Workplace Injuries and the Take-Up of Social Security Disability Benefits
Social Security Bulletin, Vol. 72, No. 3, 2012 (released August 2012)
Workplace injuries and illnesses are an important cause of disability. State workers' compensation programs provide almost $60 billion per year in cash and medical-care benefits for those injuries and illnesses. Social Security Disability Insurance (DI) is the largest disability insurance program in the United States, with annual cash payments to disabled workers of $95 billion in 2008. Because injured workers may also receive DI benefits, it is important to understand how those two systems interact to provide benefits. This article uses matched state workers' compensation and Social Security data to study the relationship between workplace injuries and illnesses and DI benefit receipt. We find that having a lost-time injury substantially increases the probability of DI receipt, and, for people who become DI beneficiaries, those with injuries receive DI benefits at younger ages. This relationship remains robust even after we account for important personal and work characteristics.
Paul O'Leary is an economist with the Office of Program Development and Research, Social Security Administration; Leslie Boden is a professor with the Department of Environmental Health, Boston University School of Public Health; Seth Seabury is an economist at the RAND Corporation; Al Ozonoff is director of biostatistics, Clinical Research Program, Children's Hospital Boston; and Ethan Scherer is a graduate student, Pardee RAND Graduate School.
Acknowledgments: The National Institute for Occupational Safety and Health (grant number R01-OH009267) and the state of California's Commission on Health and Safety and Workers' Compensation provided support for this work. We thank the New Mexico Workers' Compensation Administration, which has generously provided the workers' compensation data on which we base this article and responded to many questions about its data and system. Finally, we thank Robert T. Reville who has provided many useful insights in the development of this research.
Contents of this publication are not copyrighted; any items may be reprinted, but citation of the Social Security Bulletin as the source is requested. The findings and conclusions presented in the Bulletin are those of the authors and do not necessarily represent the views of the Social Security Administration, the California Commission on Health and Safety and Workers' Compensation, or the New Mexico Workers' Compensation Administration.
Introduction
| DER | Detailed Earnings Record |
| DI | Disability Insurance |
| EIN | employer identification number |
| IRS | Internal Revenue Service |
| MBR | Master Beneficiary Record |
| MEF | Master Earnings File |
| PPD | permanent partial disability |
| PTD | permanent total disability |
| SSA | Social Security Administration |
| WCA | Workers' Compensation Administration (New Mexico) |
A substantial proportion of disability in the United States is caused by injuries and illnesses that arise because of an individual's work (Leigh and others 2000; Reville and Schoeni 2004; Smith and others 2005). State workers' compensation programs provide cash benefits and medical-care benefits for work-related injuries and illnesses, but people with residual disability from workplace injuries may also be eligible for Social Security Disability Insurance (DI) and related Medicare benefits. Although workers' compensation and DI are the two largest social insurance programs targeting people with disabilities, there is a lack of understanding of how the systems interact and influence worker behavior. This article uses matched state workers' compensation and Social Security data to estimate whether workplace injuries and illnesses increase the probability of receiving DI benefits, the extent of any increase that occurs, and, whether people who become DI beneficiaries receive benefits at younger ages than the typical DI beneficiary.
Workers' compensation systems provide medical and cash benefits to workers injured on the job. Workers' compensation insurance or self-insurance is mandatory for well over 90 percent of employees in all states except Texas (Sengupta, Reno, and Burton 2011) and begins on the first day of employment. By statute, workers' compensation benefits typically cover all necessary medical expenses and part of lost earnings related to workplace injuries. Most workers' compensation cases are medical-only cases, with no payment of cash benefits to replace lost earnings. To be eligible for cash benefits, a worker must have a temporary disability exceeding the state's waiting period, which varies from 3 to 7 days, or must have a permanent disability. Statutory replacement of lost earnings for temporary disabilities is typically two-thirds of lost earnings, capped at a maximum that varies by state. Temporary disability benefits are paid until the workers' compensation system regards the worker as having reached maximum recovery from the injury. If the worker can return to employment at the preinjury earnings level, cash benefits for temporary disability cease. If the worker still has permanent functional impairment or lost earnings capacity, the employer or insurer may be responsible for permanent disability benefits. In turn, permanent disabilities can be either total (with virtually no residual earning capacity) or partial (where residual earning capacity remains). State systems for paying permanent partial disability (PPD) benefits vary widely (see Burton (2005) and Barth and Niss (1999)), and describing those systems is outside the scope of this article. In most states, however, PPD benefits are evaluated as a percentage of total disability. That percentage is then applied either to a statutory number of weeks of benefits (for example, $400 per week paid for 10 percent of 500 weeks equals 50 weeks) or to a weekly benefit rate that is paid for a set number of weeks (for example, 10 percent of $400 per week paid for 500 weeks). In some states, PPD benefits are paid based on the difference between current earnings and preinjury earnings (wage loss).
Most employers or insurers pay workers' compensation without contest, with benefits determined by the payer applying their respective state's laws and regulations. If a dispute arises about work-relatedness—when temporary disability benefits should end, the extent of permanent disability, or some other unresolved issue—it is adjudicated in almost all states by hearing officers or administrative law judges.
In this study, we examine DI outcomes for workers' compensation cases from New Mexico. During the study period, the New Mexico workers' compensation waiting period for temporary disability benefits was 7 days. The maximum weekly benefit was 85 percent of the state average weekly wage until 2000, when it was raised to 100 percent. To categorize injury severity, we classify workers' compensation cases by the highest level of disability payment (from low to high: medical-only, temporary disability, PPD, and permanent total disability (PTD)). About 70 percent of workers' compensation cases in New Mexico involved only medical benefits. Of lost-time cases, 73 percent were for temporary disability only, and 27 percent involved PPD. Less than 0.5 percent of lost-time cases resulted in payment of PTD benefits.
DI benefits may also be available to injured workers, although coverage of injuries is narrower in scope. First, DI benefits are only available to workers with a total disability expected to last at least 12 months or end in death. In that sense, those benefits are similar to workers' compensation for workers with PTDs. If anything, the workers' compensation definition appears more stringent because under that system permanent total disability is expected to last throughout the work life. However, the relationship in practice is determined by the decision-making process of the two systems, which is not completely codified in law or regulation. Of course, workers' compensation covers a much wider range of injuries, including those involving no lost time from work, those involving short-term disability, and those involving PPD.
Unlike workers' compensation benefits, DI benefits are available to individuals (and their families) only after they have established a sufficient work history.1 Despite the close relationship between employment history and DI, we know very little about the extent to which individuals' employment experiences contribute to disability and eventual receipt of disability benefits covered under the Social Security Administration (SSA). Those experiences include injuries at work.
The formal relationship between DI and workers' compensation is governed by a legally mandated offset program. The offset—which Congress included in the original 1956 Social Security disability program and then rescinded in 1958 and reestablished in 1965 (Reno, Williams, and Sengupta 2003)—limits the amount paid to injured workers receiving benefits from both DI and workers' compensation to a maximum of 80 percent of the worker's preinjury average earnings. Depending on the state, either SSA or the state reduces benefits such that the combined DI and workers' compensation benefits do not exceed 80 percent of prior earnings.2 In New Mexico, DI benefits are reduced if the 80 percent cap is exceeded.
The stakes in understanding how Social Security's DI program and workers' compensation interact are high because they comprise the two largest disability benefit programs in the United States. Workers' compensation paid benefits to 4 million workers in 2008 at a total cost approaching $60 billion, almost equally split between cash and medical benefits. DI in 2008 was nearly three times the size of workers' compensation, with 7.4 million disabled-worker beneficiaries at a cost of $95 billion in cash benefits, while Medicare health-care benefits for people with disabilities who were younger than age 65 totaled over $54 billion (Sengupta, Reno, and Burton 2011; SSA 2011a, 2011b).3 Both the DI and workers' compensation programs have been growing in the past two decades, but the growth in workers' compensation has been modest in comparison to DI. From 1987 through 2008, workers' compensation cash benefits increased by 65 percent while DI cash benefits grew by 403 percent (Sengupta, Reno, and Burton 2011; SSA 2011a4).
There is evidence that the effect of work-related injuries on the eventual receipt of DI benefits could be significant. Reville and Schoeni (2004) used data from the 1992 Health and Retirement Survey to estimate the proportion of disabilities caused by work. Using a narrow definition—disability caused by injury at work—they estimated that 17 percent of the disabled population aged 51–61 attributed their disability to work. That proportion grew to 36 percent under a broader definition of work-relatedness. The proportion attributing their disability to work was almost identical among those receiving DI benefits. The authors indicated that work-related limitations are a substantial contributor to overall disability rates and that DI is an important source of insurance for work-related disability. Given that work and work-related hazards are significant contributors to long-term disabilities, it is noteworthy that workers' compensation has not grown at a similar rate when compared with DI. There are differing views on the various causes of the growth in the DI rolls, but there is some consensus that much of that growth can be explained by simple inflation, the expanded labor force participation of women, and changes in disability policy in the late 1980s that led to increased awards, especially for younger individuals (Rupp and Stapleton 1995; Burkhauser and Daly 2002; Autor and Duggan 2006). Although DI and workers compensation programs differ in important ways, they serve the same populations and face many of the same demographic, social, and economic changes. As such, it is interesting that the growth rates exhibit such different patterns.
Researchers have hypothesized that workers' compensation and DI do not move together because injured workers substitute one program's benefits for the other's, as the relative value or ease of obtaining benefits changes. Sengupta, Reno, and Burton (2011) examined DI and workers' compensation cash benefits per $100 of wages in the 1980–2007 period and found that the trends for the two programs were nearly mirror opposites of each other. As cash benefits as a percentage of covered wages rose for workers' compensation from 1980 through 1991, there was a corresponding decline for DI. Then as the percentage of covered wages leveled out and subsequently declined for workers' compensation from 1992 through 2007, the authors noted movement of comparable magnitude for DI in the opposite direction. Other researchers have examined these potential substitution effects and have found that declines in the statutory cash benefit levels of workers' compensation and their more restrictive eligibility rules were both associated with increases in DI applications from 1985 through 1999 (Guo and Burton 2008).5 Guo and Burton further suggested that such changes have reduced employer safety incentives and efficiency by shifting injury costs from employers, who have the ability to affect injury risks, to SSA, which does not. However, a recent paper by McInerney and Simon (2012) did not support the Guo and Burton results. McInerney and Simon examined the relationship between DI and workers' compensation receipt within states over time. They found that the overall inverse relationship between DI and workers' compensation payments did not hold within states. Instead, the authors concluded that the increases in DI occurred in states other than those with reductions in workers' compensation.
