate overpayment amount of $402 million among the 4,901,930 DI beneficiaries who met our sample selection criteria in 2010. SSA (2013a) reports more than twice that amount ($831 million) for 2010. This difference is expected, in large part because SSA calculations are based on all DI beneficiaries—numbering approximately 9.4 million—a population almost twice as large as that represented by our sample. In fact, the SSA statistics imply an average overpayment of about $88 among all DI beneficiaries, similar to the $82 per beneficiary we estimate for our sample. The composition of our sample differs from that of all DI beneficiaries and may contribute to the minor differences in the per-beneficiary overpayment amount. In addition, the SSA figure reflects overpayments detected in 2010, the first year of our 3-year study period, which may include overpayment months in several calendar years (in or before 2010). Our analysis focuses on overpayments incurred in the analysis period and detected thereafter (through December 2016).
SSA has undertaken several initiatives to reduce the frequency and size of overpayments. For example, the agency prioritized work CDRs and allocated staff to process the oldest cases in 2010 and enhanced those efforts in 2011. Also beginning in 2010, SSA piloted a predictive model in the New York region's processing center, which prioritizes work CDRs for beneficiaries most likely to have large overpayments (SSA 2011a). In June 2011, SSA expanded the program to include three processing centers covering 60 percent of cases with unreported earnings (SSA 2014). The pilot yielded a reduction in work-related overpayment amounts, and the agency implemented the practice nationwide in June 2013 (SSA 2013b). Although the efforts appear to be effective in reducing overpayment amounts, they are unlikely to reduce overpayment incidence.
SSA continues to explore ways to reduce both the size and likelihood of overpayments. Until 2016, SSA detected beneficiary earnings predominantly from IRS data. However, those data are not available to SSA until the following calendar year, sometimes 18 to 24 months after the beneficiary earned the wages. In 2017, SSA implemented a nationwide program called Work Smart that entails quarterly earnings checks based on a Department of Health and Human Services' Office of Child Support Enforcement database called the National Directory of New Hires (SSA 2018). In addition, SSA is working to establish exchanges with payroll data providers to get faster access to wage data. These efforts are likely to reduce delays in identifying unreported earnings, which could in turn reduce the likelihood and amount of overpayments.
The complexity of DI rules governing earnings—and limited beneficiary awareness of those rules and requirements—may contribute to work-related overpayments (GAO 2015). Although SSA promotes beneficiary education with agency-funded work-incentive counselors and through other means, the low rate at which beneficiaries report earnings suggests that there is room for improvement.
One potential option for reducing overpayments is to enhance SSA communication with beneficiaries. The availability and clarity of information could be improved and targeted to beneficiaries with characteristics associated with the likelihood of overpayment. Presently, SSA informs beneficiaries about the earnings-reporting requirements during the initial claim process, with written documentation when the claim is initially approved, and in an annual letter announcing the cost-of-living benefit adjustment. The reporting requirements—along with other information—are available online and on request, but beneficiaries may not be aware of these resources. Our analysis found substantial variation in the likelihood of overpayment by race, education, primary impairment, and DI benefit amount, among other factors. The differences we observed in overpayment incidence by education may indicate that beneficiaries with lower education levels are less likely than their better-educated peers to read, understand, or remember the written material they received. Revising the printed materials or conducting outreach by phone may provide more effective communication with this population, and may facilitate understanding among beneficiaries more broadly. Increased beneficiary awareness and understanding of the reporting requirements may translate into increased compliance and thus a lower overpayment incidence.
Another option is to institute more accessible and monitored reporting requirements for DI, similar to those used in the SSI program. As noted earlier, beneficiaries who concurrently receive DI and SSI benefits are less likely to be overpaid than are those who receive DI only. We hypothesize that the SSI reporting requirements and processes are more effective than those for the DI program (or that their combination with the DI requirements instills a broader knowledge of reporting requirements among recipients of concurrent DI-SSI benefits). Several elements of SSI reporting that may be beneficial for the DI program include consistent wage reporting during the first 6 days of the month and e-mail and text reminders to report wages. SSI recipients also have the option of using a smartphone wage-reporting application. In September 2017, SSA implemented an electronic earnings-reporting system for DI beneficiaries, which is expected to improve reporting.
This article presents beneficiary-level statistics on work-related disability benefit overpayments and provides information that may advance efforts to reduce the incidence, duration, and dollar amount of overpayments. However, many questions about overpayments remain unanswered. Further research into the effects of overpayment on the nature of the beneficiary experience, SSA operations, and program finances is necessary to inform reasonable expectations and offer context for our findings. Longitudinal studies might track changes in the size and frequency of overpayments that may result from recent and pending SSA efforts and may point to additional areas for improvement. In addition, the implications of overpayments are unknown. Future research should consider the consequences of work-related overpayments for beneficiary employment and well-being. Without additional research, the prevalence and magnitude of documented negative beneficiary reactions to work-related overpayments cannot be reliably quantified.
