Trends in the Social Security and Supplemental Security Income Disability Programs
Changes in Program Policy Influencing Program Size
Introduction
Policy changes can have direct effects on program size. Changes in the way that the Social Security Administration makes disability decisions can affect the number of persons entering the disability programs, as was the case with the changes in the criteria for determining disability for mental disorders that were enacted as part of the 1984 Amendments. In the overview section of this book, a brief history of policy changes was presented. In this section, those changes will be discussed with reference to program size, particularly with respect to entry into and exit from the disability programs.
The purpose of this section is to show trends leading up to policy changes and the trends that follow them. It is not possible to measure definitively the contribution each policy change has made to the trends of the disability programs, because numerous other factors play a role in influencing trends. The reader is cautioned that correlation does not imply causality, and one must keep in mind the totality of factors that may have contributed to trends in the disability programs.
Changes in Policy Influencing—
Disability Awards
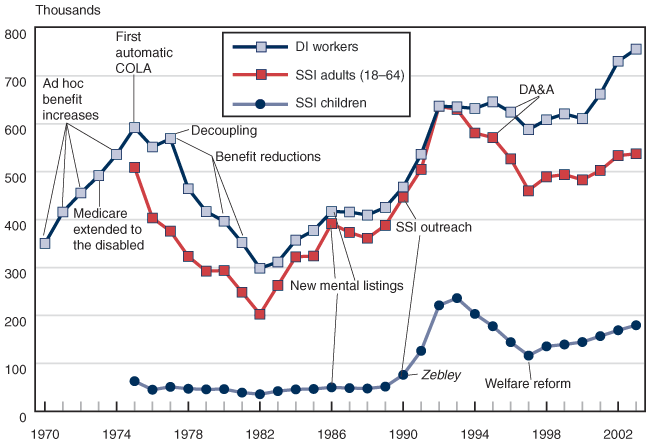
Policy changes appear to play predictable roles in determining awards of disability benefits. Reductions in benefits for the DI program and program changes in the late 1970s and early 1980s appear to have led to fewer applications and fewer awards for the DI and SSI programs.
| Year | DI workers | SSI adults (18–64) | SSI children |
|---|---|---|---|
| 1970 | 350.38 | . . . | . . . |
| 1971 | 415.90 | . . . | . . . |
| 1972 | 455.44 | . . . | . . . |
| 1973 | 491.78 | . . . | . . . |
| 1974 | 535.98 | . . . | . . . |
| 1975 | 592.05 | 508.95 | 62.88 |
| 1976 | 551.46 | 403.35 | 45.03 |
| 1977 | 568.87 | 375.95 | 50.97 |
| 1978 | 464.42 | 323.17 | 47.05 |
| 1979 | 416.71 | 292.38 | 45.81 |
| 1980 | 396.60 | 293.74 | 46.26 |
| 1981 | 351.85 | 248.34 | 39.05 |
| 1982 | 298.53 | 202.59 | 35.67 |
| 1983 | 311.49 | 262.66 | 42.11 |
| 1984 | 357.14 | 322.39 | 45.74 |
| 1985 | 377.37 | 324.07 | 46.59 |
| 1986 | 416.87 | 391.60 | 50.00 |
| 1987 | 415.85 | 373.32 | 48.48 |
| 1988 | 409.49 | 361.07 | 47.56 |
| 1989 | 425.58 | 388.12 | 51.52 |
| 1990 | 467.98 | 446.94 | 76.07 |
| 1991 | 536.43 | 504.86 | 126.19 |
| 1992 | 636.64 | 636.30 | 221.08 |
| 1993 | 635.24 | 630.03 | 236.22 |
| 1994 | 631.87 | 580.64 | 203.19 |
| 1995 | 645.65 | 571.08 | 177.55 |
| 1996 | 624.25 | 526.69 | 144.27 |
| 1997 | 587.70 | 461.26 | 116.28 |
| 1998 | 608.38 | 489.24 | 135.60 |
| 1999 | 620.56 | 493.96 | 139.40 |
| 2000 | 610.70 | 483.02 | 144.54 |
| 2001 | 661.90 | 502.59 | 156.90 |
| 2002 | 730.38 | 533.47 | 169.13 |
| 2003 | 755.71 | 537.42 | 179.59 |
| NOTE: . . . = not applicable. | |||
In the early 1970s, Congress enacted changes that increased the levels of benefits paid under the Social Security disability program. These changes included ad hoc, across-the-board benefit increases of 15 percent in 1970, 10 percent in 1971, 20 percent in 1972, and 11 percent in 1974. Automatic cost-of-living adjustments (COLAs) began with the first COLA in June 1975. Medicare was added to the disability program effective in 1973. The increasing benefits (higher cash benefits and Medicare) probably contributed to the growth of the disability program in the early to mid-1970s.