While changes in workers' compensation laws may or may not have contributed to the large increase in receipt of DI benefits, workplace injuries almost certainly add to the DI rolls. We test that hypothesis and examine the size of any workers' compensation effect on the DI program. Further, we examine the extent to which the large sizes of the two programs lead to significant DI costs. This research adds to the evidence of a causal linkage between work-related injuries and DI by using survival analyses to estimate the time-specific probability of receiving DI among people with workers' compensation injuries.
Beyond access to workers' compensation coverage and the way those benefits interact with DI benefits, states also differ in terms of the kinds of injuries covered and the level of benefits provided. Understanding the linkage between workers' compensation benefits and the DI program could help SSA in developing cooperative programs with states to improve incentives to minimize the long-term severity of injuries. This could improve retention of workers in the labor market and reduce costs for the DI program. In this analysis, we look at the extent to which injuries on the job in New Mexico ultimately lead to receipt of DI benefits.
SSA maintains some information on workers' compensation claims to manage the offset provisions. However, the workers' compensation benefits data maintained by SSA are self-reported, and there are no existing automated data matches with states.6 For reported workers' compensation benefits, SSA individually verifies the type and amount with the workers' compensation provider before adjusting DI payments, but there are no means for SSA to check for unreported workers' compensation claims. In our analysis, we match New Mexico state workers' compensation data to Social Security administrative data and Internal Revenue Service (IRS) earnings data. This provides a unique, rich data resource that allows us to integrate many details about both the nature and timing of the workers' compensation injury and any DI benefits that may result.
Using our matched data, we examine the proportion of injured workers who have received workers' compensation benefits and who eventually receive DI benefits and the age at which they transition to Social Security benefits. We also examine the extent to which employer and individual characteristics affect the propensity for workers' compensation injuries leading to DI benefits and the timing of those benefits. This information should improve our understanding of the relationship between workplace injuries and receipt of DI benefits.
Data
The New Mexico Workers' Compensation Administration (WCA) provided us with data on all cases with injury dates from 1992 through 2001 for which workers' compensation benefits were paid (N = 214,230). The data included information on the characteristics of the injured worker, the injury and the employer, compensated time lost from work, and benefits paid. New Mexico has a 7-day waiting period for temporary disability benefits, so cash benefits are only paid for cases involving more than 7 days lost from work or for permanent disability. From 1992 through 2001, there were 63,689 lost-time cases (30 percent of the total). The remaining 150,541 cases (70 percent) comprised workers who received only medical-care benefits.
Thirty-eight percent of the WCA sample had more than one workplace injury from 1992 through 2001. That is important because the first injury might causally affect the occurrence and impact of subsequent injuries. Because we do not observe individuals before 1992, some of the injuries, particularly in the early years of our sample, may not have been the first injury. For that reason, we removed workers whose first observed injury occurred in 1992 or 1993 as a compromise between reducing the number of subsequent injuries included in the analysis and maintaining sample size. In our data, 22 percent of workers have more than one injury, and 49 percent of second injuries occur within 2 years of the first injury.
We excluded injuries in 2001 to provide a longer observation period after the date of initial injury.7 This offers a clearer picture of the final status of cases. Finally, we eliminated death claims. After those exclusions, 156,961 cases in the workers' compensation file remained. Our sample consisted of 44,675 lost-time cases and 112,286 medical-only cases—categorized by the highest level of disability benefits paid. About 8 percent of lost-time cases included a lump-sum payment. We categorized those as PPD cases unless PTD benefits were paid, at which point we considered them to be PTD cases.
For people receiving DI benefits, eligibility for DI terminates at full Social Security retirement age. At full retirement age, workers are also no longer eligible for new DI benefits. In both cases, workers can receive Social Security retirement benefits instead. To provide an adequate postinjury observation period, we excluded workers aged 55 or older at the date of injury. We also excluded workers with a reported age younger than 15. After those restrictions, our sample consisted of 140,951 injury cases, of which 101,645 were medical-only and 39,306 were lost-time cases.
Using Social Security's Enumeration Validation System, based on the master files of Social Security number (SSN) holders and SSN applications (NUMIDENT), we verified the SSNs of injured workers using the WCA-provided SSN, name, date of birth, and sex of each injured worker. The NUMIDENT is a computer database that contains an abstract of the information submitted for SSN applications. Approximately 96 percent of our sample has valid SSNs. Using the validated SSN, we linked each worker to his or her Detailed Earnings Record (DER) from Social Security's Master Earnings File (MEF), retrieving annual earnings through the end of 2009. SSA derives the MEF data from IRS Form W-2, quarterly earnings records, and annual income tax forms.8 Those data include regular wages and salaries for Federal Insurance Contribution Act–covered and noncovered workers, tips, self-employment income, and deferred compensation. There may be multiple sources of earnings in any given year. Using the DER, we determined the "employer of injury." If the employer identification number (EIN) in the WCA file matched any of the EINs in the IRS data for that year, we used that EIN. In cases where none of the EINs matched, or the WCA EIN was missing in the WCA file, we used the IRS EIN that represented the highest earnings in the year of injury.
We kept one injury record for each injured worker and considered the index injury to be the first lost-time injury in the data. If a worker incurred exclusively medical-only injuries, we considered the first of those as the index injury. We also dropped cases for which the initial receipt of DI benefits preceded the index injury. That reduced our analytic sample to 98,148 cases, of which 65,705 (67 percent) were medical-only and 32,443 (33 percent) were lost-time.
We then matched the injured workers in our sample with validated SSNs to data from Social Security's Ticket Research File (TRF).9 The TRF draws data from various Social Security administrative files into a single record for each beneficiary who has received benefits based on disability since 1996.10 For our analysis, we focus primarily on data from the Master Beneficiary Record (MBR) as contained in the TRF. The MBR contains information about all recipients of Old-Age, Survivors, or Disability Insurance cash benefits. It includes their dates and types of eligibility, payment amounts, and other demographic and benefit characteristics. We matched injured workers in the sample to the TRF to determine whether they began receiving DI benefits between the date of injury and the end of 2009, based on the date SSA determined those individuals to be eligible to receive DI cash benefits.11 The eligibility date for DI receipt provides us with the dependent variable in the survival analysis. Death is a censoring event, so we also used the Social Security Death Master File from the NUMIDENT to derive dates of death.12
Methods
To measure the impact of workplace injuries on DI receipt directly, we must observe an individual's probability of receiving DI under both injured and uninjured circumstances. However, it is impossible to observe workers simultaneously as both injured and uninjured. Instead, we used the cumulative hazard of receipt of DI for medical-only workers to estimate the counterfactual probability of receiving DI absent an injury. By "cumulative hazard," we mean the probability (as a function of time T) that an individual will receive DI by time T after the date of injury. In the analysis, we measure time in 3-month increments, although our results are presented in a scale of years. Because medical-only cases involve 7 or fewer days off work, the underlying severity of the injuries is low and should result in little to no long-term physical impairment. Thus, we expect that the underlying risk of long-term total disability for workers with medical-only injuries should be approximately equal to that of an uninjured worker. We can approximate the increased hazard of DI receipt from lost workday injuries by estimating the difference between the probability of DI receipt for workers with lost-time injuries and those of workers with medical-only injuries.13
All analyses were performed using SAS 9.2.14 We derived separate Kaplan-Meier curves to estimate the length of time to DI receipt for workers with lost-time and medical-only injuries. We also derived age-specific Kaplan-Meier curves because age is strongly and positively related to disability (Chart 1). Although the Kaplan-Meier curves have the advantage of being nonparametric and easy to interpret, they fail to account for potentially confounding covariates.
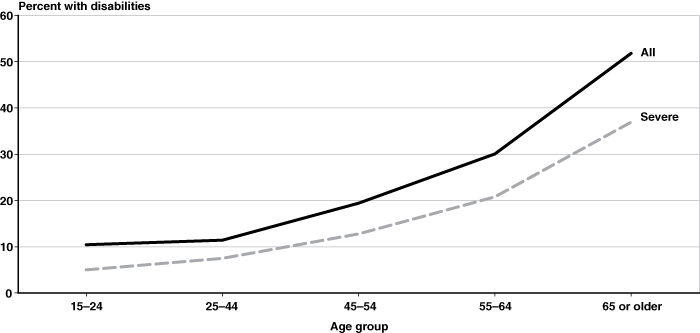
Relationship between age and disability: US population, 2005
| Age group | All | Severe |
|---|---|---|
| 15–24 | 10.4 | 5.0 |
| 25–44 | 11.4 | 7.5 |
| 45–54 | 19.4 | 12.8 |
| 55–64 | 30.1 | 20.8 |
| 65 or older | 51.8 | 36.9 |
- Had difficulty performing one or more functional activities, which include seeing, hearing, speaking, lifting/carrying, using stairs, walking, or grasping small objects
- Had difficulty with one or more activities of daily living (ADLs), which include getting around inside the home, getting in or out of bed or a chair, bathing, dressing, eating, and toileting
- Had difficulty with one or more instrumental ADLs, which include going outside the home, keeping track of money and bills, preparing meals, doing light housework, taking prescription medicines in the right amount at the right time, and using the telephone
- Had one or more specified conditions: a learning disability or some other type of mental or emotional condition
- Used a wheelchair, a cane, crutches, or a walker
- Was unable to perform or needed help to perform one or more of the functional activities
- Was unable to perform or needed help to perform one or more ADLs
- Had one or more specified conditions: a developmental disability or Alzheimer's disease
- Had any other mental or emotional condition that seriously interfered with everyday activities
- Had a condition that limited the ability to work around the house or made it difficult to remain employed
To account for other covariates, we estimated Cox proportional hazards models for workers with lost-time and medical-only injuries, controlling for the employer's size and 2-digit industry category; the injured worker's sex, his or her preinjury earnings category, and age category; and injury severity as measured by workers' compensation benefit categories. Those categories are medical-only, temporary disability of less than 8 weeks, temporary disability of at least 8 weeks, PPD, and PTD. We chose to distinguish workers with more than 8 weeks off work because research suggests that lost earnings are much larger for such workers as compared with workers with less lost time (Boden and Galizzi 1999). The Cox model allows us to estimate the length of time to DI receipt for lost-workday injuries relative to medical-only injuries. We interpret hazard ratios estimated from this model as the relative likelihood of receiving DI benefits at any point in time for a particular subgroup relative to its reference group.