Appendix A
We estimate the duration of overpayment spells by deriving the distribution of overpayment time (that is, the survival curve) using the PROC PHREG command in SAS v9.4. The distribution of overpayment time can be used to determine the proportion of a population that will remain overpaid beyond a certain window. To arrive at the distribution, this nonparametric method calculates, for each month in the observation window, the proportion of beneficiaries who exited overpayment status in that month, relative to all beneficiaries with observable overpayment data in that month. The censoring indicator reflects whether or not the beneficiary was observed to have exited overpayment status in December 2012. In this way, the partial information known for right-censored individuals (that is, that they remained overpaid at least through and possibly beyond December 2012) is factored in by including individuals in the calculations for as long as they were observed. In a typical Cox model analysis, only the time to the first event would be analyzed and recurrent events would be ignored. As a simplifying assumption, we consider all episodes to be contiguous. More than three-quarters of overpaid beneficiaries in the analysis sample had just one overpayment spell.
In addition to accounting for right-censoring, we account for the length of unobserved left-truncation time (that is, the time beneficiaries were overpaid prior to 2010) among those who were overpaid in January 2010 and also had a consecutive spell of STW months leading up to January 2010. To do so, we start by counting the total number of consecutive STW months prior to January 2010 (necessarily including STW status in December 2009). We multiply the number of consecutive pre-2010 months by an estimate of the expected proportion of overpayment months.11 This expected proportion is estimated from the sample of beneficiaries whose STW status began in the 2010–2012 window; among this sample, we count the number of STW months before December 2012 and the number of those months for which beneficiaries were overpaid, and divide the latter by the former to obtain the expected proportion of overpayment months. In sensitivity analyses, we tested other proxies for the number of pre-2010 overpayment months, but found that the predicted 5th-, 25th-, 50th-, and 75th-percentile values were unchanged and that there were only small changes at the 95th percentile.
We use the estimated distribution (the survival curve) of adjusted overpayment months described in the previous paragraph (accounting for right-censoring and left-truncation) to estimate the distribution of adjusted overpayment amounts. First, we calculate the unadjusted monthly overpayment amount by dividing the total unadjusted overpayment amount by the unadjusted overpayment length. We then multiply this value by the adjusted number of overpayment months (accounting for truncation and censoring) to arrive at the adjusted overpayment amount.
Notes
1 The threshold for SGA can vary depending on the beneficiary's circumstances. In most cases, SSA determines whether a DI claimant or beneficiary is engaging in SGA based on the beneficiary's wages or self-employment earnings; but the agency also offers a wide variety of work incentives that may reduce a beneficiary's countable earnings to a level that is lower than the SGA threshold and thereby allow continued benefit eligibility.
2 In rare instances, work-related overpayments occur because a new DI beneficiary returns to SGA within 12 months of disability onset.
3 The 10 reasons are (1) conditional payment status, (2) technical entitlement, (3) pending determination of continuing disability, (4) work (outside the United States), (5) work (inside the United States), (6) pending provision of accurate current address, (7) prisoner suspension, (8) SGA suspension during the EPE, (9) refusal of vocational rehabilitation services, and (10) payee not determined.
4 Beneficiaries aged 59 or younger in January 2010 were thus younger than 62 in December 2012.
5 SSA does not directly identify whether a beneficiary in the EPE or a subsequent benefit termination phase meets the STW criteria in its administrative data. Therefore, we must determine a beneficiary's STW status by collecting and assessing various data elements in combination. We use an algorithm developed for the DAF to identify STW status.
6 SSA no longer publishes statistics by race because of inconsistencies in data collection and racial category definitions over time. For more information, see Martin (2016).
7 Although our analysis excludes overpayments occurring during the IRP, their inclusion would not change the overall prevalence (1.2 percent).
8 SSA recognized that the other 34.8 percent met the STW criteria in real time and discontinued their benefit payments before issuing any overpayments.
9 We ran several models to account for left-truncation in addition to the model on which we base the main results. One alternative was to account for pre-2010 overpayment months during any pre-2010 STW months, even if they were not consecutive to January 2010. This alternative specification produced an average of 2.8 consecutive pre-2010 overpayment months and the adjusted estimates it generated are identical to those of our proxy.
10 Note that the age cutoff we use in Table 4 (between 54 and 55) differs by 1 year from SSA's cutoff for assigning work CDRs to the central processing center or a regional one (between 53 and 54).
11 An alternative approach would be to directly calculate the consecutive overpayment months used in the left-truncation adjustment. That approach, however, would exceed the scope and resources of this research.