Growth in the disability rolls during the early to mid-1970s prompted Congress to enact legislation to slow the growth, in part by reducing benefits. The 1977 Amendments "decoupled" the effects of inflation on earnings and the adjustments of the consumer price index (CPI) in the benefit formula to reduce the unintended increase in disability benefits and replacement rates. This decoupling was accomplished by indexing earnings in the benefit formula and applying CPI adjustments to benefits rather than to the benefit formula. As part of the 1980 Amendments, additional benefit reductions were instituted by capping the family benefit amount and reducing the number of dropout years in the benefit calculation. In 1981, Congress eliminated the Social Security minimum benefit (minimum primary insurance amount) and placed a cap on the replacement rate from all public disability program benefits. As can be seen in Chart 49, fairly significant reductions in benefits and replacement rates probably contributed to a decline in awards from 1977 to 1982. The 1980 Amendments also required SSA to conduct more preeffectuation quality reviews for favorable decisions.
The 1984 Amendments, enacted in response to public outcry over disability policy in the early 1980s, mandated that SSA develop new disability standards for individuals with mental disorders, evaluate pain as part of the decision process, place emphasis on evidence from treating physicians in the decision process, and consider the impact of multiple nonsevere impairments in determining disability. The decline in award rates and the decrease in disability beneficiaries in the early 1980s began to reverse itself, and growth accelerated in the late 1980s and early 1990s. Awards for mental disorders continued to increase, both in absolute numbers (Chart 50) and as a percentage of awards (Charts 27, 30, and 33), after the new mental listings, which focused on functioning, were implemented in 1986. Awards for mental disorders continue at higher levels today.
SSA has, from time to time, conducted outreach activities to increase public awareness of the disability programs and help potentially eligible individuals apply for benefits. In 1990, a major outreach program was instituted for the SSI disability program. This program came in the aftermath of a period of deinstitutionalization of the disabled, particularly those with mental disorders, and an increase in homelessness. The outreach efforts probably contributed not only to the increase in the SSI recipient population but also to an increase in concurrent beneficiaries (that is, persons eligible for disability benefits under both Social Security and SSI) in the early 1990s.
The Zebley court case was initiated by advocates for children with disabilities who objected to disability decisions for children that were based solely on the medical listings as not being of comparable severity to adult standards of severity, as stated in the law. The decision process had no consideration of factors that contributed to disability at a level that was less severe than that in the listings (that is, there was no decision equivalent to steps 4 and 5 in the adult decision process). In 1990, the U.S. Supreme Court ruled for the plaintiffs, and SSA was required to make changes to the way claims for SSI disabled children were decided. The new decision process centered on the functioning of the child (for example, age-appropriate behavior), and, as with the mental listings for adult applicants, the number of awards rose quickly. The number of SSI child recipients more than tripled between 1989 (before Zebley) and 1995. The number of SSI awards to children based on mental disorders increased significantly, with a heightened awareness surrounding attention deficit hyperactivity disorder (ADHD) and mental disorders that resulted in maladaptive behavior. Awards for low birth weight also increased dramatically.
In 1996, Congress passed reform legislation that resulted in changes to the way noncitizens were treated by the SSI program and eliminated drug addiction and alcoholism (DA&A) as the basis for a finding of disability. These changes probably produced only small changes in awards. The effect of the DA&A change probably had a larger effect on the SSI program than it did on the DI program, since it led to larger numbers of SSI terminations. Later that same year, welfare reform legislation changed the Zebley-based criteria for SSI children and may have reduced SSI awards to children, because the comparable severity standard was replaced with a stricter requirement of "marked and severe functional limitations." The legislation also ended the use of individualized functional assessment, and it targeted mental disorders that manifested themselves as maladaptive behavior.
Other internal policy changes have occurred within the disability programs that are too numerous to mention. There have been revisions to medical listings, including elimination of the obesity listing in 1999 and the issuance of new musculoskeletal listings in 2002.