A key assumption of the Cox proportional hazards model is that the hazard ratio is constant over time. We tested the proportional hazards assumption by adding interactions between time and the other covariates to the basic model. We used two separate time variables: a linear trend and a dummy variable for more than 5 years after injury. For variables violating the proportionality assumption, we reestimated the Cox model separately for medical-only and lost-time cases, stratifying on those variables to derive cumulative hazard curves for the lost-time cases.15 In addition, we estimated the counterfactual cumulative hazard by applying the medical-only estimates to the covariate values of the lost-time cases, providing a predicted probability of DI receipt if the lost-time injuries had been medical-only cases.
Finally, we estimated the Cox model for all workers in our sample, allowing the hazard to vary by severity group based on workers' compensation benefit status. From this, we derived cumulative hazard curves comparing expected probability of DI receipt for the population of injured workers had they experienced injuries of differing severity.
All survival models were right-censored using the earliest of four dates: the date of full retirement age when individuals are no longer eligible for DI benefits, the date of death, the first date after injury when the person was ineligible for benefits because of insufficient work credits, and the end of the observation period (December 31, 2009). We censored at the first date of ineligibility because take-up of DI benefits is not possible during periods of ineligibility. Even though people may later have become eligible for benefits and some information would be lost, these are censored outcomes and thus should not bias estimates of the hazard ratio.
We did not adjust for what is known as the disability freeze. Technically, workers who are insured for DI at the time of their injury would not lose DI-insured status in subsequent months if their work or earnings dropped because of their disability. SSA uses recent work credits to establish DI-insured status, but SSA freezes the insured status and benefit levels for DI and retirement benefits at the predisability levels if an individual's earnings while disabled in the period prior to DI award would make him or her ineligible for benefits or reduce the level of benefits he or she would receive. We do not make this adjustment in the analysis for two reasons. First, the disability freeze applies to any SSA defined disability—one that prevents substantial gainful activity and are expected to last for 12 months or end in death. Most workers' compensation PTD cases would likely qualify, but many PPD cases may qualify as well, as would other disabilities that are present at the time of injury or occur after the workers' compensation injury. We have no means of accurately applying the disability freeze for all injured workers so we apply it to none of them. Second, ignoring the disability freeze is the more conservative approach in that fewer injured workers would be insured for DI at any given point in time postinjury. As described later, we find that eligibility has little effect on our findings under this extreme case, so adjusting for the disability freeze would not substantially affect the results.
Results
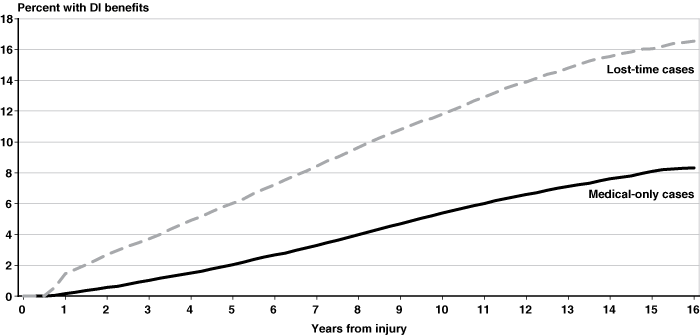
Table 1 provides descriptive statistics for medical-only and lost-time cases. The first column reports the average for all claims, while the third and fifth columns report the averages for the medical-only and lost-time cases, respectively. On average, people with lost-time injuries were older, worked in larger firms, worked in the private sector, had lower earnings, and were less likely to be female than those with medical-only injuries. Both 5 years and 10 years after injury, the proportion of people with lost-time injuries who had become DI beneficiaries was about double that for medical-only cases. We can see this relationship graphically in Chart 2, which shows separate Kaplan-Meier curves for medical-only and lost-time cases. Some of the disparity in the probability of DI receipt may be related to differences in characteristics between the medical-only and lost-time groups.
| Characteristic | All claims | Medical-only cases | Lost-time cases | |||
|---|---|---|---|---|---|---|
| Average | Standard deviation | Average | Standard deviation | Average | Standard deviation | |
| Individual | ||||||
| Age (years) | 34.5 | 9.9 | 33.9 | 9.9 | 35.7 | 9.7 |
| Female (%) | 0.37 | 0.48 | 0.39 | 0.49 | 0.34 | 0.47 |
| Employer | ||||||
| Number of employees | 32,410 | 161,381 | 30,238 | 155,883 | 36,810 | 171,898 |
| Median | 532 | 611 | 415 | |||
| Public sector (%) | 0.13 | 0.33 | 0.14 | 0.35 | 0.10 | 0.30 |
| Claim (%) | ||||||
| Medical-only | 0.67 | 0.47 | 1.00 | 0.00 | 0.00 | 0.00 |
| Temporary disability, less than 8 weeks | 0.19 | 0.39 | . . . | . . . | 0.57 | 0.50 |
| Temporary disability, at least 8 weeks | 0.05 | 0.22 | . . . | . . . | 0.16 | 0.37 |
| Permanent partial disability | 0.09 | 0.28 | . . . | . . . | 0.27 | 0.44 |
| Permanent total disability | 0.001 | 0.04 | . . . | . . . | 0.004 | 0.07 |
| Earnings, year before injury (2007 $) | 23,044 | 20,264 | 23,792 | 21,441 | 21,530 | 17,544 |
| Median | 19,409 | 20,071 | 18,144 | |||
| Proportion receiving DI within— | ||||||
| 5 years of injury | 0.03 | 0.17 | 0.02 | 0.14 | 0.05 | 0.22 |
| 10 years of injury a | 0.07 | 0.25 | 0.05 | 0.22 | 0.10 | 0.30 |
| Number of observations | 98,148 | 65,705 | 32,443 | |||
| SOURCE: Authors' analysis of New Mexico workers' compensation claims from 1994 through 2000 matched to Social Security administrative data. | ||||||
| NOTE: . . . = not applicable. | ||||||
| a. Some workers were no longer eligible for DI benefits by the end of the 10-year period. They were not included in the calculation. | ||||||
Receipt of DI benefits among medical-only and lost-time cases: Kaplan-Meier curves
| Years from injury | Medical-only cases | Lost-time cases |
|---|---|---|
| 0 | 0.00 | 0.00 |
| 0.25 | 0.00 | 0.00 |
| 0.5 | 0.01 | 0.03 |
| 0.75 | 0.04 | 0.57 |
| 1 | 0.16 | 1.45 |
| 1.25 | 0.25 | 1.74 |
| 1.5 | 0.36 | 2.04 |
| 1.75 | 0.46 | 2.35 |
| 2 | 0.56 | 2.70 |
| 2.25 | 0.64 | 2.97 |
| 2.5 | 0.76 | 3.24 |
| 2.75 | 0.91 | 3.46 |
| 3 | 1.02 | 3.72 |
| 3.25 | 1.15 | 4.00 |
| 3.5 | 1.27 | 4.33 |
| 3.75 | 1.38 | 4.63 |
| 4 | 1.50 | 4.91 |
| 4.25 | 1.62 | 5.17 |
| 4.5 | 1.76 | 5.49 |
| 4.75 | 1.91 | 5.79 |
| 5 | 2.05 | 6.02 |
| 5.25 | 2.21 | 6.29 |
| 5.5 | 2.38 | 6.67 |
| 5.75 | 2.53 | 6.96 |
| 6 | 2.68 | 7.24 |
| 6.25 | 2.79 | 7.55 |
| 6.5 | 2.97 | 7.83 |
| 6.75 | 3.12 | 8.11 |
| 7 | 3.28 | 8.44 |
| 7.25 | 3.46 | 8.76 |
| 7.5 | 3.63 | 9.03 |
| 7.75 | 3.80 | 9.33 |
| 8 | 3.98 | 9.66 |
| 8.25 | 4.17 | 9.97 |
| 8.5 | 4.35 | 10.27 |
| 8.75 | 4.53 | 10.53 |
| 9 | 4.70 | 10.80 |
| 9.25 | 4.87 | 11.08 |
| 9.5 | 5.06 | 11.35 |
| 9.75 | 5.21 | 11.53 |
| 10 | 5.39 | 11.81 |
| 10.25 | 5.55 | 12.08 |
| 10.5 | 5.70 | 12.35 |
| 10.75 | 5.88 | 12.66 |
| 11 | 6.01 | 12.91 |
| 11.25 | 6.19 | 13.19 |
| 11.5 | 6.33 | 13.48 |
| 11.75 | 6.46 | 13.70 |
| 12 | 6.59 | 13.88 |
| 12.25 | 6.70 | 14.15 |
| 12.5 | 6.86 | 14.38 |
| 12.75 | 7.00 | 14.54 |
| 13 | 7.12 | 14.80 |
| 13.25 | 7.23 | 15.03 |
| 13.5 | 7.33 | 15.24 |
| 13.75 | 7.48 | 15.43 |
| 14 | 7.61 | 15.55 |
| 14.25 | 7.70 | 15.73 |
| 14.5 | 7.80 | 15.83 |
| 14.75 | 7.96 | 16.01 |
| 15 | 8.08 | 16.05 |
| 15.25 | 8.20 | 16.21 |
| 15.5 | 8.25 | 16.38 |
| 15.75 | 8.29 | 16.46 |
| 16 | 8.32 | 16.54 |
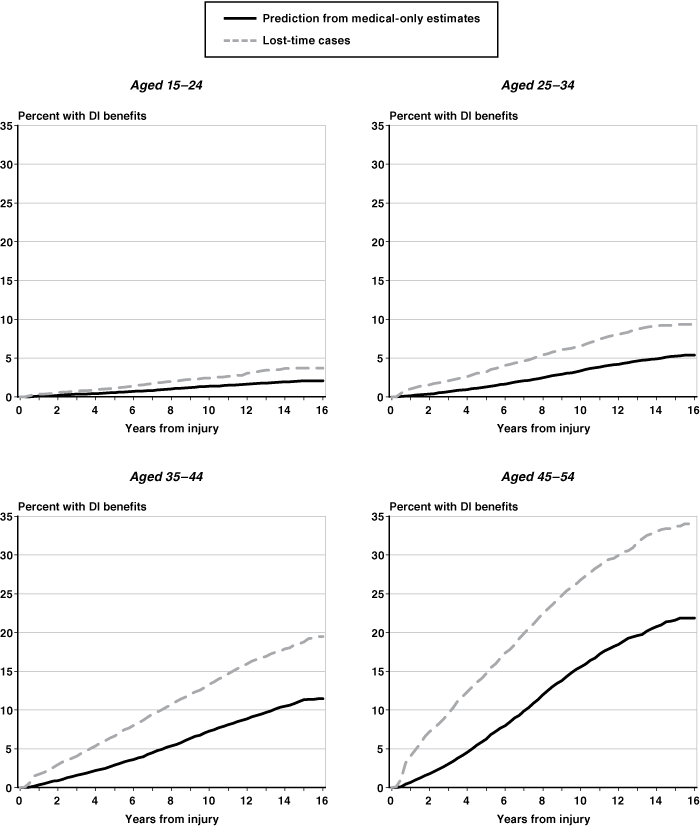
Because age is so strongly associated with disability (Chart 1), we stratified our sample by 10-year age groups to derive age-specific Kaplan-Meier curves (Chart 3). The curves show that the length of time to DI receipt differs substantially by age group. They also show that, within an age group, workers with lost-time injuries have a substantially greater probability of receiving DI benefits than those with medical-only injuries at all postinjury points in time.