References
[GAO] Government Accountability Office. 2011. SSA Can Improve Efforts to Detect, Prevent, and Recover Overpayments. GAO Publication No. 11-724. Washington, DC: GAO.
———. 2013. Work Activity Indicates Certain Social Security Disability Insurance Payments Were Potentially Improper. GAO Publication No. 13-635. Washington, DC: GAO.
———. 2015. SSA Could Do More to Prevent Overpayments or Incorrect Waivers to Beneficiaries. GAO Publication No. 16-34. Washington, DC: GAO.
———. 2016. SSA Needs to Better Track Efforts and Evaluate Options to Recover Debt and Deter Potential Fraud. GAO Publication No. 16-331. Washington, DC: GAO.
Gubits, Daniel, Michelle Derr, Jillian Berk, Ann Person, David Stapleton, Denise Hoffman, Stephen Bell, Rachel Cook, and David Wittenburg. 2013. BOND Implementation and Evaluation: Stage 2 Early Assessment Report. Cambridge, MA: Abt Associates.
Hoffman, Denise, Sarah Croake, David R. Mann, David Stapleton, Priyanka Anand, Chris Jones, Judy Geyer, Daniel Gubits, Stephen Bell, Andrew McGuirk, David Wittenburg, Debra Wright, Amang Sukasih, David Judkins, and Michael Sinclair. 2017. BOND Implementation and Evaluation: 2016 Stage 1 Interim Process, Participation, and Impact Report. Cambridge, MA: Abt Associates, and Washington, DC: Mathematica Policy Research. https://www.ssa.gov/disabilityresearch/documents/BOND_Deliverable%2024c%202%201_3%2020%2017_clean_toSSA_with_Warning.pdf.
Kregel, John. 2017. “A Qualitative Study of Employment Experiences of SSDI Beneficiaries After Receipt of an Overpayment.” DRC Working Paper No. 2018-06. Washington, DC: Mathematica Policy Research.
Martin, Patricia. 2016. “Why Researchers Now Rely on Surveys for Race Data on OASDI and SSI Programs: A Comparison of Four Major Surveys.” Research and Statistics Note No. 2016-01. Washington, DC: SSA.
O'Day, Bonnie, Frank Martin, Hannah Burak, Gina Freeman, Kathleen Feeney, Grace Lim, Elizabeth Kelley, and Katie Morrison. 2016. “Employment Experiences of Young Adults and High Earners Who Receive Social Security Disability Benefits: Findings from Semistructured Interviews.” Washington, DC: Mathematica Policy Research.
Olsen, Anya, and Russell Hudson. 2009. “Social Security Administration's Master Earnings File: Background Information.” Social Security Bulletin 69(3): 29–46.
[SSA] Social Security Administration. 2011a. Annual Statistical Report on the Social Security Disability Insurance Program, 2010. Publication No. 13-11826. Washington, DC: SSA.
———. 2011b. The Social Security Administration's Report on Continuing Disability Reviews Resulting from Work Activity. https://www.ssa.gov/legislation/WorkCDRFY2010(edited).pdf.
———. 2013a. Social Security Administration Agency Financial Report, Fiscal Year 2013. Baltimore, MD: SSA. https://www.ssa.gov/finance/fy13_AFR.html.
———. 2013b. Social Security Administration Annual Payment Recapture Audit Report. https://www.ssa.gov/improperpayments/documents/Annual_PRA_Report_2013_10252013.pdf.
———. 2014. Work Continuing Disability Reviews for Disabled Title II Beneficiaries with Earnings. Audit Report No. A-01-12-12142. Baltimore, MD: SSA, Office of the Inspector General. https://oig.ssa.gov/sites/default/files/audit/full/pdf/A-01-12-12142_0.pdf.
———. 2015. Overpayments in the Social Security Administration's Disability Program—A 10-Year Study. Audit Report No. A-01-14-24114. Baltimore, MD: SSA, Office of the Inspector General. https://oig.ssa.gov/sites/default/files/audit/full/pdf/A-01-14-24114.pdf.
———. 2016. Social Security Administration Agency Financial Report, Fiscal Year 2016. Baltimore, MD: SSA. https://www.ssa.gov/finance/fy16_AFR.html.
———. 2018. Incorrect Payments to Disabled Beneficiaries Who Return to Work. Audit Report No. A-07-17-50131. Baltimore, MD: SSA, Office of the Inspector General. https://oig.ssa.gov/sites/default/files/audit/full/pdf/A-07-17-50131.pdf.
Wright, Debra, Gina Livermore, Denise Hoffman, Eric Grau, and Maura Bardos. 2012. “2010 National Beneficiary Survey: Methodology and Descriptive Statistics.” Washington, DC: Mathematica Policy Research.