There are also nondisability policy changes that influence the disability programs. Legislation in 1983 designed to make the Social Security program solvent raised the age for full retirement to 67 in staged increases. Early retirement is still available for persons aged 62, but beginning in 2003 the larger actuarial reduction for persons younger than the full retirement age may serve to increase the attractiveness of the DI program. Although it is too early to know with certainty the magnitude of the effect on the DI program, there are many reasons to believe this change is likely to increase the number of DI beneficiaries. The number of older beneficiaries entering the DI program will increase as the retirement age increases to 67 and additional older workers are eligible for the DI program. The increase in the full retirement age to 67 will also result in longer stays on the DI rolls for many beneficiaries, since conversion to the retirement program will occur at older ages. Again, the increase in the full retirement age could increase incentives to seek disability benefits, particularly for persons in their 60s who face higher actuarial reductions for early retirement.
Disability awards for mental disorders
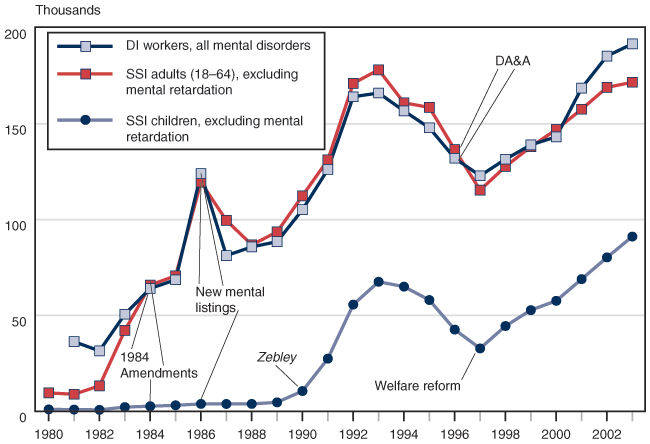
New mental listings put in place in 1986 seem to have led to continuing increases in the number of awards for mental disorders other than mental retardation, initially from the 1984 backlog and then continuing for several more years. Changes from welfare reform legislation, which mandated a stricter definition of disability for children and which were put in place in late 1996, do not seem to have reduced awards to SSI children with mental disorders, because these awards began to increase shortly thereafter.
| Year | DI workers, all mental disorders |
SSI adults (18–64), excluding mental retardation |
SSI children, excluding mental retardation |
|---|---|---|---|
| 1980 | . . . | 9.60 | 0.98 |
| 1981 | 36.32 | 8.89 | 0.91 |
| 1982 | 31.53 | 13.30 | 0.77 |
| 1983 | 50.63 | 42.18 | 2.21 |
| 1984 | 64.08 | 65.89 | 2.65 |
| 1985 | 68.61 | 70.67 | 3.14 |
| 1986 | 123.98 | 119.48 | 3.85 |
| 1987 | 81.24 | 99.58 | 3.83 |
| 1988 | 85.76 | 86.87 | 3.86 |
| 1989 | 88.50 | 93.56 | 4.67 |
| 1990 | 105.17 | 112.42 | 10.58 |
| 1991 | 126.18 | 131.16 | 27.47 |
| 1992 | 164.09 | 171.09 | 55.66 |
| 1993 | 166.05 | 178.13 | 67.57 |
| 1994 | 156.70 | 160.94 | 65.04 |
| 1995 | 147.90 | 158.51 | 58.05 |
| 1996 | 132.02 | 136.48 | 42.62 |
| 1997 | 122.90 | 115.40 | 32.80 |
| 1998 | 131.50 | 127.70 | 44.48 |
| 1999 | 138.98 | 138.02 | 52.79 |
| 2000 | 143.20 | 146.93 | 57.64 |
| 2001 | 168.60 | 157.59 | 68.94 |
| 2002 | 185.31 | 168.97 | 80.28 |
| 2003 | 191.68 | 171.65 | 91.16 |
| . . . = not applicable. | |||
In the 1984 Amendments, Congress mandated that SSA develop new disability standards for individuals with mental disorders, including mandatory specialist reviews of denials. Awards for mental disorders continued to increase after new mental listings, which focused on functioning, were implemented in 1986, and they continue at higher levels today.
The Zebley court case in 1990 resulted in new disability criteria for deciding claims for SSI disabled children's benefits. The new criteria centered on the functioning of the child (for example, age-appropriate behavior), and the program saw awards to children increase dramatically and the number of SSI child recipients more than triple between 1989 (before Zebley) and 1995. A significant portion of the increase in awards involved mental disorders other than mental retardation, with much attention directed at awards based on attention deficit hyperactivity disorder (ADHD) and various mental disorders manifesting themselves in maladaptive behaviors.