Receipt of DI benefits among medical-only and lost-time cases, by age group: Kaplan-Meier curves
| Years from injury | Aged 15–24 | Aged 25–34 | Aged 35–44 | Aged 45–54 | ||||
|---|---|---|---|---|---|---|---|---|
| Prediction from medical-only estimates | Lost-time cases | Prediction from medical-only estimates | Lost-time cases | Prediction from medical-only estimates | Lost-time cases | Prediction from medical-only estimates | Lost-time cases | |
| 0 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 |
| 0.25 | 0.00 | 0.02 | 0.00 | 0.00 | 0.02 | 0.03 | 0.01 | 0.08 |
| 0.5 | 0.02 | 0.13 | 0.03 | 0.45 | 0.04 | 0.58 | 0.09 | 1.07 |
| 0.75 | 0.04 | 0.31 | 0.10 | 0.87 | 0.20 | 1.48 | 0.45 | 3.24 |
| 1 | 0.07 | 0.35 | 0.13 | 1.02 | 0.34 | 1.71 | 0.67 | 4.07 |
| 1.25 | 0.12 | 0.36 | 0.21 | 1.21 | 0.47 | 1.96 | 0.99 | 4.84 |
| 1.5 | 0.13 | 0.38 | 0.26 | 1.39 | 0.66 | 2.24 | 1.25 | 5.63 |
| 1.75 | 0.14 | 0.46 | 0.30 | 1.47 | 0.82 | 2.61 | 1.53 | 6.57 |
| 2 | 0.17 | 0.54 | 0.36 | 1.56 | 0.89 | 2.95 | 1.78 | 7.18 |
| 2.25 | 0.23 | 0.60 | 0.42 | 1.72 | 1.05 | 3.30 | 2.07 | 7.69 |
| 2.5 | 0.27 | 0.62 | 0.54 | 1.80 | 1.27 | 3.54 | 2.39 | 8.22 |
| 2.75 | 0.31 | 0.69 | 0.59 | 1.94 | 1.42 | 3.79 | 2.67 | 8.86 |
| 3 | 0.34 | 0.73 | 0.66 | 2.09 | 1.60 | 4.06 | 3.06 | 9.56 |
| 3.25 | 0.36 | 0.79 | 0.75 | 2.22 | 1.74 | 4.44 | 3.39 | 10.31 |
| 3.5 | 0.37 | 0.81 | 0.82 | 2.35 | 1.84 | 4.71 | 3.78 | 11.17 |
| 3.75 | 0.38 | 0.85 | 0.88 | 2.48 | 2.04 | 5.08 | 4.13 | 11.72 |
| 4 | 0.41 | 0.91 | 0.93 | 2.60 | 2.20 | 5.37 | 4.52 | 12.33 |
| 4.25 | 0.43 | 0.97 | 1.04 | 2.82 | 2.33 | 5.76 | 4.97 | 12.94 |
| 4.5 | 0.48 | 1.01 | 1.12 | 3.03 | 2.48 | 6.04 | 5.47 | 13.59 |
| 4.75 | 0.52 | 1.05 | 1.20 | 3.10 | 2.67 | 6.38 | 5.85 | 14.07 |
| 5 | 0.55 | 1.13 | 1.28 | 3.24 | 2.91 | 6.64 | 6.27 | 14.70 |
| 5.25 | 0.61 | 1.19 | 1.38 | 3.52 | 3.08 | 7.06 | 6.85 | 15.45 |
| 5.5 | 0.63 | 1.23 | 1.44 | 3.68 | 3.32 | 7.46 | 7.24 | 15.97 |
| 5.75 | 0.67 | 1.31 | 1.57 | 3.82 | 3.47 | 7.68 | 7.68 | 16.71 |
| 6 | 0.72 | 1.39 | 1.63 | 4.04 | 3.63 | 8.00 | 7.99 | 17.35 |
| 6.25 | 0.74 | 1.51 | 1.76 | 4.21 | 3.85 | 8.35 | 8.48 | 17.81 |
| 6.5 | 0.76 | 1.56 | 1.88 | 4.37 | 3.98 | 8.66 | 9.00 | 18.42 |
| 6.75 | 0.79 | 1.64 | 1.98 | 4.46 | 4.26 | 9.08 | 9.32 | 19.22 |
| 7 | 0.81 | 1.74 | 2.08 | 4.62 | 4.49 | 9.46 | 9.86 | 19.88 |
| 7.25 | 0.88 | 1.80 | 2.13 | 4.74 | 4.77 | 9.72 | 10.33 | 20.53 |
| 7.5 | 0.92 | 1.84 | 2.24 | 4.98 | 4.95 | 10.05 | 10.88 | 21.11 |
| 7.75 | 0.98 | 1.92 | 2.33 | 5.18 | 5.18 | 10.41 | 11.38 | 21.81 |
| 8 | 1.03 | 1.98 | 2.46 | 5.41 | 5.38 | 10.72 | 12.00 | 22.48 |
| 8.25 | 1.09 | 2.05 | 2.60 | 5.56 | 5.57 | 11.12 | 12.51 | 23.06 |
| 8.5 | 1.12 | 2.11 | 2.74 | 5.76 | 5.77 | 11.40 | 12.99 | 23.56 |
| 8.75 | 1.16 | 2.19 | 2.82 | 5.90 | 6.07 | 11.68 | 13.43 | 24.18 |
| 9 | 1.18 | 2.23 | 2.92 | 6.08 | 6.36 | 12.01 | 13.81 | 24.77 |
| 9.25 | 1.24 | 2.25 | 3.03 | 6.16 | 6.59 | 12.36 | 14.34 | 25.38 |
| 9.5 | 1.31 | 2.32 | 3.10 | 6.24 | 6.76 | 12.55 | 14.79 | 25.83 |
| 9.75 | 1.33 | 2.41 | 3.22 | 6.42 | 7.05 | 12.91 | 15.24 | 26.28 |
| 10 | 1.35 | 2.41 | 3.37 | 6.54 | 7.26 | 13.31 | 15.57 | 26.79 |
| 10.25 | 1.37 | 2.43 | 3.51 | 6.77 | 7.47 | 13.60 | 15.90 | 27.27 |
| 10.5 | 1.39 | 2.55 | 3.64 | 7.01 | 7.72 | 14.00 | 16.37 | 27.70 |
| 10.75 | 1.44 | 2.55 | 3.75 | 7.19 | 7.87 | 14.29 | 16.72 | 28.22 |
| 11 | 1.49 | 2.63 | 3.82 | 7.43 | 8.12 | 14.66 | 17.23 | 28.62 |
| 11.25 | 1.52 | 2.69 | 3.96 | 7.61 | 8.30 | 15.02 | 17.61 | 29.15 |
| 11.5 | 1.56 | 2.77 | 4.06 | 7.78 | 8.49 | 15.33 | 17.88 | 29.44 |
| 11.75 | 1.60 | 2.80 | 4.15 | 7.94 | 8.67 | 15.63 | 18.19 | 29.56 |
| 12 | 1.64 | 3.06 | 4.21 | 8.06 | 8.86 | 15.97 | 18.46 | 29.98 |
| 12.25 | 1.67 | 3.13 | 4.31 | 8.19 | 9.11 | 16.29 | 18.87 | 30.39 |
| 12.5 | 1.70 | 3.24 | 4.43 | 8.32 | 9.30 | 16.51 | 19.27 | 30.55 |
| 12.75 | 1.75 | 3.35 | 4.53 | 8.61 | 9.49 | 16.73 | 19.44 | 30.95 |
| 13 | 1.77 | 3.43 | 4.63 | 8.72 | 9.70 | 16.91 | 19.62 | 31.68 |
| 13.25 | 1.80 | 3.43 | 4.70 | 8.86 | 9.89 | 17.22 | 19.74 | 32.07 |
| 13.5 | 1.85 | 3.48 | 4.77 | 8.98 | 10.14 | 17.44 | 20.18 | 32.51 |
| 13.75 | 1.91 | 3.53 | 4.84 | 9.07 | 10.34 | 17.59 | 20.51 | 32.73 |
| 14 | 1.93 | 3.65 | 4.90 | 9.16 | 10.47 | 17.87 | 20.75 | 32.98 |
| 14.25 | 1.95 | 3.65 | 4.98 | 9.19 | 10.63 | 18.02 | 20.98 | 33.27 |
| 14.5 | 1.97 | 3.72 | 5.12 | 9.23 | 10.84 | 18.43 | 21.37 | 33.38 |
| 14.75 | 2.02 | 3.72 | 5.18 | 9.23 | 11.12 | 18.53 | 21.44 | 33.38 |
| 15 | 2.06 | 3.72 | 5.26 | 9.29 | 11.32 | 18.79 | 21.61 | 33.71 |
| 15.25 | 2.06 | 3.72 | 5.29 | 9.36 | 11.37 | 19.21 | 21.84 | 33.71 |
| 15.5 | 2.06 | 3.72 | 5.38 | 9.36 | 11.37 | 19.32 | 21.84 | 34.03 |
| 15.75 | 2.06 | 3.72 | 5.38 | 9.36 | 11.47 | 19.49 | 21.84 | 34.03 |
| 16 | 2.06 | 3.72 | 5.38 | 9.36 | 11.47 | 19.49 | 21.84 | 34.03 |
To account for differences in other relevant covariates, we estimated separate Cox proportional hazard models for medical-only and lost-time cases. Age group had the largest impact on receipt of DI, followed by the preinjury income category. (Estimated hazard ratios are available on request.) When testing for proportionality, we found significant interactions between age and the 5-year dummy variable, but not for the interaction between age and a time trend. In neither case was the time interaction for any of the preinjury income categories statistically significant.
Because the proportional hazards assumption did not seem to hold for age, we estimated the Cox model stratified by age group. We display the estimated hazard ratios and their confidence intervals for covariates stratified by age group in Table 2. For both lost-time and medical-only cases, the probability of receiving DI benefits was significantly higher for people employed in the mining industry than for other industries and for people in lower earnings categories. Estimated hazard ratios were lower for women and for workers in the smallest industry group. Aside from mining, several other industry groups had statistically significant hazard ratios for the medical-only cases, but for lost-time injuries, only the hazard ratio for mining was significant.
| Characteristic | Medical-only cases | Lost-time cases | ||
|---|---|---|---|---|
| Hazard ratio | 95 percent confidence interval | Hazard ratio | 95 percent confidence interval | |
| Individual | ||||
| Female | 0.82 | 0.77–0.88 | 0.90 | 0.84–0.97 |
| Male (reference group) | . . . | . . . | . . . | . . . |
| Employer | ||||
| 1–100 employees | 0.88 | 0.81–0.96 | 0.89 | 0.82–0.97 |
| 101–500 employees | 0.93 | 0.86–1.01 | 1.02 | 0.95–1.11 |
| 501–1,000 employees | 0.92 | 0.82–1.03 | 1.00 | 0.89–1.12 |
| 1,000 employees or more (reference group) | . . . | . . . | . . . | . . . |
| Earnings, year before injury (2007 $) | ||||
| 0–9,999 | 2.40 | 2.11–2.73 | 1.56 | 1.38–1.77 |
| 10,000–19,999 | 2.38 | 2.11–2.68 | 1.45 | 1.28–1.64 |
| 20,000–29,999 | 1.79 | 1.58–2.02 | 1.83 | 1.60–2.08 |
| 30,000–39,999 | 1.43 | 1.25–1.63 | 1.18 | 1.03–1.34 |
| 40,000–49,999 | 1.26 | 1.09–1.46 | 1.15 | 0.99–1.34 |
| 50,000 or more (reference group) | . . . | . . . | . . . | . . . |
| Industry | ||||
| Agriculture, fishing, forestry | 0.72 | 0.52–0.99 | 1.19 | 0.80–1.75 |
| Mining | 1.42 | 1.18–1.73 | 1.27 | 1.07–1.52 |
| Construction | 1.17 | 1.01–1.35 | 1.00 | 0.86–1.17 |
| Nondurable manufacturing | 1.02 | 0.85–1.24 | 0.94 | 0.77–1.14 |
| Durable manufacturing | 1.15 | 0.96–1.37 | 1.17 | 0.97–1.41 |
| Transportation | 0.99 | 0.85–1.16 | 1.03 | 0.88–1.21 |
| Wholesale | 1.02 | 0.84–1.24 | 1.02 | 0.82–1.24 |
| Retail | 1.10 | 0.96–1.26 | 1.07 | 0.93–1.24 |
| Finance, insurance, real estate | 0.96 | 0.75–1.24 | 1.09 | 0.95–1.34 |
| Services | 1.04 | 0.90–1.21 | 1.00 | 0.86–1.18 |
| Health | 1.20 | 1.03–1.40 | 1.09 | 0.92–1.29 |
| Law, education, social services | 0.92 | 0.80–1.45 | 1.05 | 0.90–1.22 |
| Government (reference group) | . . . | . . . | . . . | . . . |
| SOURCE: Authors' analysis of New Mexico workers' compensation claims from 1994 through 2000 matched to Social Security administrative data. | ||||
| NOTES: Estimates are stratified by age. Because we stratified by age, no hazard ratios are estimated for age groups.
. . . = not applicable.
|
||||
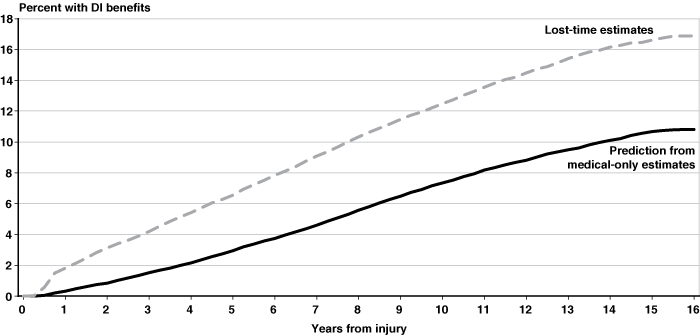
To simulate the counterfactual—what would have happened if workers with lost-time injuries instead had medical-only injuries—we predicted the hazard from the medical-only proportional hazards estimate, using the covariates of the lost-time cases. We display the estimated curves reflecting length of time from injury to initial receipt of DI benefits in Chart 4.16 The Cox model estimates for both lost-time and medical-only cases are similar to the corresponding Kaplan-Meier estimates (Chart 2), although somewhat higher.
Cox proportional hazards estimates of the impact of lost-time injuries on the receipt of DI benefits
| Years from injury | Prediction from medical-only estimates | Lost-time estimates |
|---|---|---|
| 0 | 0.00 | 0.00 |
| 0.25 | 0.01 | 0.03 |
| 0.5 | 0.05 | 0.57 |
| 0.75 | 0.21 | 1.50 |
| 1 | 0.33 | 1.82 |
| 1.25 | 0.48 | 2.14 |
| 1.5 | 0.61 | 2.46 |
| 1.75 | 0.75 | 2.83 |
| 2 | 0.85 | 3.12 |
| 2.25 | 1.01 | 3.39 |
| 2.5 | 1.19 | 3.62 |
| 2.75 | 1.33 | 3.90 |
| 3 | 1.51 | 4.19 |
| 3.25 | 1.67 | 4.53 |
| 3.5 | 1.82 | 4.86 |
| 3.75 | 1.99 | 5.14 |
| 4 | 2.16 | 5.41 |
| 4.25 | 2.35 | 5.73 |
| 4.5 | 2.56 | 6.04 |
| 4.75 | 2.74 | 6.27 |
| 5 | 2.95 | 6.56 |
| 5.25 | 3.19 | 6.94 |
| 5.5 | 3.38 | 7.22 |
| 5.75 | 3.58 | 7.52 |
| 6 | 3.73 | 7.84 |
| 6.25 | 3.97 | 8.12 |
| 6.5 | 4.18 | 8.40 |
| 6.75 | 4.37 | 8.76 |
| 7 | 4.61 | 9.09 |
| 7.25 | 4.84 | 9.37 |
| 7.5 | 5.08 | 9.67 |
| 7.75 | 5.31 | 10.01 |
| 8 | 5.57 | 10.33 |
| 8.25 | 5.81 | 10.63 |
| 8.5 | 6.04 | 10.89 |
| 8.75 | 6.27 | 11.18 |
| 9 | 6.48 | 11.47 |
| 9.25 | 6.72 | 11.74 |
| 9.5 | 6.92 | 11.94 |
| 9.75 | 7.16 | 12.21 |
| 10 | 7.34 | 12.48 |
| 10.25 | 7.52 | 12.73 |
| 10.5 | 7.76 | 13.03 |
| 10.75 | 7.93 | 13.28 |
| 11 | 8.17 | 13.55 |
| 11.25 | 8.35 | 13.83 |
| 11.5 | 8.51 | 14.05 |
| 11.75 | 8.68 | 14.20 |
| 12 | 8.82 | 14.49 |
| 12.25 | 9.03 | 14.72 |
| 12.5 | 9.22 | 14.88 |
| 12.75 | 9.36 | 15.13 |
| 13 | 9.49 | 15.41 |
| 13.25 | 9.60 | 15.63 |
| 13.5 | 9.81 | 15.84 |
| 13.75 | 9.98 | 15.96 |
| 14 | 10.10 | 16.15 |
| 14.25 | 10.23 | 16.27 |
| 14.5 | 10.43 | 16.43 |
| 14.75 | 10.55 | 16.45 |
| 15 | 10.67 | 16.62 |
| 15.25 | 10.75 | 16.74 |
| 15.5 | 10.78 | 16.85 |
| 15.75 | 10.80 | 16.89 |
| 16 | 10.80 | 16.89 |
With the exception of the youngest age group (15–24), the probability of DI receipt averages about twice as high for lost-time cases as for medical-only cases over the 9 to 15 postinjury years we observe. Moreover, the impact of a lost-time injury seems to be about the same as the impact of a 10-year increase in age. This can be seen by comparing the medical-only cumulative hazard function for an age group with the lost-time cumulative hazard function of the preceding age group (for example, lost-time cases for the 25–34 group closely match medical-only cases for the 35–44 group). We also see this in Table 3, which shows the 15-year cumulative probability of receiving DI benefits for medical-only and lost-time cases by age group.
| Age group | Medical-only cases | Lost-time cases |
|---|---|---|
| 15–24 | 3.0 | 4.9 |
| 25–24 | 5.5 | 10.1 |
| 35–44 | 10.9 | 20.0 |
| 45–54 | 20.3 | 34.4 |
| SOURCE: Authors' analysis of New Mexico workers' compensa-tion claims from 1994 through 2000 matched to Social Security administrative data. | ||
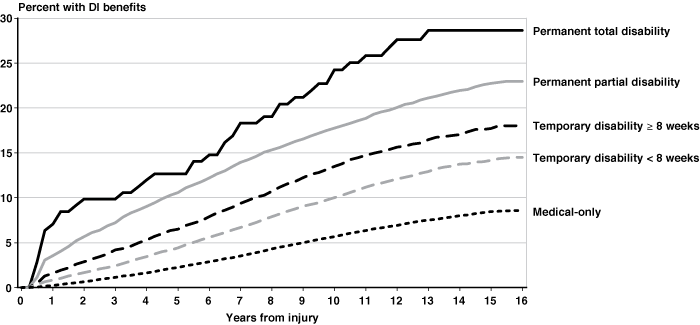
Lost-time cases cover a broad range, from workers who were off work for only 8 days and returned without any documented continuing work-related disability to those who were declared permanently and totally disabled. To see the extent to which workers' compensation disability categories were associated with DI receipt, we estimated Cox models separately for four workers' compensation lost-time severity groups and for medical-only cases, again stratifying within the model for age group (Chart 5). We found that increasing workers' compensation severity was associated with a higher cumulative probability of DI receipt. However, two of the severity groups had excess risks that differed from our prior expectations. First, even the lost-time group with less than 8 weeks of temporary disability benefits had a substantially greater probability of receiving DI benefits than did the medical-only group. Second, the group classified by the New Mexico workers' compensation system as permanently and totally disabled had less than a 30 percent probability of DI receipt, even 15 years postinjury. Because there were only 137 injured workers from our sample with PTDs, estimates for that group are imprecise.