Welfare reform legislation passed by Congress in 1996 changed the definition of disability for SSI children, eliminating the individualized functional assessment and certain references to maladaptive behaviors in the mental listings that had been in place since 1991, pursuant to the Zebley decision. This change established a listings-level standard for disabled children under the SSI program that could be expected to reduce awards. However, the number of SSI awards to children for mental disorders began increasing again after 1997, and in 2003 reached an all-time high.
Disability terminations
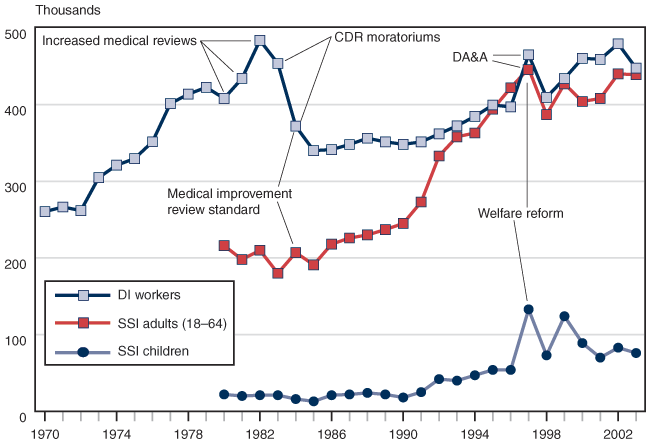
Policy changes enacted in 1980 and accelerated reviews in 1982 and 1983 increased the number of terminations. The moratoriums on continuing disability reviews on mental disorders in 1983 and on all CDRs in 1984 and the adoption of the medical improvement review standard resulted in large reductions in terminations.
| Year | DI workers | SSI adults (18–64) | SSI children |
|---|---|---|---|
| 1970 | 260.44 | . . . | . . . |
| 1971 | 266.47 | . . . | . . . |
| 1972 | 261.74 | . . . | . . . |
| 1973 | 304.79 | . . . | . . . |
| 1974 | 320.96 | . . . | . . . |
| 1975 | 329.53 | . . . | . . . |
| 1976 | 351.50 | . . . | . . . |
| 1977 | 401.33 | . . . | . . . |
| 1978 | 413.57 | . . . | . . . |
| 1979 | 422.50 | . . . | . . . |
| 1980 | 408.05 | 216.00 | 22.00 |
| 1981 | 434.19 | 198.00 | 20.00 |
| 1982 | 483.85 | 210.00 | 21.00 |
| 1983 | 453.62 | 180.00 | 21.00 |
| 1984 | 371.91 | 207.00 | 16.00 |
| 1985 | 339.98 | 191.00 | 13.00 |
| 1986 | 341.28 | 218.00 | 21.00 |
| 1987 | 347.95 | 226.00 | 22.00 |
| 1988 | 356.14 | 230.00 | 24.00 |
| 1989 | 351.40 | 237.00 | 22.00 |
| 1990 | 348.19 | 245.00 | 18.00 |
| 1991 | 351.30 | 273.00 | 25.00 |
| 1992 | 361.80 | 333.00 | 42.00 |
| 1993 | 372.32 | 358.00 | 40.00 |
| 1994 | 384.59 | 363.00 | 47.00 |
| 1995 | 399.48 | 394.00 | 54.00 |
| 1996 | 396.98 | 422.00 | 54.00 |
| 1997 | 464.98 | 447.00 | 133.00 |
| 1998 | 409.49 | 387.00 | 73.00 |
| 1999 | 433.95 | 427.00 | 124.00 |
| 2000 | 460.35 | 404.00 | 89.00 |
| 2001 | 459.07 | 408.00 | 70.00 |
| 2002 | 479.36 | 440.00 | 83.00 |
| 2003 | 447.49 | 439.00 | 76.00 |
| NOTE: . . . = not applicable. | |||
The 1980 Amendments included a requirement that SSA conduct continuing disability reviews (CDRs) every 3 years, except for persons expected to be permanently disabled.1 In the early 1980s, these medical reviews were accelerated, with large numbers of beneficiaries terminated by the reviews under a new standard. The outcry over the high termination rate, as well as numerous court cases, led to a nationwide moratorium on continuing disability reviews for most mental disorders in 1983 and for all cases in 1984, although some states had suspended all CDRs before the national moratoriums.