Cox proportional hazards estimates of the impact of lost-time injuries on the receipt of DI benefits, by workers' compensation severity group
| Years from injury | Permanent total disability | Permanent partial disability | Temporary disability at least 8 weeks | Temporary disability less than 8 weeks | Medical only |
|---|---|---|---|---|---|
| 0 | 0.00 | 0.00 | 0.00 | 0.00 | 0.00 |
| 0.25 | 0.00 | 0.05 | 0.04 | 0.02 | 0.00 |
| 0.5 | 2.85 | 1.12 | 0.45 | 0.30 | 0.04 |
| 0.75 | 6.35 | 3.05 | 1.30 | 0.65 | 0.15 |
| 1 | 7.06 | 3.56 | 1.59 | 0.83 | 0.23 |
| 1.25 | 8.47 | 4.06 | 1.93 | 1.04 | 0.33 |
| 1.5 | 8.47 | 4.58 | 2.20 | 1.28 | 0.45 |
| 1.75 | 9.17 | 5.20 | 2.61 | 1.47 | 0.55 |
| 2 | 9.87 | 5.65 | 2.87 | 1.68 | 0.63 |
| 2.25 | 9.87 | 6.12 | 3.18 | 1.87 | 0.76 |
| 2.5 | 9.87 | 6.40 | 3.45 | 2.07 | 0.91 |
| 2.75 | 9.87 | 6.87 | 3.75 | 2.22 | 1.01 |
| 3 | 9.87 | 7.23 | 4.18 | 2.42 | 1.14 |
| 3.25 | 10.57 | 7.84 | 4.36 | 2.69 | 1.27 |
| 3.5 | 10.57 | 8.30 | 4.61 | 2.94 | 1.38 |
| 3.75 | 11.27 | 8.66 | 4.97 | 3.21 | 1.50 |
| 4 | 11.96 | 9.03 | 5.28 | 3.43 | 1.64 |
| 4.25 | 12.66 | 9.44 | 5.70 | 3.73 | 1.79 |
| 4.5 | 12.66 | 9.90 | 5.99 | 3.99 | 1.96 |
| 4.75 | 12.66 | 10.27 | 6.33 | 4.14 | 2.10 |
| 5 | 12.66 | 10.56 | 6.51 | 4.43 | 2.24 |
| 5.25 | 12.66 | 11.09 | 6.90 | 4.75 | 2.43 |
| 5.5 | 14.05 | 11.45 | 7.18 | 5.02 | 2.57 |
| 5.75 | 14.05 | 11.78 | 7.46 | 5.32 | 2.73 |
| 6 | 14.75 | 12.21 | 7.90 | 5.59 | 2.86 |
| 6.25 | 14.75 | 12.64 | 8.32 | 5.85 | 3.04 |
| 6.5 | 16.16 | 12.98 | 8.62 | 6.13 | 3.20 |
| 6.75 | 16.88 | 13.47 | 8.96 | 6.43 | 3.33 |
| 7 | 18.31 | 13.93 | 9.38 | 6.67 | 3.52 |
| 7.25 | 18.31 | 14.23 | 9.72 | 6.95 | 3.71 |
| 7.5 | 18.31 | 14.63 | 10.08 | 7.24 | 3.89 |
| 7.75 | 19.02 | 15.07 | 10.29 | 7.59 | 4.09 |
| 8 | 19.02 | 15.33 | 10.73 | 7.90 | 4.29 |
| 8.25 | 20.43 | 15.58 | 11.17 | 8.19 | 4.48 |
| 8.5 | 20.43 | 15.93 | 11.55 | 8.49 | 4.66 |
| 8.75 | 21.17 | 16.29 | 11.82 | 8.75 | 4.83 |
| 9 | 21.17 | 16.54 | 12.24 | 9.06 | 5.00 |
| 9.25 | 21.92 | 16.90 | 12.60 | 9.26 | 5.19 |
| 9.5 | 22.68 | 17.17 | 12.81 | 9.45 | 5.35 |
| 9.75 | 22.68 | 17.48 | 13.14 | 9.73 | 5.53 |
| 10 | 24.23 | 17.76 | 13.50 | 10.00 | 5.68 |
| 10.25 | 24.23 | 18.01 | 13.80 | 10.29 | 5.84 |
| 10.5 | 25.03 | 18.29 | 14.22 | 10.58 | 6.03 |
| 10.75 | 25.03 | 18.58 | 14.45 | 10.87 | 6.19 |
| 11 | 25.85 | 18.83 | 14.72 | 11.18 | 6.36 |
| 11.25 | 25.85 | 19.30 | 14.94 | 11.44 | 6.53 |
| 11.5 | 25.85 | 19.58 | 15.15 | 11.64 | 6.66 |
| 11.75 | 26.72 | 19.75 | 15.37 | 11.85 | 6.80 |
| 12 | 27.61 | 20.05 | 15.63 | 12.07 | 6.93 |
| 12.25 | 27.61 | 20.41 | 15.74 | 12.29 | 7.10 |
| 12.5 | 27.61 | 20.53 | 15.97 | 12.47 | 7.26 |
| 12.75 | 27.61 | 20.89 | 16.09 | 12.73 | 7.39 |
| 13 | 28.61 | 21.11 | 16.45 | 12.93 | 7.51 |
| 13.25 | 28.61 | 21.31 | 16.74 | 13.20 | 7.61 |
| 13.5 | 28.61 | 21.54 | 16.79 | 13.39 | 7.76 |
| 13.75 | 28.61 | 21.75 | 16.91 | 13.53 | 7.87 |
| 14 | 28.61 | 21.96 | 17.04 | 13.74 | 7.99 |
| 14.25 | 28.61 | 22.05 | 17.34 | 13.80 | 8.08 |
| 14.5 | 28.61 | 22.36 | 17.59 | 13.96 | 8.23 |
| 14.75 | 28.61 | 22.60 | 17.59 | 14.02 | 8.35 |
| 15 | 28.61 | 22.74 | 17.70 | 14.15 | 8.45 |
| 15.25 | 28.61 | 22.83 | 18.00 | 14.36 | 8.51 |
| 15.5 | 28.61 | 22.96 | 18.00 | 14.42 | 8.54 |
| 15.75 | 28.61 | 22.96 | 18.00 | 14.52 | 8.57 |
| 16 | 28.61 | 22.96 | 18.00 | 14.52 | 8.57 |
Discussion and Conclusions
This study offers a new perspective on the relationship between work-related disability and DI. We begin with people who experienced injuries at work and who qualified for workers' compensation benefits. In this population, only 21 percent was considered to have permanent disabilities, and only 0.5 percent was considered permanently and totally disabled. We then examined whether our sample population incurred an increased risk of long-term total disability, as measured by receipt of DI benefits. We found that a lost-time workplace injury doubled the probability of receiving DI benefits over the 9 to 15 year follow-up period. By 10 years after injury, 6 percent of workers with medical-only injuries had received DI benefits compared with 12 percent of workers with lost-time injuries (Chart 2). From this new perspective, we also see the aging effect of disability in a new way. Research has shown that older workers with mounting physical or mental limitations tend to regard disability benefits as an early retirement option (see for example, Bound and Burkhauser (1999)). What we find here is that a workplace injury affects transition to DI in a consistent manner across all age groups: Workers with injuries in one age group have a pattern of DI risk that mimics noninjured workers in the next older group. That is, the impact of a lost-time injury on the transition to DI is virtually the same as aging by 10 years.
These findings suggest that the rates of long-term total disability associated with workplace injuries are substantial. In particular, injured workers incur long-term total disability more often than could reasonably be inferred from the 0.5 percent of lost-time cases classified as permanent and total by workers' compensation. It is possible that, by including all lump-sum cases as PPD, some PTD cases that were settled with a lump-sum payment were misclassified as PPD, but this quite likely explains at most a small fraction of the disparity we have seen between medical-only and lost-time cases. Another possible explanation for our findings is that there are delayed impacts of injury on health. Work-related disability may interact with other health problems that develop over time to intensify functional limitations and affect employability. Alternatively, changing labor market conditions or other exogenous factors could lead to job loss, after which the limitations caused by the injury could make it more difficult to find a new job. Both of these explanations may be distant in time from the original injury and hard to link causally. Nevertheless, they may well be the long-term consequences of workplace injury.
It may appear counter-intuitive that even workers who had not received permanent disability benefits—even those receiving temporary disability benefits for less than 8 weeks—had an excess cumulative probability of receiving DI benefits. There are several possible reasons for this finding. One is that some people in this group experienced long-term impairments, but did not receive permanent disability benefits. Another is that the injury or the subsequent workers' compensation experience led some people in this group to miss a raise or promotion or to lose their jobs, with subsequent long-term loss of competitiveness in the labor market. Future employment or health shocks might then make it more difficult to remain employed. Studies of lost earnings of workers injured in Washington state and Wisconsin provide evidence of long-term losses consequent to injuries classified as temporarily disabling (Boden, Reville, and Biddle 2005).
For temporary and permanent total disability workers' compensation cases, there has long been agreement that the adequacy benchmark is two-thirds of pretax earnings (National Commission on State Workmen's Compensation Laws 1972). A consensus document promulgated by the Council of State Governments (1974)—the Model Act, revised—specifies pretax replacement rates of 55 percent to 65 percent for PPDs, a standard used in a recent book by the National Academy of Social Insurance (Hunt 2004).
Recent studies estimating the proportion of lost earnings replaced by workers' compensation for long-term temporary disability and PPD cases consistently show workers' compensation replacing well under half of long-term losses. Those studies include Boden and Galizzi (1999), Reville (1999), and Reville and others (2001). Delayed poor labor market outcomes could also partially explain why workers' compensation replaces only a small fraction of lost earnings. Disability determination typically occurs within 1 or 2 years postinjury. In many cases, claimants have agreed to settle their PPD claims and, once settled, they cannot reopen them. Injured workers who have not settled their claims may not be aware that they can request additional benefits if their long-term losses are greater than initially expected. Finally, it may be extremely difficult to demonstrate the relationship between the injury and labor market difficulties that occur years in the future. As a consequence, workers' compensation systems are unlikely to adjust benefits for such delayed effects of injury.
Delayed postinjury effects raise concern about the design of workers' compensation benefits: Perhaps workers' compensation agencies should reexamine benefit payments several years after the initial benefit determination. In circumstances where earnings are much lower than originally anticipated, the agencies could consider the possible link to the workplace injury. If a link is established, then the agencies could increase cash benefits commensurate with the updated unexpected earnings losses.
Currently, however, workers' compensation often provides replacement levels that fall short of its own ideals. In those cases, DI potentially acts as backup insurance, reducing the financial burden of the long-term consequences of workplace injuries on the most severely disabled. This is an important contribution to the welfare of those individuals with disabilities. However, it also implies that the replacement levels for workers' compensation may be providing suboptimal incentives to minimize work injuries. Employers, who are in the best position to improve workplace safety, do not bear the full costs of those injuries and therefore have a reduced incentive for prevention. Instead, employers shift some of the costs to workers and to the DI program, which workers and employers fund through payroll taxes that are not risk adjusted. This implies that current incentives for workplace safety and return-to-work policies operating through workers' compensation are inadequate. Moreover, the scale of this inadequacy is potentially quite large.
Our analysis shows that workers' compensation lost-time injuries are responsible for about half of all new DI awards for the workers who incurred those injuries. Our data included an average of 4,600 lost-time New Mexico cases per year, of which about 700 ended up on the DI rolls. Because half of these cases can be attributed to New Mexico lost-time injuries, we can say lost-time injuries in the state generally increased DI receipt by 350 cases per year. Comparing these figures to Social Security published statistics, we find that on average, these new awards represented 7 percent of all new DI awards in New Mexico over the relevant years they could occur (SSA, various issues, 1995–2010).17
If this New Mexico experience holds on average for other years and for the rest of the country, then 7 percent of the roughly 1 million new DI beneficiaries in 2010 (SSA 2011a, Table 35) would be due to workers compensation injuries. That would amount to 70,000 new DI awardees in 2010. Annual benefits averaged $13,500 for workers in 2010 (SSA 2011a, Table 36). Newsome and Parent (2008) found that, primarily because of offsets, benefits for people who receive workers' compensation or public disability benefits (PDBs) were about 6 percent lower than for other beneficiaries.18 Applying that reduction to 2010 benefit levels implies an estimated first-year additional cost of $889 million to Social Security because of workers' compensation injuries. Further, Social Security actuarial estimates suggest that for DI beneficiaries with our gender mix and our average DI starting age of 47, we can expect new beneficiaries that come from workers' compensation injuries to remain on the DI rolls for 13½ years (Zayatz 2011, Tables 24A and 24B). Given that the typical discount rate used for federal DI benefits is more than offset by cost-of-living increases in benefit levels, a conservative present value estimate of DI benefit costs related to workers compensation injuries is roughly $12 billion for each new annual cohort. Adding Medicare costs would nearly double that figure.
Because we do not know whether the New Mexico experience for injuries from the 1990s is representative of the rest of the country or more recent spans of time, we present the previous figures only to be illustrative. Still, those figures demonstrate that the significant size of these programs means that the impact of workplace injuries on DI costs is likely to be substantial.
Given these potentially large costs, there may be a need for additional programs that reward employers for injury prevention or that otherwise help to reduce the delayed effects of injuries for workers of all ages. Autor and Duggan (2010) recently proposed a mandated private disability insurance program that would cover both occupational and nonoccupational disabilities. This program would provide wage-replacement benefits and extra incentives for compliance with workplace accommodations mandated by the Americans with Disabilities Act and for vocational rehabilitation. It would begin 90 days after the onset of disability. For workplace injuries, this program would seem to duplicate some of the features of workers' compensation and present problems of integration (for example, integration of wage-replacement benefits).
Oregon has two programs designed to improve retention, return to work, and hiring of injured workers. All Oregon workers with accepted claims are eligible for the Employer-at-Injury Program (EAIP). The program subsidizes employers who offer modified or light-duty jobs to get people back to work. Employers are also eligible for a wage subsidy of 50 percent of preinjury wages or 50 percent of wages in the modified job, whichever is less. The subsidy is available for up to 66 work days. The EAIP also reimburses employers for worksite modification and for tools, equipment, and clothing not usually supplied by the employer. Oregon's Preferred Worker Program (PWP) provides incentives to hire permanently disabled workers who cannot return to regular employment (Department of Consumer and Business Services, Oregon, n.d.). Employers hiring workers enrolled in the PWP can receive 50 percent of wage reimbursement for up to 6 months and up to $25,000 for tools, equipment, and redesign of the work site. Also, employers pay no workers' compensation premiums for preferred workers. In addition, if preferred workers have new workers' compensation claims during the 3 years after they enroll in the PWP, the program reimburses all related costs. No studies have been done to determine whether these programs are effective, and perhaps such studies might be a first step in determining whether comparable programs would be justified in other states.
Washington State has a PWP that is similar to Oregon's. Also, in 2011, Washington initiated its Stay at Work program, which covers injured workers released to restricted work activity by their health-care providers. For workers assigned to light-duty jobs, this program reimburses employers for up to half of the injured workers' wages and for the cost of training, tools, and clothing needed for those jobs.
Our findings also make a case for increased research on and incentives for the prevention of workplace injuries and illnesses. Workers' compensation premiums may provide prevention incentives (Tompa, Trevithick, and McLeod 2007), but benefit levels and access to benefits have been a concern for several decades (Burton and Spieler 2001). As a result, US employer costs per $100 of payroll in 2008 were only 61 percent of what they were in 1990 (Sengupta, Reno, and Burton 2011). Another avenue to reduce workplace injuries and illnesses is strengthening and providing more resources for workplace safety regulation. The resources of the Occupational Safety and Health Administration are very limited compared with the number of workplaces it is tasked with inspecting.
There are some limitations of the current study. We have analyzed data from only one state, so we do not know whether the results will hold in other states with different labor market conditions and workers' compensation systems. In addition, we have used workers with medical-only injuries as controls, implicitly assuming that those relatively minor injuries have no long-term consequences on disability. Also, a number of potential confounders, like education and preinjury health status, are not available in our data. Still, this analysis provides a first step toward enhancing our understanding of the issue, and we plan to address these limitations in future studies.
Finally, this study only addresses injuries for which workers' compensation benefits were paid. Studies have consistently shown that many injured workers do not receive workers' compensation benefits (Burton and Spieler 2001; Azaroff, Levenstein, and Wegman 2002; Rosenman and others 2006; Boden and Ozonoff 2008; Bonauto and others 2010). Moreover, Reville and Schoeni (2004) found that 29 percent of people aged 51–61 with a disabling work injury reported receiving DI benefits at their time of interview, but only 12 percent had ever received workers' compensation benefits. For injured workers who never receive workers' compensation benefits, DI effectively becomes the sole social insurance program for occupational injuries and illnesses.
Notes
1 Social Security insures individuals for disabled-worker benefits, if they have worked long enough and recently enough in Social Security–covered employment. The number of work credits (also known as quarters of coverage) a person needs to qualify for benefits depends on the individual's age at disability onset. Generally, an individual needs 40 work credits, of which he or she must earn 20 in the 10 years ending with the year of disability onset. Younger workers may qualify with fewer credits. A person can earn up to four work credits per year. The amount of earnings required for a credit increases each year as general wage levels increase. In 1994, one work credit was earned for each $620 in annual covered earnings, up to a maximum of four credits annually. In 2010, workers could earn one work credit for each $1,120 in covered earnings.
2 In most states, SSA reduces DI benefits so that the combined Social Security and workers' compensation benefits do not exceed 80 percent of prior earnings. However, in 15 "reverse offset" states, the workers' compensation program reduces the benefit to meet the 80 percent rule.
3 This excludes disabled widow(er)s and adult disabled children, as well as benefits to nondisabled dependents. Total DI benefits paid to disabled workers is our calculation (SSA 2011a, Table 3). Costs for "disabled persons" in 2008 were $54.0 billion for hospital and medical insurance combined (SSA 2011b, Table 8B2).
4 For DI workers only, data based on authors' calculations using SSA (2011a, Table 3).
5 For descriptions of these workers' compensation changes, see Burton and Spieler (2001), Boden and Ruser (2003), and Spieler and Burton (2012).
6 In December 1999, the Government Accountability Office reported, "Thus far, SSA has been able to obtain on-line access to State WC data in just five States," http://oig.ssa.gov/sites/default/files/audit/full/pdf/A-04-98-64002.pdf (p. iii). These are not batch data matches, but rather states where SSA has some limited online access to workers' compensation information. The only batch match SSA has conducted with a state was a two-phase match with Texas workers' compensation data in September 2001 and March 2002. The match worked, but encountered several problems with the data structure, format, and completeness (based on internal SSA correspondence, December 14, 2011).
7 This marginally increases the proportion of workers with multiple injuries to 23 percent.
8 See Olsen and Hudson (2009). SSA maintains the MEF subject to IRS disclosure rules as detailed in Section 6103 of the Internal Revenue Code. Consistent with those rules, only SSA employees had access to individual DER records for this project.
9 SSA initially developed the TRF to support SSA's evaluation of the Ticket to Work program, but TRF data are useful for a broad range of disability/employment topics.
10 Although we only include individuals who received DI from 1996 forward, we know the start dates for those who began receiving benefits before 1996. This raises the possibility that we might miss those who both started and terminated benefits between 1994 and 1996. Such exits could only occur because of transition to Social Security retirement, medical recovery, or death. Because we exclude workers aged 55 or older at the date of injury, we do not lose anyone to Social Security retirement. Because of work incentives, no one could terminate because of work within such a short time frame. In only a minority of cases, where SSA expects to see medical improvement, does the agency review medical eligibility within 3 years of awarding benefits. These are the only cases that could lead to a termination for medical recovery. For those people who started receiving benefits between 1996 and 2009, only six had a medical termination within 24 months, and, at most, two had such a termination in any 2-year period. A medical termination by 1996 for those who started receiving benefits between 1994 and 1996 is thus very unlikely. After applying our other data restrictions, we found that no workers injured between 1994 and 1996 had died before 1996.
11 This eligibility date differs from the date insured status began and may also differ from the first DI benefit date. SSA determines insured status based on the individual's quarters of coverage over his or her work history. To be eligible for cash benefits, the individual must be both insured and disabled under the SSA disability definition. Because of processing lags, the agency often pays initial cash benefits after the date of eligibility. In such cases, the first payment SSA makes to the beneficiary will include retroactive payments back to the initial eligibility date.