In 1986, SSA began to conduct CDRs again, employing the new medical improvement review standard mandated by Congress in the 1984 Amendments. In 1994, legislation (P.L. 103-296) mandated that SSA conduct continuing disability reviews on a minimum of 100,000 SSI recipients a year from 1996 to 1998. Before 1996, very few CDRs were conducted on SSI recipients, and the reviews were predominantly on concurrent beneficiaries receiving Social Security benefits.
In 1996, during the era of welfare reform, Congress enacted changes that required SSA to change disability criteria. First, in P.L. 104-121, drug addiction and alcoholism was removed as a basis for disability, which led to an increase in terminations of adults in the DI and SSI programs in 1996. That legislation also provided dedicated funding for SSA to conduct continuing disability reviews of both Social Security and SSI disability beneficiaries from 1996 to 2002. Second, legislation (P.L. 104-193) tightened the definition of disability and eligibility criteria that were established for SSI children after the Zebley decision; required redeterminations of awards to SSI children awarded on the basis of the Zebley decision that initiated individualized functional assessment and certain diagnostic criteria; mandated redeterminations that applied adult disability standards for all SSI children who were within a year of their 18th birthday; and mandated the review of all awards for low birth weight for children nearing their first birthday. These reviews and redeterminations led to an increase in terminations of SSI children in 1997 but were followed by the reinstatement of provisional benefits for some children whose payments were ceased while SSA initiated a rereview of those cases. Terminations peaked a second time in 1999 as appeals were exhausted and SSA rereviews were completed.
Disability terminations for return to work
It does not appear that policy changes have resulted in any significant increases in successful returns to work. Consequently, changes in policy appear to have had little influence on termination rates.
There have been various changes to program work incentives to encourage return to work and increase program exit, although it does not appear that any of these changes resulted in any significant increase in successful return to work and consequently appear to have done little to influence termination rates.
The 1980 Amendments made several major changes to work incentives. A 15-month extended period of eligibility, which permits beneficiaries whose disability benefits are ceased because of work to regain their benefits if their earnings fall below the substantial gainful activity level, and a 36-month period of extended Medicare were added to the Disability Insurance program. Provisions were added to the SSI program that enabled SSI recipients to work without the fear of losing cash payments or Medicaid eligibility (sections 1619a and 1619b were implemented for a limited period and were made permanent in 1986). Impairment-related work expenses were added to the SSI and DI programs, and the Plan for Achieving Self-Support was added to SSI. The 1980 Amendments eliminated the need to serve a second waiting period for cash benefits for disability beneficiaries who returned to the program within 60 months of a termination. They also eliminated a second Medicare waiting period for a disabled worker returning to the disability rolls within 60 months and for a disabled widow(er) or disabled adult child returning to the DI program within 84 months of termination.
Beginning in 1988, the extended period of eligibility was increased from 15 months to 36 months. In 1989, DI beneficiaries who exhausted their extended Medicare eligibility were permitted to buy into the Medicare program to maintain coverage.
The trial work period was established in 1960 to encourage the disabled to test their ability to work. It permitted beneficiaries to work for 9 months (which need not be consecutive) and earn as much as they were able to without losing cash benefits. Beginning in 1992, the 9-month trial work period was changed to a rolling 9 months in any 60-month period, permitting persons who failed at a work attempt to obtain additional months of trial work.
In 1999, the Ticket to Work and Work Incentives Improvement Act made further major changes to work incentives. Extended Medicare coverage was increased to 102 months from 36 months. The Ticket to Work made private vocational rehabilitation providers eligible for payments for successful rehabilitation. Under the ticket, providers receive outcome payments for months in which the beneficiary's cash benefit is suspended for work. They also have the option to elect milestone payments, which reduce later outcome payments. The legislation permits disabled beneficiaries who can no longer work an "easy-back-on" option to again receive cash payments. The law prohibits SSA from using a beneficiary's return to work to trigger a continuing disability review, prohibits termination for medical improvement if the beneficiary is using the Ticket, and precludes SSA from using evidence from work to show medical improvement. The law also authorized additional options for states to offer Medicaid buy-ins for the disabled who work.
Note
1. CDRs may be done more frequently than every 3 years, as is generally the case for persons who are expected to improve medically.