12 The NUMIDENT file includes information received from family members and other sources including funeral director reports, all state and territorial bureaus of vital statistics, and the Veterans Administration.
13 We examined the sensitivity of our results to restricting the medical-only injury group to people with a single medical-only injury. This led to virtually no difference in our results.
14 SAS 9.2 (2002-2003, SAS Institute, Cary, NC).
15 We use SAS Proc Phreg to derive the cumulative hazard curves for the lost-time cases. Because it is not possible to plot survival curves directly through this procedure, we use the baseline option to output a data set for the survival function from which we produce survival functions for specific covariate patterns.
16 In fact, using the medical-only covariates would have made virtually no difference in the cumulative hazard curves. At all observed durations, the predicted medical-only curve using lost-time covariates differed by less than 0.3 percent from the curve using medical-only characteristics (not shown).
17 For the proportion of new DI cases that are due to lost-time injuries each year, we divide the attributable injuries for a given year by the average DI awards over the period such awards occurred. Thus for 1994 injuries, we divide by the average DI awards in New Mexico for the 1994–2009 period, while for injuries in 2000, we divide by the average DI awards for the 2000–2009 period.
18 Newsome and Parent (2008) found that about 11 percent of all DI beneficiaries with initial entitlement dates from January 2003 through June 2004 also received workers' compensation or PDBs. (Per SSA (2011a, Table 31), we also know that about 85 percent of such beneficiaries are those with state workers' compensation benefits.) On average, beneficiaries who receive workers' compensation or PDBs have higher average indexed monthly earnings, but because of the offset provision, those who receive workers' compensation or PDBs received initial benefits that were 94 percent of the benefits of those without workers' compensation or PDBs ($916 as compared with $983 for the 2003–2004 period examined).
References
Autor, David H., and Mark G. Duggan. 2006. "The Growth in the Social Security Disability Rolls: A Fiscal Crisis Unfolding." Journal of Economic Perspectives, American Economic Association 20(3): 71–96 (Summer).
———. 2010. Supporting Work: A Proposal for Modernizing the U.S. Disability Insurance System. Washington, DC: Center for American Progress and The Hamilton Project (December).
Azaroff, Lenore S., Charles Levenstein, and David H. Wegman. 2002. "Occupational Injury and Illness Surveillance: Conceptual Filters Explain Underreporting." American Journal of Public Health 92(9): 1421–1429.
Barth, Peter S., and Michael Niss. 1999. Permanent Partial Disability Benefits: Interstate Differences. Cambridge, MA: Workers Compensation Research Institute.
Boden, Leslie I., and Monica Galizzi. 1999. "Economic Consequences of Workplace Injuries and Illnesses: Lost Earnings and Benefit Adequacy." American Journal of Industrial Medicine 36(5): 487–503.
Boden, Leslie I., and Al Ozonoff. 2008. "Capture-Recapture Estimates of Nonfatal Workplace Injuries and Illnesses." Annals of Epidemiology 18(6): 500–506.
Boden Leslie I., Robert T. Reville, and Jeff Biddle. 2005. "The Adequacy of Workers' Compensation Cash Benefits." In Workplace Injuries and Diseases: Prevention and Compensation: Essays in Honor of Terry Thomason, edited by Karen Roberts, John F. Burton Jr., and Matthew M. Bodah, 37–68. Kalamazoo, MI: W. E. Upjohn Institute for Employment Research.
Boden, Leslie I., and John W. Ruser. 2003. "Workers' Compensation 'Reforms,' Choice of Medical Care Provider, and Reported Workplace Injuries." Review of Economics and Statistics 85(4): 923–929.
Bonauto, David K., Joyce Z. Fan, Thomas W. Largo, Kenneth D. Rosenman, Mandy K. Green, Jaime K. Walters, Jennifer Flattery, and others. 2010. "Proportion of Workers Who Were Work-Injured and Payment by Workers' Compensation Systems—10 States, 2007." Morbidity and Mortality Weekly Report 59(29): 897–900.
Bound, John, and Richard V. Burkhauser. 1999. "Economic Analysis of Transfer Programs Targeted on People With Disabilities." In chapter 51 of Handbook of Labor Economics, ed. 1, vol. 3, no. 3, edited by O. Ashenfelter and D. Card, 3417–3528. North-Holland: Elsevier.
Burkhauser, Richard V., and Mary C. Daly. 2002. "Policy Watch: U.S. Disability Policy in a Changing Environment." The Journal of Economic Perspectives 16(1): 213–224.
Burton, John F., Jr. 2005. "Permanent Partial Disability Benefits." In Workplace Injuries and Diseases: Prevention and Compensation: Essays in Honor of Terry Thomason, edited by Karen Roberts, John F. Burton Jr., and Matthew M. Bodah, 69–116. Kalamazoo, MI: W. E. Upjohn Institute for Employment Research.
Burton, John F., Jr., and Emily A. Spieler. 2001. "Workers' Compensation and Older Workers." In Ensuring Health and Income Security for An Aging Workforce, edited by Peter P. Budetti, Richard V. Burkhauser, Janice M. Gregory, H. Allan Hunt, 41–83. Kalamazoo, MI: W. E. Upjohn Institute for Employment Research.
Council of State Governments. 1974. Workmen's Compensation and Rehabilitation Law (Revised). Lexington, KY: Council of State Governments.
Department of Consumer and Business Services, Oregon. n.d. Preferred Worker Program. Salem, OR: Workers' Compensation Division. http://www.cbs.state.or.us/wcd/rdrs/rau/pwp/top_pwp.pdf.
Guo, Xuguang (Steve), and John F. Burton Jr. 2008. "The Relationship Between Workers' Compensation and Disability Insurance." In Labor and Employment Relations Association Series: Proceedings of the 60th Annual Meeting, edited by Adrienne E. Eaton, 25–32. Champlain, IL: Labor and Employment Relations Association.
Hunt, H. Allan, ed. 2004. Adequacy of Earnings Replacement in Workers' Compensation Programs: A Report of the Study Panel on Benefit Adequacy of the Workers' Compensation Steering Committee, National Academy of Social Insurance. Kalamazoo, MI: W. E. Upjohn Institute for Employment Research.
Leigh, J. Paul, Steven B. Markowitz, Marianne Fahs, Philip J. Landrigan. 2000. Costs of Occupational Injuries and Illnesses. Ann Arbor MI: University of Michigan Press.
McInerney, Melissa P., and Kosali I. Simon. 2012. "The Effect of State Workers' Compensation Program Changes on the Use of Federal Social Security Disability Insurance." Industrial Relations 51(1): 57–88 (January).
National Commission on State Workmen's Compensation Laws. 1972. The Report of the National Commission on State Workmen's Compensation Laws. Washington, DC: Government Printing Office.
Newsome, Ronda, and Rene Parent. 2008. "Characteristics of Disabled-Worker Beneficiaries Receiving Workers' Compensation or Public Disability Benefits Compared With Disabled-Worker Beneficiaries Without These Additional Benefits." Research and Statistics Note No. 2008-01. http://www.socialsecurity.gov/policy/docs/rsnotes/rsn2008-01.html.
Olsen, Anya, and Russell E. Hudson. 2009. "Social Security Administration's Master Earnings File: Background Information." Social Security Bulletin 69(3): 29–45.
Reno, Virginia, Cecili Thompson Williams, and Ishita Sengupta. 2003. "Workers' Compensation, Social Security Disability Insurance, and the Offset: A Fact Sheet." Social Security Bulletin 65(4): 3–6.
Reville, Robert T. 1999. "The Impact of a Disabling Workplace Injury on Earnings and Labor Force Participation." In The Creation and Analysis of Linked Employer-Employee Matched Data, Contributions to Economic Analysis, edited by J. C. Haltiwanger and others, 147–173. New York: Elsevier Science, North-Holland.
Reville, Robert T., Leslie I. Boden, Jeff E. Biddle, and Christopher Mardesich. 2001. An Evaluation of New Mexico Workers' Compensation Permanent Partial Disability and Return to Work. RAND Monograph Report. Santa Monica, CA: RAND Corporation.
Reville, Robert T., and Robert F. Schoeni. 2004. "The Fraction of Disability Caused at Work." Social Security Bulletin 65(4): 31–37.
Rosenman, Kenneth D., Alice Kalush, Mary Jo Reilly, Joseph C. Gardiner, Mat Reeves, and Zhehui Luo. 2006. "How Much Work-Related Injury and Illness Is Missed by the Current National Surveillance System?" Journal of Occupational and Environmental Medicine 48(4): 357–365.
Rupp, Kalman, and David C. Stapleton. 1995. "Determinants of the Growth in the Social Security Administration's Disability Programs—An Overview." Social Security Bulletin 58(4): 43–70.
Sengupta, Ishita, Virginia Reno, and John F. Burton Jr. 2011. Workers' Compensation: Benefits, Coverage, and Costs, 2009. Washington, DC: National Academy of Social Insurance.
Smith, Gordon S., Helen M. Wellman, Gary S. Sorock, Margaret Warner, Theodore K. Courtney, Glenn S. Pransky, and Lois A. Fingerhut. 2005. "Injuries at Work in the US Adult Population: Contributions to the Total Injury Burden." American Journal of Public Health 95(7): 1213–1219
[SSA] Social Security Administration. Various issues, 1995–2010. Annual Statistical Supplement to the Social Security Bulletin, [1994–2009]. Washington DC: Office of Retirement and Disability Policy, Office of Research, Evaluation, and Statistics.
———. 2011a. Annual Statistical Report on the Social Security Disability Insurance Program, 2010. Washington, DC: Office of Retirement and Disability Policy, Office of Research, Evaluation, and Statistics.
———. 2011b. Annual Statistical Supplement to the Social Security Bulletin, 2010. Washington, DC: Office of Retirement and Disability Policy, Office of Research, Evaluation, and Statistics.
Spieler, Emily A., and John F. Burton Jr. 2012. "The Lack of Correspondence Between Work-Related Disability and Receipt of Workers' Compensation Benefits." American Journal of Industrial Medicine 55(6): 487–505.
Tompa, Emile, Scott Trevithick, and Christopher McLeod. 2007. "Systematic Review of the Prevention Incentives of Insurance and Regulatory Mechanisms for Occupational Health and Safety." Scandinavian Journal of Work Environment and Health 33(2): 85–95.
Zayatz Tim. 2011. "Social Security Disability Insurance Program Worker Experience." Actuarial Study No. 122. SSA Pub. No. 11-11543. Baltimore, MD: Social Security Administration, Office of the Chief Actuary.